2025 National Conference

2025 National Conference
Date: March 7-9, 2025
Location: Duke University School of Medicine, Durham, NC
Registration Details:
General Registration Waitlist
Banquet Tickets – SOLD OUT
Discounted Housing Form and Reservation – CLOSED
General Registration – SOLD OUT
Early Bird Registration and House of Delegates Registration – CLOSED
Research Abstract Submission – CLOSED
Travel Subsidy Application – TBA
In recent years, APAMSA National Conferences have embraced a forward-thinking approach while also engaging in a thorough reflection of past experiences. This dual focus has worked to bring our community together in a concerted effort to address healthcare disparities. Given the alarming rise in anti-AANHPI hate crimes and the surge in mental health crises exacerbated by the pandemic, addressing AANHPI mental health has become more critical than ever.
In line with these values, our theme for the 2025 APAMSA National Conference is: “Blossom: Healing Our Communities and Inspiring Transformation.” The stigmatization of mental health issues within AANHPI communities has often led to inadequate support, conflict, and deep hurt. Therefore, it is essential that our conference fosters open dialogue on this subject. We will explore complex issues such as intergenerational trauma, which can perpetuate cycles of mental health challenges and cultural disconnection. We will also address the need for racial healing, recognizing that historical injustices have lasting impacts on our well-being.
Additionally, we will confront the realities of burnout and moral injury, which are increasingly common among healthcare providers and community leaders. By engaging in these discussions, we aim to develop strategies and insights that will empower future healthcare providers to effect meaningful change.
Reminiscent of the iconic cherry blossom trees on Duke’s campus, our goal is to inspire a new generation of AANHPI healthcare trainees to “blossom” into providers who are not only aware of these challenges, but also equipped with the tools and empathy needed to foster transformation within our communities. Through these conversations, we hope to build a stronger, more resilient network capable of addressing both individual and systemic issues related to AANHPI mental health and healthcare equity.
Friday, March 7
Duke University School of Medicine: Trent Semans Center for Health Education
8 Searle Center Dr, Durham, NC 27710
7:30-9:00pm – Anti-Racism Caucus
Saturday, March 8
Duke University School of Medicine: Trent Semans Center for Health Education
8 Searle Center Dr, Durham, NC 27710
7:30-8:30am – Check in
8:30-9:05am – Welcome Address
9:05-9:50am – Keynote Address
10:00-10:45am – Breakout Session 1
11:00-11:45am – Breakout Session 2
11:45-12:50pm – Lunch
12:00-1:45pm – House of Delegates (HOD) Meeting
1:45-2:45pm – Poster Session, Diversity Mixer
3:00-3:45pm – Breakout Session 3
4:00-4:45pm – Breakout Session 4
5:00-5:45pm – Closing Ceremony, Election Results
6:00-7:30pm – Alumni Mixer
7:30-10:00pm – Banquet at Namu Korean Eats, Beer Hall & Coffee Bar
Sunday, March 9
Duke University School of Medicine: Trent Semans Center for Health Education
8 Searle Center Dr, Durham, NC 27710
10am-1pm ET / 7am-10 am PT – Transition Meeting for elected leadership and outgoing National Board (hybrid)
Discounted housing is now closed, but please see our guide to hotels for housing recommendations close to the conference venue!
The 2025 APAMSA National Conference has secured discounted accommodations at The Residence Inn Durham McPherson/ Duke University Medical Center Area from Friday, March 7, 2025 through Sunday, March 9, 2025. The Residence Inn is an 8 minute drive to the conference venue, the Trent Semans Center for Health Education at the Duke University School of Medicine, as well as 15 minute to downtown Durham! Shuttle services to the conference venue will be provided.
The Residence Inn Durham McPherson/ Duke University Medical Center Area: 1108 West Main Street, Durham, North Carolina, USA, 27701
Discounted housing is available on a first come, first served basis. Please register for discounted housing here by February 10th, 2025 at 11:59PM EST. To register, please fill out one form per room (max 3 people) and complete 1 reservation per room. It is your responsibility to pay for the hotel room and split the cost if relevant. Failure to do so will result in forfeiting your room and penalty on APAMSA National Conference.
If you are interested in finding a roommate, please use the conference Discord channel!
Cost: average $169/night for a King Studio Room (king bed + sofa bed)
Max Occupancy: 3 people
The 2025 APAMSA National Conference has secured discounted flights with United Airlines and Delta Airlines.
United Airlines: Please check out the infographic below for instructions on how to make your flights reservations.
United Meetings Online Instruction (1)
Delta Airlines: Please read instructions for making your flight reservations below.
Delta Air Lines is pleased to offer special discounts for APAMSA.
Please click here to book your flights. You may also call Conferences and Events® at 1.800.328.1111* Monday–Friday, 8:00 a.m. – 6:30 p.m. (EST)
Meeting Event Code: NY3EV
*Please note there is not a service fee for reservations booked and ticketed via our reservation 800 number.
Abstract submission for the Research Poster Session is open until December 31st, 2024. Sign up here!
– Poster presentations are in-person and after lunch time during the conference (Saturday, March 7th, 2025).
-Abstracts categories include: Basic Science; Translation & Clinical Health; Community Health, Epidemiology, Education, and Policy; and Healthcare Professional and Trainee Wellbeing
– At least one author will need to be available at all times to give a quick oral presentation and answer questions during this session.
– There will be judges who will be selecting for the most outstanding abstracts in each category during the abstract presentation session.
Please note:
– Abstract approval decisions will be emailed to the corresponding author.
– Upon approval of submission, presenters will need to provide a demonstration of conference ticket purchase to confirm their attendance at this poster session.
Poster Printing:
– We are happy to announce that we will have discounted poster printing in partnership with PhD Posters! Printed posters will be available for pick-up at the conference venue. Please place orders here.
– If you are printing your poster prior to arrival at the conference, please make sure it is within these dimensions: 36in (width) x 42in (height)
Feel free to contact research@apamsa.org with any questions!
Helen Heo
National Conference Logistics Director
Duke University School of Medicine
Jamie Lim
National Conference Logistics Director
Duke University School of Medicine
Katrina Hon
National Conference Speaker Relations Director
Duke University School of Medicine
Kelly Pu
National Conference Speaker Relations Director
Duke University School of Medicine
Allan Chen
National Conference Finance Director
Duke University School of Medicine
Hannah Ford
National Conference Communications Director
Duke University School of Medicine
Logistics
National Conference Committee Members
Duke University School of Medicine
Jessica Guo, Jamie Karl, Mindy Kim, Helen Heo, Jamie Lim, Nathan Sattah
Speaker Relations
National Conference Committee Members
Duke University School of Medicine
Sophia Chang, Katrina Hon, Grace Kim, Joyce Liu, Kelly Pu
Communications
National Conference Committee Member
Duke University School of Medicine
Robyn Guo, Sonia Lin, Hannah Zang, Daphne Zhu
Finance
National Conference Committee Members
Duke University School of Medicine
Allan Chen, Zikang Tan, Christian Zirbes
Thank you to our Sponsors!
For those who are interested in having an exhibitor booth at the National Conference, please contact conference@apamsa.org and CC externalvp@apamsa.org and sponsorship@apamsa.org in your email by January 25th, 2025 so that we can draft a sponsorship contract and create an invoice for you. Thank you for your interest!
Check out the National APAMSA Instagram to follow our speaker reveals and see our 2025 National Conference Booklet for the full speaker list!
Never been to Durham, North Carolina before? Come explore our city! Known as the Bull City and the City of Medicine, we hope you can experience all of the fun activities and yummy food this area has to offer!
Check our Exploring Durham Guide!

Image source: Downtown Durham Inc
Please see here for information on parking at the conference venue and transportation in Durham!
Please check back soon for more information!
ALUMNI & PHYSICIAN CONFERENCE PROGRAM
Alumni Directors’ Welcome Message:
Hello alumni/residents/physicians! This year, we are excited to announce the addition of physician-specific programming at National Conference, including our affiliate’s National Asian Physician Association (NAPA) Inaugural Roundtable Discussion, focused on professional growth for AANHPI physician leaders and community health. We hope to see you soon!
All events are specifically geared toward physicians and open to everyone.
To RSVP for in-person attendance, register for the APAMSA Conference as a Physician/Alumni link HERE: https://bit.ly/NCalumniregistration
BREAKOUT SESSION #2, 11:00 – 11:45 AM: North Carolina Asian Americans Together (NCAAT) Event
Location: Lab 5-6 (Rm 3055-3056)
As a doctor, you want to make sure that your patients are getting the best possible care. For patients who are struggling with mental health conditions, however, your passion and care for them may not be enough to overcome the systemic barriers they’re facing. Learn how you can use your position as a healthcare professional to advocate for change on personal, community, and legal support systems that lead to the best outcomes for the patients you care for. Panelists will discuss health advocacy on all levels and real-life examples and outcomes of mental health advocacy efforts in the US.
BREAKOUT SESSION #3, 3:00 – 3:45 PM: Duke/UNC Faculty Panel
Location: Learning Hall (Rm 2050)
Join a distinguished panel of faculty physicians from Duke, UNC, and Wake Forest as they share their diverse clinical, academic, and research experiences. This session will provide valuable insights on addressing Asian American stereotypes, navigating racism in clinical settings, personal relationships in medicine, pursuing leadership opportunities, and more.
BREAKOUT SESSION #4, 4:00 – 4:45 PM: National Asian Physician Association (NAPA) Roundtable Discussion
Location: Classroom 4 (Rm 4067)
For years, APAMSA alumni have envisioned a “physician version of APAMSA.” NAPA brings that vision to life by fostering connection and collaboration among Asian physicians nationwide. NAPA’s mission is to advance the health of Asian Americans and empower Asian physicians through leadership and professional development, workforce wellness, and community engagement. This inaugural roundtable is a chance to connect, share insights, and advance Asian physician representation and community health. The hybrid event is free, and light bites and drinks available to all in-person attendees.
Option to join virtually, RSVP via Zoom Registration link HERE: https://bit.ly/NAPA-NCZoom
6:00 – 7:30 PM: Alumni/Physician Mixer
Location: Namu, 5420 Durham-Chapel Hill Blvd, Durham, NC 27707
It is our pleasure to invite all residents, physicians, and alumni to the Alumni/Physician social & mixer event, free of charge, to connect with APAMSA alumni/residents/attendings from all over the country.
7:30 – 10:00 PM: Banquet
Location: Namu, 5420 Durham-Chapel Hill Blvd, Durham, NC 27707
(open to people who purchased banquet ticket)
This year’s banquet will take place at and be catered by Namu. Namu is a Korean fusion restaurant, beer hall, and coffee house and is one of The Eater’s 18 Essential Durham Restaurants.
Contact Us
Questions? Email us at conference@apamsa.org.
.
2024 Hepatitis Conference
WELCOME TO THE 18TH ANNUAL APAMSA HEPATITIS CONFERENCE!
We are happy to announce the 18th Annual Hepatitis B/C Conference will take place on Saturday, November 16, 2024 from 8 AM to 5 PM PST in San Diego, CA! The UC San Diego School of Medicine APAMSA Chapter has graciously partnered with us to put together the best conference yet! APAMSA members and non-members are all welcome to register and attend.
Each year, we strive to collectively engage in the global fight against liver diseases, including hepatitis B and C, and to raise awareness about health disparities and their impact within the Asian American, Native Hawaiian, and Pacific Islander (AANHPI) population.
The objectives of the conference are to raise awareness about the impact of liver diseases on the AANHPI community, to encourage future health care providers to advocate for policy changes to address the current health disparities that the AANHPI community face, to provide opportunities for current health profession students to network with prominent leaders in hepatology and to provide a venue for students to present their research on topics related to GI/hepatology.
Medical Education & Telemedicine Building
Ong Family Auditorium
3160 Biomedical Sciences Wy
La Jolla, CA 92093
SCHEDULE
8:00 – 8:50 AM Registration and Breakfast
9:00 – 9:10 AM Introduction & Opening Remarks by Dr. Araneta, UCSD Associate Dean of Diversity and Community Partnerships
9:10 – 10:00 AM Saira Khaderi, M.D., M.P.H.
10:10 – 11:00 AM Robert Wong, M.D., M.S., FACG, FAASLD
11:10 – 12:00 PM Wendy Lo
12:00 – 1:00 PM Lunch
1:00 – 2:00 PM Research Poster Session & Oral Presentation
2:10 – 3:00 PM Breakout Sessions
3:10 – 4:00 PM Robert Gish, M.D., FAASLD
4:00 – 4:30 PM Closing Remarks

Tzu-Hao (Howard) Lee, M.D.Assistant Professor, Baylor College of Medicine
Dr. Howard T. Lee is a gastroenterologist and transplant hepatologist at Baylor College of Medicine, Houston, Texas. He completed his medicine, gastroenterology and hepatology training at Duke. Dr. Lee’s academic and clinical interests include viral hepatitis, liver transplant and health disparities, with a special focus on the LGBTQ+ population.

Saira Khaderi, M.D., M.P.H.
Assistant Professor, Transplant Hepatology Medical Director, Baylor College of Medicine
Dr. Khaderi is a transplant hepatologist at Baylor College of Medicine in Houston, Texas and has a special interest in viral hepatitis elimination and hepatocellular carcinoma. She is the Medical Director for Project ECHO (Extension for Community Healthcare Outcomes) at Baylor St. Luke’s Medical Center (BSLMC). Project ECHO uses video conferencing to develop expert health care networks to manage complex liver diseases in underserved areas. In the past 10 years, ECHO BSLMC has treated over 2,800 patients for HCV/HBV across the United States (most of whom are uninsured). She is also on the Steering Committee for Hepatitis C Elimination in Texas, AASLD Hepatitis C SIG, and the AASLD’s Women’s Initiative Committee.

Robert J. Wong, M.D., M.S., FACG, FAASLD
Clinical Associate Professor, Stanford University School of Medicine
Robert J. Wong, MD, MS, FACG, FAASLD is a Clinical Associate Professor of Medicine in the Division of Gastroenterology and Hepatology, Stanford University School of Medicine, and staff physician at the Veterans Affairs Palo Alto Healthcare System. He is a passionate advocate and clinician-scientist whose work has focused on highlighting and addressing healthcare disparities and inequities among individuals with viral hepatitis and chronic liver diseases. Dr. Wong’s current research continues to focus on epidemiology, outcomes, and health services research in liver diseases, with particular emphasis on healthcare disparities among under-served, vulnerable, and ethnic minority populations with HBV and HDV, steatotic liver disease, and hepatocellular carcinoma. His work has been supported by the National Institute on Minority Health and Health Disparities, the National Institute on Alcohol Abuse and Alcoholism, the American Association for the Study of Liver Diseases, the American College of Gastroenterology, and others. He has authored over 250 publications and work has been published in high impact journals including, JAMA, Hepatology, Gastroenterology, Journal of Hepatology, Clinical Gastroenterology and Hepatology, and American Journal of Gastroenterology. Dr. Wong’s collaborative research, advocacy, and educational projects span broadly and includes working with AASLD, ACG, Hepatitis B Foundation, American Liver Foundation, Global Liver Institute, Chronic Liver Disease Foundation, and others. His current work in the field of HBV focuses on improving disease awareness and reducing stigma, improving implementation of universal HBV screening, expanding and simplifying HBV treatment criteria, and continuing to address existing gaps in timely linkage to care and treatment particularly among vulnerable populations.

Wendy Lo, B.A.
Advocate, Speaker, Consultant, Wendy Co Consulting, LLC
Wendy Lo is a patient advocate, speaker and consultant for liver health, patient inclusion and hepatitis elimination. After being diagnosed and living with chronic hepatitis B for nearly three decades, Wendy broke her silence by sharing her personal story openly. From patient turned advocate, she is on a mission to raise awareness, promote understanding, tackle stigma, influence policy and advance clinical research to fight the hepatitis epidemic. Her advocacy spans speaking appearances, consulting on patient engagement, community outreach, and activism for public health and policy changes.
Wendy is also a health seeker turned health coach, mindfulness practitioner and personal fitness trainer. Her previous career in the software industry spans 20+ years with roles in global education services, go-to-market strategy & execution, and information technology (IT) consulting. Visit wendylo.com for more information.

Robert Gish, M.D., FAASLD
Medical Director, Hepatitis B Foundation
Principal, Robert G. Gish Consultants, LLC
Dr. Gish is a fellow of the American Association for the Study of Liver Disease, the American Society of Transplantation and American College of Physicians.
He has served on the editorial boards of American Journal of Gastroenterology, Hepatology, Journal of Hepatology, Digestive Diseases and Sciences, and Gastroenterology, among many others. He co-authored a public health policy for liver health in Vietnam focusing on HBV and is also assisting with the development of viral hepatitis health care policies in Georgia, Armenia, and the Philippines. He was a major early contributor to decipher methods for the detection of hepatitis B and C virus and characterizing their epidemiology and clinical presentation in humans. He was involved in studies that led to the genotypic classification strategies and methods now in use worldwide. He has published more than 700 original articles, abstracts, and book chapters.
Robert G. Gish, MD, is currently the Medical Director of the Hepatitis B Foundation in Doylestown, Pennsylvania. He is an Adjunct Professor of Medicine at the University of Nevada Schools of Medicine in Las Vegas and in Reno. He serves as an Adjunct Professor of Pharmacy at Skaggs School of Pharmacy and Pharmaceutical Sciences at UCSD, a Clinical Professor of Medicine at Loma Linda University. In addition, he is the Medical Director of the American Pacific Health Foundation in San Diego, CA. Dr. Gish is currently seeing patients, both in-person and via telemedicine, at various clinics in San Diego, Folsom (El Dorado Hills), Santa Rosa, and Valley Springs. He is a staff physician at La Maestra, a federally qualified health center in San Diego. Dr. Gish also serves as a Board Member of the Viet Nam Viral Hepatitis Alliance (VVHA).
Abstract submissions for the 18th Annual APAMSA Hepatitis Conference are now open!
EXTENDED DEADLINE: November 2, 2024 at 11:59 PM PST
Thank you for your interest in submitting your research for consideration for presentation at the 18th Annual National APAMSA Hepatitis Conference. We look forward to evaluating your hard work. We prefer research to cover GI/Hepatology topics but also accept research related to AANHPI communities.
The poster session is tentatively scheduled for 1 PM to 2 PM. At least one author is required to give a presentation during this time. Poster awards will be given by our judges.
Please contact us at hepatitis@apamsa.org if you have any questions.
REGISTRATION:
To register, please fill out and pay through the registration form. Both steps must be completed in order for you to be fully registered. Below are our registration deadlines:
- Early Bird Registration: $30, Ends October 5, 2024
- Regular Registration: $35, Ends November 2, 2024
- Late Registration: $40, Ends November 9, 2024
TRAVEL SUBSIDY:
We are providing the first 30 chapters a $100 subsidy towards their travel and other conference expenses. To receive financial aid to attend the Hepatitis Conference, please fill out the travel subsidy application.
HOUSING INFORMATION:

Alex Le
Health Affairs Vice President
Texas A&M College of Medicine

Christopher Huy Doan
Hepatitis Director
John Sealy School of Medicine at UTMB Galveston

Alicia Bui
Hepatitis Director
Oakland University William Beaumont School of Medicine

Bunnarin Theng
Hepatitis Director
John Sealy School of Medicine at UTMB Galveston

Hoang-Viet Tran
Hepatitis Graphics Committee
George Washington School of Medicine

Nick Sze
Hepatitis Graphics Committee
Wright State University Boonshoft School of Medicine

David Wang
Hepatitis Graphics Committee
John Sealy School of Medicine at UTMB Galveston

Sophia Choi
Hepatitis Speakers Committee
John Sealy School of Medicine at UTMB Galveston

Madeline Pan
Hepatitis Logistics Committee
John Sealy School of Medicine at UTMB Galveston

Roland Yu
Hepatitis Speakers Committee
John Sealy School of Medicine at UTMB Galveston

Luke Sequeira
Hepatitis Speakers Committee
Brown University

Leah Katz
Hepatitis Logistics Committee
Touro College of Osteopathic Medicine – Middletown

Louis Zhang
Hepatitis Logistics Committee
UT Health San Antonio Long School of Medicine
- Home
- Archive by Category "Conference"
Contact Us
Questions? Email us at hepatitis@apamsa.org.
.
2024 Region IV & IX Conference

Crossing Silk Roads: Exploring Intersections and Connections of AAPI Identity and Healthcare
Date: Saturday, October 12th, 2024
Location: Emory University School of Medicine, Atlanta, GA
Registration Details: Click below for more info
We are thrilled to announce a collaboration between APAMSA Regions IV and IX for this year’s regional conference, themed “Crossing Silk Roads: Exploring Intersections and Connections of AAPI Identity and Healthcare.” This in-person event will be hosted at Emory University School of Medicine and is open to both APAMSA members and non-members. Attendees can look forward to an exciting day filled with AAPI speakers, engaging panels, interactive workshops, valuable networking opportunities, a poster session, and more!
Conference Information:
Theme: “Crossing Silk Roads: Exploring Intersections and Connections of AAPI Identity and Healthcare”
Date & Time: Saturday, October 12, 2024 | Time 8:30 AM – 4:30 PM
Location: Emory University School of Medicine | Atlanta, GA (2015 Uppergate Dr, Atlanta, GA 30307)
Schedule
Pre-Registration: 7:45 AM – 8:30 AM
Welcome: 8:30 AM – 8:45 AM
Opening Statements and Introduction: 8:45 AM – 9:00 AM
Keynote Speaker: 9:00 AM – 10:00 AM
Be The Match: 10:00 AM – 10:20 AM
Breakout Session 1: 10:30 AM – 12:00 PM
Lunch: 12:00 PM – 1:00 PM
Poster Session: 1:00 PM – 1:50 PM
Breakout Session 2: 2:00 PM – 2:50 PM
Breakout Session 3: 3:00 PM – 3:50 PM
Closing Statements: 4:00 PM – 4:30 PM
Stay tuned as we reveal more speakers!

Dr. Sandra Wong, MD, MS
Sandra L. Wong, MD, MS, an accomplished surgical oncologist and health services researcher who joined Emory School of Medicine as Dean in March 2024. She also serves as the chief academic officer for Emory Healthcare.
Dr. Wong is a surgical oncologist specializing in the management of soft tissue sarcomas, melanoma and non- melanoma skin cancers. She is among the most widely recognized health services researchers in academic surgery, with an extensive record of research funding and more than 250 peer-reviewed studies to her credit. She has held leadership positions in several prominent professional organizations including the Society of Surgical Oncology, the Society of University Surgeons, and the Society of Surgical Chairs. Wong has been honored with numerous medical student and resident teaching awards.
She completed her bachelor’s degree at the University of California Berkeley. After receiving an MD from Northwestern University Medical School, she completed a surgical residency at the University of Louisville School of Medicine and a surgical oncology fellowship at Memorial Sloan-Kettering Cancer Center.
Wong spent a decade at the University of Michigan where she was an instrumental leader as a vice chair of academic affairs and an associate chief of staff. As chair of the Department of Surgery at the Dartmouth Hitchcock Medical Center and the Geisel School of Medicine at Dartmouth, she was responsible for overseeing all aspects of research, education and clinical operations. During her tenure at Dartmouth, she co-founded the federally-funded Center for Rural Health Care Delivery Science, which provides infrastructure to train junior investigators who focus on solving challenges associated with the provision of equitable health care.

Dr. Amy Chen, MD, MPH, MBA, FACS
Amy Y. Chen, MD, MPH, MBA, FACS is the Willard and Lillian Hackerman Professor and the Inaugural Vice Chair for Diversity, Equity and Inclusion of the Department of Otolaryngology and Head and Neck Surgery at The Emory University School of Medicine. She serves as the Director of Head and Neck Endocrine Surgery and was the Program Director for the Head and Neck Surgery Fellowship. Her expertise is in thyroid and parathyroid surgery. She has also served as Director of Health Services Research in the Department of Surveillance and Health Policy Research of the American Cancer Society. She serves on the Board of the American Thyroid Association, Asian Pacific Institute on Gender Based Violence, and the Partnership for Southern Equity.
Dr. Chen has been instrumental in developing a team approach to patient care. She developed and currently leads the multidisciplinary thyroid and head and neck tumor conferences. Her primary focus of research is in measuring outcomes of oncology treatment as well as measuring determinants of successful outcomes of care. Dr. Chen’s research agenda is to create a multi-disciplinary, multi-site center dedicated to health services research, outcomes, and quality of care. Her secondary focus of research is directed toward translational research of head and neck and thyroid malignancies. She is also an implicit bias facilitator and a diversity, equity and inclusion champion.
Dr. Chen joined the Emory faculty in 2001 after a fellowship in Head and Neck Oncologic Surgery at the MD Anderson Cancer Center in Houston. Prior to that fellowship she was a resident in Otolaryngology and General Surgery at Baylor College of Medicine, also in Houston.
She is board certified by the American Board of Otolaryngology and holds a Master of Public Health degree from the University of Texas School of Public Health. She also recently completed her Master of Business Administration at Goizueta Business School at Emory. Dr. Chen has received numerous awards and honors, among them the Helen F. Krause, MD Trailblazer Award, Emory Eminent Physician Award, the Margaret Butler Award for Outstanding Mentor of Women Head and Neck Surgeons, Emory School of Medicine Excellence in Diversity, Equity and Inclusion Award, Top Atlanta Doctor, Gussack Memorial Award for Teaching, Percy Memorial Research Award, the Rande Lazar Health Services Research Award, the American Head and Neck Society Scholarship Award, and The Women’s Fund for Health, Education and Research Grant. She is married and birthed two daughters. She misses her recently deceased rescue yellow Labrador retriever.
In January 2025, she will be moving to City of Hope Cancer Center in Newnan, GA as Chief of Surgery and Director of Thyroid Oncology.

John William Eley, MD, MPH
Bill Eley is a native of Georgia who received his Bachelor of Arts in chemistry, Doctor of Medicine, and Master of Public Health from Emory University. He holds faculty appointments of Professor in the Department of Hematology and Medical Oncology and Associate Professor in the Department of Epidemiology at the Rollins School of Public Health. A Board-certified medical oncologist, he has practiced oncology within Emory Healthcare and at Grady Memorial Hospital.
Dr. Eley was initially appointed in the Rollins School of Public Health (RSPH) where he investigated disparities in cancer survival. He has taught medical students clinical epidemiology and served on the Admissions committee at the Emory University School of Medicine (SOM). In 2000 he became Associate Dean and Director of Admissions in School of Medicine and in 2004, he was appointed Executive Associate Dean for Medical Education and Student Affairs. In his current role he oversees the six degree programs within the School of Medicine and the Graduate Medical Education programs and is overseeing the Medical Education Curriculum Transformation Initiative.
Dr. Eley is committed to the spread of compassion – compassion for others and self, as embodied by the Cognitive Based Compassion Training (CBCT) course developed at Emory. He is privileged to teach CBCT within the School of Medicine and is interesting in incorporating compassion training in the field of medicine.

Dr. Reena Hemrajani, MD
Dr. Reena Hemrajani completed medical school at Florida State University and internal medicine residency, followed by chief residency at Virginia Commonwealth University (VCU). She subsequently served as an academic hospitalist and in residency education leadership at George Washington University and VCU. In 2017, Dr. Hemrajani moved to Atlanta to be an academic hospitalist in the inaugural Hospital Medicine Program at Grady Memorial Hospital. At Emory, she has held roles as the Associate Division Director for Faculty Development in Hospital Medicine and Associate Program Director for the residency. In 2022, she stepped into the role of the Internal Medicine Residency Program Director at Emory and values her role in supporting residents to achieve their goals. In her free time, she is an avid city walker in the vibrant neighborhoods of Atlanta, enjoys trying out new local restaurants, and takes advantage of opportunities for travel.

Dr. Emily Herndon, MD
Emily Herndon is an Assistant Professor in the Department of Family & Preventive Medicine at Emory and currently serves as a Staff Physician at Emory Student Health. She, along with a registered dietician and chef, teaches a second-year elective on Culinary Medicine. She is a graduate of Emory School of Medicine, a past Small Group Advisor and Clerkship Director, and practicing community physician for over 20 years. Much of her clinical experience was working at a Grady Neighborhood Center that served many immigrants and people from a wide variety of cultures. She enjoys traveling, cooking, dancing and yoga.
Contact Information: eherndo@emory.edu

Dr. Wei Huang, MD, PhD
Dr. Wei Huang is an Associate Professor of Rehabilitation Medicine at Emory University School of Medicine. She received her medical degree in Shanghai, PhD in Neuroscience/Psychology at Vanderbilt University, and residency training at UNC Chapel Hill. Besides being a Board-certified physiatrist, Dr. Huang is also certified in Integrative Holistic Medicine and is a certified acupuncturist in Georgia. She is the founding physician of the first acupuncture clinic and the first integrative medicine clinic at the Atlanta VA Medical Center, and often acts as a consultant to regional medical centers about acupuncture services. She is currently co-Medical Director of Emory Acupuncture Service. Dr. Huang serves on the Editorial Board of the American Journal of PMR. Her own research and publications have been in sleep, pain, traumatic brain injury, and geriatric medicine; but her long-standing passion is to integrate the best of world’s traditional medicines with Western Medicine in clinical practice.

Dr. Jeane Khoo, DO

Dr. Abhi Kole, MD, PhD
Dr. Abhi Kole received his MD from Emory and PhD in Immunology from the University of Oxford. He is a graduate of the Internal Medicine residency program at Emory and was subsequently a fellow with the HEAL Initiative (Health Equity, Action, and Leadership) through UCSF and spent two years in India with this program. He returned to Grady as a hospitalist in 2020. He also teaches the Community Learning and Social Medicine course for first-year medical students. His areas of interest are in addressing structural causes of inequity in our healthcare system.
Contact Information: akole@emory.edu

Dr. Gerald Lee, MD
Dr. Gerald Lee, MD is an associate professor of pediatrics and medicine at Emory University School of Medicine. He is an allergist/immunologist at Children’s Healthcare of Atlanta and Grady Memorial Hospital. He completed his Internal Medicine/Pediatrics residency at Saint Vincent’s Hospital in New York City and an Allergy/Immunology fellowship at Cincinnati Children’s Hospital Medical Center. He is the director of the Emory allergy/immunology fellowship and the preclinical immunology thread for the medical school. His academic interests are medical education, quality improvement in allergy/immunology, and hosting the AllergyTalk podcast.

Dr. Rebecca Sanders, MD, PhD
Dr. Sanders has served as Emory Pediatrics Residency Program Director since 2021. She works as a hospitalist for Children’s Healthcare of Atlanta at both the Hughes Spalding and Arthur M Blank campuses. She has a strong interest in curriculum development, particularly in improving mental health care education for pediatric residents and fellows. In her spare time she loves reading, gardening, and building Lego.

Dr. Jessica Wu, MD
Dr. Wu was born in Los Angeles, CA but moved to Houston, Texas at a young age. She then spent the next twenty-years in the Lone Star state, where she acquired her love for country music, football, and BBQ (mostly the sides!). She attended The University of Texas-Austin (Hook ‘em!) and received a Bachelor of Arts degree in Biochemistry with a minor in Business Administration. After doing a year of research at MD Anderson, Jessica attended The University of Texas Medical Branch – Galveston for medical school.
At this time, Jessica decided it was time to explore places outside of Texas. She left the great state of Texas and moved back to Los Angeles for her General Surgery training at USC. During her residency at USC, Jessica developed an interest in hernia surgery and bariatric surgery. Her research focused on optimizing hernia surgery and bariatric surgery outcomes at a safety-net hospital. Given such interest, Jessica is currently pursuing a MIS fellowship at Emory University with hopes of becoming a future hernia, foregut, and bariatric surgeon.

Dr. Ju Zhang, PhD
Ju Zhang is a postdoctoral fellow in bioethics at the Emory University Center for Ethics. She received her Ph.D. in philosophy from The University of Texas at Austin in 2022. Her current research focuses on developing and defending a trust-oriented model of the patient-physician relationship. Her goal is to promote reasonable patient-physician trust by modifying relevant concepts such as patient autonomy, informed consent, and justified intervention in light of her model. She intends to extend her research on patient-physician trust to nonexpert-expert trust in general and to trust between a relatively disadvantaged individual/group and a relatively advantaged individual/group. She is also interested in studying trust and cooperation among communities, societies, and nations, believing that reasonable trust is key in tackling global issues such as climate change and pandemics.
Email: ju.zhang@emory.edu

Christopher Doan
Christopher Doan is a an MS4 from UTMB Galveston and has recently been recognized as a member of the GHHS and AOA. He grew up in the Dallas metroplex and attended UT Dallas for his undergraduate degree. He is currently one of the National APAMSA Hepatitis Initiative Directors and has research interests in AANHPI disaggregation of cancer data, cancer screenings, and medical humanities. Previously, he also served as a local chapter president and was one of the founding members of the Hepatitis B screening initiative with outreach to Asian immigrant fishermen working in the Galveston port.
Need help finding accommodations? Check out our Accommodations Guide!


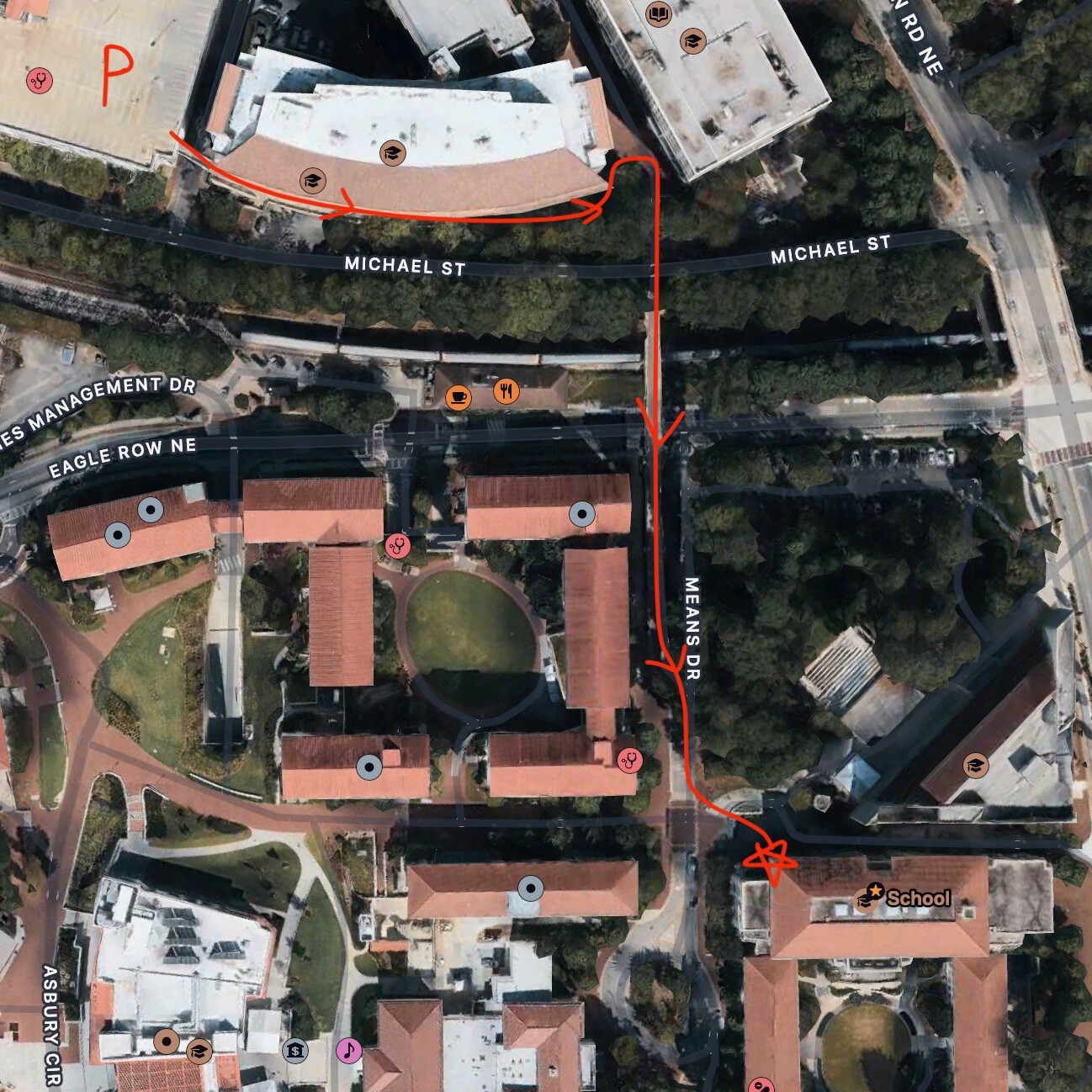
Michael St. Entrance
Walk to Entrance
APAMSA Regions 4 and 9 invite you to submit an abstract for the Regional Conference on October 12, 2024. There is no cost for submitting an abstract.
Deadline for abstract submission: September 28, 2024
Submissions are now closed. Thank you all who submitted their abstracts. If you have not bought your ticket, please do so as soon as possible.
Accepted Posters
“Novel compound heterozygous mutations in ILNEB syndrome”
- Hannah Wu
“Kidney Utilization in the Context of a Shifting Donor Landscape”
- Helen Jeon
“Our Approach to Vitrectomy Surgery in Diabetic Retinopathy is Changing Due to Intraoperative Fluorescein Angiography Guidance”
- Mariam Omar
“Comparing Outcomes for Proximal Tibia Replacement in High Grade Primary Bone Sarcoma, Low Grade Primary Bone Sarcoma and Metastatic Bone Disease”
- Linhan Ha
“Revolutionizing Mandibular Osteoblastoma Treatment: The Power of Computer-Assisted Virtual Surgical Planning”
- Leon Liu
“Mechanisms of Action of Kavalactone on Nociceptive Pathways: A Systematic Review”
- Daiana Takashima
“Clearance of Purinergic Molecules with Hemodialysis”
- Zijian Tan
“Prevalence of Comorbid Conditions in Young Men Presenting with Erectile Dysfunction”
- Troy La
“Characteristics of Men Switching Testosterone Formulations – Who, What, and Why”
- Troy La
“Utilization of Long-Term Video EEG Monitoring in Pediatric Patients: Experience of a Large Pediatric Tertiary Care Center”
- Phillip Sumardi
“Use of Ambulatory Blood Pressure Monitoring (ABPM) to Predict Left Ventricular Mass Index (LVMi) in the Pediatric Population: A Single-Center Experience.”
- Isha Patel
“Understanding Cultural Barriers and Mental Health Disparities in Treatment-Seeking Behaviors Among Asian Americans”
- Carrie Chen
“Skin Cancer Screening and Perceptions Quality Improvement”
- Danielle Flores
“Enhancing Alzheimer’s Dementia knowledge and utilization through trainings for healthcare professionals”
- Winnie Chen
“Hidden Epidemic of India’s Most Marginalized: Sickle Cell Amongst Scheduled Castes and Scheduled Tribes”
- Supriya Jain, Esha Mohnalkar
“Sex Ed for Med”
- Harrison Goodall
“Improving Health Literacy and Diabetes Management Adherence with Updated Novel Educational Technology”
- Michael Xie
“Transfer of low-risk patients in emergency general surgery: Patient survey on the process of care and perceptions of safety”
- Min Hyuk Jang
“Metabolic Biomarkers of Recurrent Urinary Tract Infections Among Post-Menopausal Women”
- Ivy Nguyen
National Board

Amelia Huynh
Membership Co-VP
Pacific Northwest University
of Health Sciences

Paul Tominez
Membership Co-VP
University of California, San Francisco School of Medicine

James Chen
Region IX RD
University of Texas Medical Branch – John Sealy School of Medicine

Daiana Takashima
Region IV RD
Emory University School of Medicine

Jerry Liu
Region IX RD
Texas A&M School of Medicine

Yuna Seo
Region IV RD
Philadelphia College of Osteopathic Medicine (North Georgia)

Francis Khuong
Region IX RD
Texas Tech University Health Sciences Center

Neil Vuppala
Region IV RD
Alabama College of Osteopathic Medicine
Local Chapter Leadership

Brandon Lee
Emory University School of Medicine

Janet Mao
Emory University School of Medicine

Katherine Tong
Emory University School of Medicine

John Choi
Emory University School of Medicine

Hithardhi Duggireddy
Emory University School of Medicine

Max Su
Emory University School of Medicine

Margaret Lim
Emory University School of Medicine

Akshay Nair
Emory University School of Medicine
Contact Us
Questions? Email us at region4@apamsa.org or region9@apamsa.org
2024 Region VIII Conference
Welcome to the Region VIII Conference!
Turning the Tide
Date: Saturday, October 19, 2024
Time: 10:00 AM – 4:30 PM l Registration starts at 9:15 AM
Location: University of California, Irvine l Nelson Auditorium, 1003 Health Sciences Rd, Irvine, CA 92617
Tickets: $8 Early Bird price until 9/28/24 l $10 for General Admission
Lunch and swag are included in all tickets!

APAMSA Region VIII and the UCI APAMSA chapter are ecstatic to invite you to the annual Region VIII Conference hosted at the University of California, Irvine in Irvine. We are excited to host this event, celebrate all backgrounds, and uplift AANHPI communities through our conference “Turning the Tide.”
Our theme highlights the shift in narrative towards unity, commemorating diverse backgrounds and perspectives, and acceptance of all. Through this conference, we hope to uphold this goal by hosting influential speakers in the AANHPI sphere, facilitating pre-medical and resident/attending panels, and featuring the research contributions of APAMSA members.
Please join us for a lovely day of celebration, as well as networking with fellow medical and pre-medical students from neighboring chapters! We are excited to welcome you to Irvine!
Saturday, October 19th, 2024
9:15 AM – 10:00 AM l Registration
10:00 AM – 10:40 AM l Keynote Speaker l Dr. Donna Tran
10:45 AM – 11:25 AM l Lung Cancer in Asian American Women: A Rising Disparity l Dr. Jeffrey Velotta
11:30 AM – 12:10 PM l Women in Medicine l Dr. Alison Taur, Dr. Susan Wu, Dr. Sunny Park, Dr. Shravani Reddy
12:10 PM – 12:50 PM l Lunch, LGBTIA+ Mixer, & Exhibitors for NMDP, All of Us, Vot-ER
12:50 PM – 1:30 PM l Poster Session l Plumwood Room 166
1:35 PM – 2:00 PM l National Marrow Donor Program (NMDP)
2:05 PM – 2:30PM l All of Us
2:35 PM – 3:15 PM l HEAL-IM Program and Holistic Medicine l Dr. Hwang
3:20 PM – 4:00 PM l Breakout Session
- Residency Panel (Nelson Auditorium): Dr. Donna Tran, Dr. Shiree Lee, Dr. Charissa Lau, Dr. Michael Sy, Dr. Catherine Wu, Dr. Kevin Naito
- Pre-Medicine Panel (Tamkin Room F110): UCISOM Dean of Students Dr. Megan Osborn, UCI Med Students
- Ultrasound/Hepatitis Workshop (MedEd 2nd floor Clinical Skills Center)
4:00 PM – 4:30 PM l Closing

Jacob Hwang, ND
Jacob Hwang is a naturopathic doctor and integrative health specialist who uses a whole-person approach to patient care with emphasis on emerging evidence and health promotion. He earned his doctoral degree in naturopathic medicine from Bastyr University in Kenmore, Washington and completed a three-year naturopathic residency program at Bastyr University Clinic and UCI Susan Samueli Integrative Health Institute. Besides seeing patients and training learners, Dr. Hwang also contributes to various educational initiatives.
Dr. Hwang uses an integrative approach to treating diseases, which encompasses a comprehensive diagnostic process, evaluation of social determinants of health, and unique consideration for the individual patient presentation. His clinical toolbox typically involves lifestyle interventions, dietary recommendations, evidence-based nutraceutical supplements, and limited pharmacological therapies. In addition, Dr. Hwang believes having a collegial healthcare team is important to maintain patient-centered care and allow shared insights to make the best clinical decision. He enjoys coordinating and working alongside other medical specialists and healthcare providers.

Megan Osborn, MD
Dr. Osborn is Vice Chair for Education and Associate Professor of Clinical Emergency Medicine at the University of California, Irvine (UCI). She also serves as the Associate Dean for Students for UCI School of Medicine. Dr. Osborn is passionate about medical education, ophthalmologic, ENT, and hematologic emergencies.
She has more than 60 peer-reviewed publications and has won the Clinical Pathologic Case (CPC) Competition twice and the ACEP National Faculty Teaching Award. Dr. Osborn serves as the Senior Associate Editor for the innovative Journal of Education and Teaching in Emergency Medicine (JETem).

Sunny Park, MD
Dr. Sunny Park is double board-certified in Facial Plastic & Reconstructive Surgery, and Otolaryngology, Head & Neck Surgery. She specializes in cosmetic and reconstructive surgeries of the face and neck, and has a private practice in Newport Beach. After attending UC Berkeley for her BA and MPH, she obtained her MD from Jefferson Medical College. She completed her residency in Otolaryngology, Head & Neck Surgery at Penn State University followed by a fellowship in Facial Plastic & Reconstructive Surgery at LSU Shreveport. She has lectured regularly at the American Academy of Facial Plastic and Reconstructive Surgery meetings and has volunteered for medical mission trips overseas, most recently in 2019 to Vietnam. In addition, Dr. Park has been chosen as a Physician of Excellence in Facial Plastic & Reconstructive Surgery by Orange County Medical Association and Orange Coast Magazine every year since 2021.

Shravani Reddy, MD
Dr. Shravani R. Reddy is a UCI Health gastroenterologist who specializes in esophageal disorders. Her clinical interests include gastroesophageal reflux disease (GERD), achalasia, Barrett’s esophagus and esophageal cancer.
She earned her medical degree at American University of the Caribbean. She completed a residency in internal medicine followed by a fellowship in gastroenterology, both at Virginia Tech Carilion School of Medicine in Roanoke.
She has a particular interest in esophageal disorders and has completed additional training through the American Neurogastroenterology Motility Society. She has a passion for medical education and has taken an active role in various teaching capacities, including curriculum development and procedure-based instruction.

Alison Taur, MD
Dr. Alison Taur (she/her) serves as Regional Coordinating Chair of Nuclear Medicine for Kaiser Permanente Southern California and as Clinical Assistant Professor for the Kaiser Permanente Bernard J. Tyson School of Medicine. She graduated from University of Michigan Medical School and completed her Nuclear Medicine residency at Stanford University School of Medicine. In addition to her clinical and administrative duties, Dr. Taur devotes her time to training, education, and advocacy for equitable transgender health care both within and outside of KP. She helped found the multidisciplinary Pediatric GenderCare Clinic at KP San Bernardino County. Dr. Taur also helps facilitate a trans teen support group and is active in her local PFLAG chapter. She lives with her wife of now 27 years and three sons in Newport Beach and enjoys playing double bass and feasting on exquisite sushi.

Donna Tran, MD, MPH
Donna Tran, MD, MPH, is a psychiatry resident at Stanford Health Care and earned her MD at Michigan State University College of Human Medicine and MPH at Johns Hopkins School of Public Health. During medical school, she served as the National President of the Asian Pacific American Medical Student Association from 2021 – 2023. In 2024, she was appointed as the District 10 Representative on the Senior Citizens Commission of the City of San Jose and interned under U.S. Congressman Jimmy Panetta (CA-19). Previously, she worked on health policy in the U.S. Senate Committee on Health, Education, Labor, and Pensions (HELP) and presented to the President Biden’s Advisory Commission for Asian American, Native Hawaiian, and Pacific Islander AANHPI (PAC-AANHPI/WHIAANHPI), advocating for public mental health. For research, she focuses on health inequities, leadership, primary care, and advocacy. In her free time, Donna enjoys bouldering, her French bulldog, Boba Princess, and TED Talks/podcasts.

Jeffrey Velotta, MD, FACS
Dr. Jeffrey Velotta, MD, FACS is a thoracic surgeon at Kaiser Permanente Oakland Medical Center, an adjunct Clinical Assistant Professor in the Department of Surgery at the University of California, San Francisco (UCSF) School of Medicine, and Clinical Professor in the Department of Clinical Science at the Kaiser Permanente Bernard J. Tyson School of Medicine. Dr. Velotta’s clinical and research interests involve innovative techniques and regionalization pathways for lung cancer, esophageal cancer, and mesothelioma. In addition, his most recent research involves improving lung cancer screening uptake in Asian Americans and identifying key factors in the rising incidence of lung cancer in non-smoking Asian American women.
Conference Address
Nelson Auditorium
1003 Health Sciences Rd, Irvine, CA 92617
Airport: John Wayne Airport (Santa Ana)
Valid Parking Location: General unmarked and AR reserved stalls Lot 83, Lot 83D, or Health Sciences Parking Structure,
Parking Valid Time: All Day
Sales Window: 10/09/2024 – 10/19/2024
Permit Rate: $16 /registration
Direct Link: https://apps.parking.uci.edu/parkbyplate/s/purchase.cfm?code=ODYBMKWW
There will be pedestrian signs put up to help direct you, but please feel free to contact us if you run into any difficulties finding where to go.
Housing: Below are some recommendations that are close by UCI!
We are welcoming posters from all research fields. ABSTRACT SUBMISSIONS ARE CLOSED.

Julia Liu
Region VIII Director
Oregon Health & Sciences University (OHSU)

Christine Nguyen
Region VIII Director
Pacific Northwest University of Health Sciences (PNWU)
Brandon Tang
Region VIII Director
University of Southern California (USC)

Naomi Tsai
Region VII Director
Oregon Health & Science University (OHSU)

Amelia Huynh
Membership Vice President
Pacific Northwest University of Health Sciences (PNWU)

Jiyeon Lee
Mentorship Chair
University of California Irvine (UCI)

Justin Chiu
Research/Grant Chair
University of California Irvine (UCI)

Ryan Hoang
Co-President
University of California Irvine (UCI)

Frank Lee
Health Education Chair
University of California Irvine (UCI)

Catherine Zhang
Co-President
University of California Irvine (UCI)
Contact Us
Questions? Email us at region8@apamsa.org.
2024 Region III Conference

Peril, Power, Progress: Navigating AANHPI Identity and Advocacy in the Public Space
Date: Saturday, October 5th, 2024, 9 AM-4 PM
Location: Drexel University College of Medicine (60 N 36th St, Philadelphia, PA 19104)
Registration Details: Click below for more info
APAMSA Region III and the APAMSA chapter at Drexel University College of Medicine are so excited to welcome you to this year’s Region III Conference! Our theme this year is “Peril, Power, Progress: Navigating AANHPI Identity and Advocacy in the Public Space.”
Location: Drexel University College of Medicine (60 N 36th St, Philadelphia, PA 19104)
Date: Saturday, October 5th, 2024
Time: 9 AM – 4 PM, with an optional post-conference social afterwards
At our conference, we want to explore the intersection between medicine, political involvement and AANHPI identity, a theme that seems particularly timely during this election year. What does activism look like on the ground, working with local community stakeholders? How can we emphasize health equity and strive towards eliminating disparities in our future practices as health professionals?
We hope this conference can be a space where we can form lasting connections with one another and be empowered to be a voice for change in our communities. Registration will include attendance to talks from a variety of wonderful speakers, networking opportunities, a space to present your research, workshops, lunch, and more!
Ticket Pricing:
Early bird tickets are $20 (until 9/28).
Regular pricing after 9/28 is $25
Saturday, October 5
| Time | Event | Location |
| 8:00 – 9:00 AM |
Pre-Registration |
1st Floor Lobby |
| 9:00-9:30 AM |
Opening Statements |
1W03-05 |
| 9:30-10:15 AM |
Keynote AddressSpeaker: Walter Tsou “Reflections on Health Equity: An Unending Journey” |
1W03-05 |
| 10:15-10:30 |
Break |
|
| 10:30 – 11:30 AM |
Breakout: Professional Development |
|
|
|
Session 1: Specialty Networking Session (Fireside Chat)For the list of physicians attending and their bios, please see our speaker tab |
4E05 |
Session 2: Pre-Health Panel (Q&A)For the list of students attending and their bios, please see our speaker tab |
4E06 | |
| 11:30 AM- 12:40 PM |
Lunch & Research Poster Session |
4E04 |
| 12:40-2:45 PM |
Breakout Sessions: Skills and Community Health |
|
| 12:40-2:00 PM |
Skills Sessions |
|
Session 1: Intubation WorkshopLed by: Steven Pham DO, Sophia Chiu MS, MD |
7E19 | |
Session 2: Suture WorkshopLed by: Jason Han MD, Justin Ly MD, Sophia Dang MD, Yazid K Ghanem, MD |
4E06 | |
Session 3: Lumbar Puncture WorkshopLed by: Linda Xu, MD |
7E17 | |
Session 4: Advocacy by AMA |
4E05 | |
| All sessions will run twice with every attendee getting the chance to attend one clinical workshop + advocacy; you will be given the opportunity rank your preference at registration and assigned a group accordingly | ||
| 2:00-2:45 PM |
Community Health Sessions |
|
Session 1: Mango Tree CounselingSpeaker: Hanna Lee, ATR, MA, MA, BFA |
1W03-05 | |
Session 2: No Arena in ChinatownSpeakers: No Arena JeffMed: Sharon Chen, DNP, FNP-BC, Dr. Bill King, “Jimmy” Cheemeng Low, NREMT |
4E06 | |
Session 3: Kevin Rituzel, Koreatown LA Community Health ClinicSpeaker: Kevin Riutzel, MS, DO
|
4E05 | |
| 3:00-3:30 PM |
Hep B UnitedSpeaker: Catherine Freeland, PhD, MPH |
1W03-05 |
| 3:30 PM | Conference End and Closing Statements | 1W03-05 |
Stay tuned as we reveal more speakers!

Walter Tsou, MD, MPH
Keynote Speaker
Walter Tsou, MD, MPH is a nationally known consultant on public health and health care reform. He is a retired Adjunct Professor of Family Medicine and Community Health at the University of Pennsylvania where he taught community health at their Center for Public Health Initiatives. He is a Past President of the American Public Health Association and former Health Commissioner of Philadelphia. He was the founding Deputy Director for Personal Health Services and Medical Director of the Montgomery County (PA) Health Department from 1991-2000. He has extensive experience in public health and has lectured widely on public health and health disparities.
Nationally, he is a Board Advisor at Physicians for a National Health Program and Healthcare-NOW. He is Past Chair of the Board of the Asian Pacific Islander American Health Forum. Locally he is on the boards of Physicians for Social Responsibility Pennsylvania, Hepatitis B Foundation, Health Care for All Pennsylvania and the Philadelphia County Medical Society. His medical degree is from the University of Pennsylvania; his MPH is from the Johns Hopkins School of Hygiene and Public Health, and he has an honorary Doctorate in Medical Sciences from Drexel University.

Kevin Riutzel MS, DO
Community Health Speaker
Born in South Korea and raised in the greater LA area, Kevin Riutzel is a family physician currently working in Los Angeles, CA. The clinic he works at is a federally-qualified health center in LA’s Koreatown primarily serving local Korean-American and local AAPI communities, many of whom are the 1st generation in their families to immigrate to the U.S.
He has served in several roles for the Asian Pacific American Medical Student Association including National President for three terms. He finished his undergraduate studies at UC San Diego and graduate studies at Columbia University. After graduating from Touro University Nevada, he completed his training in family medicine at UC Irvine with a focus on integrative medicine. He served as one of the chief residents while at UC Irvine.
Kevin takes a particular interest in mental health in AAPI communities along with providing an integrative and holistic approach to the care he offers to the communities he serves while focusing on a work-life balance to stay energized for the patients he serves.

Hanna Lee (she/her), ATR, MA, MA, BFA
Community Health Speaker: Mango Tree Counseling and Consulting
Hanna Lee (she/her) is a disabled and neurodivergent Korean-American art therapist and art educator with an extensive background in working with people of all ages and abilities. She is a passionate proponent of using the arts to provide a variety of supports for historically marginalized populations and has spoken on this topic through organizations such as the National Art Educators Association, Department of VSA at the John F. Kennedy Center for the Performing Arts, and the International Conference on Disability Studies, Arts, and Education. Working with and advocating for diverse communities has allowed her to explore art-making as an unlimited means of honest expression and personal growth beyond the social, economic, physical, and intellectual limits to which people are often confined.
Lee’s educational background includes a Masters in Art Therapy and Counseling from Drexel University and a Masters in Art Education with an emphasis on Inclusive Practices from Moore College of Art & Design. She currently works with Asian Americans as a therapist at Mango Tree Counseling & Consulting and serves as Director of Research at the Asian Americans with Disabilities Initiative to provide investigative research, advocacy, and resources for Asian Americans with disabilities. Lee is also an adjunct professor at her alma mater, Moore, where she is currently establishing an art therapy minor.

Sharon Chen, DNP, FNP-BC
Community Health Speaker: No Arena Jeff Med
Sharon is a Family Nurse Practitioner who provides primary care in Mandarin and English at a federally qualified health center (FQHC) in Philadelphia Chinatown. She studied Environmental Biology at the University of California, Berkeley, and completed her nursing education at Columbia University. As a former Care Coordination Nurse and School Nurse in several outpatient settings, she has a special interest in understanding how social, cultural, and environmental factors affect health status. In her spare time, she runs the @ClimateHealthNurse blog and Instagram page, where she writes about sustainability and wellbeing.

“Jimmy” Cheemeng Low, NREMT
ACLS, PALS, BLS, Certified in Ultrasound Guided IV, Burn Wound Care specialist
United State Air National Guard 4N (LPN), BLS Instruction, Tactical Combat Casualty Care (TCCC) Instructor, Certified CPR Instructor
Community Health Speaker: No Arena Jeff Med
Jimmy was born and raised outside Kuala Lumpur, Malaysia. He came to the US in 1995 to pursue his education and after exploring several paths became an EMT. In 2005 he joined the National Guard where he went on to oversee medical logistics for the 111th Medical Group. He has been working as an EMT or Technician inside the hospital since 2007. He holds many specialty medical certificates and has wide ranging experience working in the emergency room, trauma department, surgical ICU, and remote medicine. Jimmy achieved Master Sergeant rank and teaches several courses through the Air Guard as a 4N, which is the civilian equivalent of an LPN.

Anudeeta Gautam
Community Health Speaker: Advocacy by AMA
Her AMA journey began as President of the LKSOM AMA Chapter during her first year, and she now serves as the AMA-MSS Region 6 Chair and a Delegate in both the MSS and Pennsylvania caucuses to the AMA House of Delegates. Organized advocacy has been the most transformative part of her medical school experience, showing her the power of persistent, diverse voices, even when outnumbered. She is passionate about helping others find their voice and forge their unique path. Outside of work, you can find her at a dance workshop learning a new style, exploring the Philly neighborhoods with her camera, or booking her next flight.

Catherine Freeland, PhD, MPH
Hep B United
Catherine Freeland is the Associate Director of Public Health Research at the Hepatitis B Foundation. Catherine received her Ph.D. at Thomas Jefferson University, College of Population Health with a concentration in Health Behavior Science and a dissertation on addressing low hepatitis B birth dose uptake in Nigeria. She led the effort to incorporate values and preferences for people with lived experience within the updated 2024 World Health Organization Guidelines and continues to focus on addressing barriers and facilitators to hepatitis B elimination globally.
Resident/Fellow Panel

Pratistha Koirala, MD, PhD
Obstetrics & Gynecology/Gynecologic Oncology, Temple University
Pratistha Koirala, MD, PhD, was elected to the American Medical Association Board of Trustees in June 2021. Dr. Koirala is a gynecologic oncology fellow at Fox Chase Cancer Center and Temple University in Philadelphia.
Dr. Koirala’s health care journey began thousands of miles away, in Nepal, in the foothills of the tallest mountains in the world. In pursuit of education her family immigrated to the United States when she was a child. Her family story, of poverty and a lack of access to health care, inspired her to become a physician. Years later, as a medical student in the Bronx, she cared for patients living in the poorest congressional district in the United States. After witnessing the impact of social determinants of health on both a population and at an individual patient level, she became active in health policy, aiming to better the health and well-being of her community.
When she joined the AMA as a medical student, one of her first endeavors was celebrating and promoting the organization’s accomplishments as a membership recruitment chair. Since then, Dr. Koirala has served in multiple leadership roles in organized medicine; notably, she was a member of the Executive Council of the Medical Society of the State of New York and served on the board of directors of the AMA Political Action Committee.
Dr. Koirala attended college at the University of Connecticut and graduated with a major in biology. She completed her MD, her MS in genetics, and her PhD in molecular pharmacology at Albert Einstein College of Medicine. Her research has ranged from understanding the role of immune checkpoint inhibitors in sarcoma to the genetic basis of cardiac development. She completed residency in obstetrics and gynecology at Danbury Hospital and a health equity fellowship at Boston Medical Center. As a physician scientist, Dr. Koirala understands the power the AMA has as a trusted voice in medicine and public health.
Dr. Koirala’s work and accomplishments within the AMA reflect the value she places in diversity in medicine and health equity. Her actions and advocacy are driven by her personal story as an immigrant, as someone who has lived in poverty, as a woman, as a scientist, and as a trainee working with underserved populations.

Minh Than, MD, PhD
Internal Medicine, Hematology-Oncology, University of Pennsylvania
Minh Than is a third-year Hematology-Oncology fellow at the University of Pennsylvania. He was born in Denver, Colorado. He studied molecular biology at the University of Colorado, Boulder before completing a combined MD/PhD at Yale University. He completed Internal Medicine Residency at the University of Pennsylvania. His current interests include basic and translational science for improving therapeutic strategies for solid malignancies. In his free time, he enjoys rock climbing, board games, and the Philly food scene.

Cecilia Jiang, MD
Radiation Oncology, University of Pennsylvania
Cecilia Jiang is a fifth-year radiation oncology resident at the University of Pennsylvania. She was born in Pittsburgh, PA and grew up in Edison, NJ. She studied biology at the University of Chicago and worked as a hospitalist scribe at Overlook Medical Center in Summit, NJ for a year after graduation. She then completed her medical degree at Emory University School of Medicine. Her clinical interests include radiation toxicity mitigation and imaging. In her free time, she enjoys visiting bakeries, used bookstores, and picnicking in the park.

Jason Han, MD
Cardiac Surgery, University of Pennsylvania
Jason Han is currently a cardiac surgery resident at the Hospital of the University of Pennsylvania. He is in his 8th and last year of training and aspires to be an academic cardiac surgeon with a focus on humanism, education, and writing. He has been recognized for these efforts as the recipient of the Penn Pearl Teaching Award, the Donald Liu Hero of Humanism in Surgery Award, and the Fellowship at Auschwitz for the Study of Professional Ethics. As a medical student and resident, he wrote a monthly column for the Philadelphia Inquirer that combined personal experiences with deeper reflections on patient perspectives. He has written over 80 columns to-date and has been featured at various regional and national meetings such as the “Telling Your Health Story” and “Finding Your Voice” conferences. He has written extensively about his identity as a Korean American Immigrant, and how his background influences, and enhances his interactions with patients. In the academic sphere, his writing about surgical education and culture has been featured in journals such as the New England Journal of Medicine, the Journal of the American Medical Association, and Annals of Surgery.

Sophia Dang, MD
Otorhinolaryngology, Head and Neck Oncologic and Microvascular Reconstructive Surgery, University of Pennsylvania

Justin Ly, MD
Orthopaedic Surgery, Temple University Hospital

Alison Yu, MD
Otorhinolaryngology, Rhinology and Skull Base Surgery, University of Pennsylvania

Jonas Kwok, MD
Pediatric & Internal Medicine, Nephrology Fellow, University of Pennsylvania

Esha Jain, MD
Family Medicine, Cooper Medical School of Rowan University
In addition to her advocacy efforts, Dr. Jain has dedicated significant time to assisting international medical graduates in navigating the residency matching process. Serving as an ambassador for matcharesident, and other companies, she provides invaluable guidance and support to aspiring physicians. Maintaining a commitment to academic excellence, Dr. Jain has contributed to the medical literature through the publication of multiple journal articles. Furthermore, she actively mentors medical students, fostering their intellectual growth and scholarly pursuits.
Central to Dr. Jain’s professional ethos is her unwavering dedication to promoting equitable access to primary care. She espouses a patient-centered approach, characterized by empathy and compassion, in her clinical practice. Moreover, she is resolute in her mission to combat medical misinformation, recognizing its detrimental effects on patient health and well-being. Through her multifaceted contributions, she endeavors to enhance the health outcomes of her patients and their families while advancing the broader objectives of her profession.

Roy Wang, MD
Internal Medicine, University of Pennsylvania

Nilanjan Haldar, MD
Radiation Oncology, Thomas Jefferson University Hospital

Derek Sung, MD, PhD
Anatomic and Clinical Pathology Resident, University of Pennsylvania

Edward Guo, MD
Emergency Medicine, Emergency Ultrasound, Cooper University Hospital

Jason Yuan, MD
Interventional Radiology/ Diagnostic Radiology Integrated Residency, University of Pennsylvania

Linda Xu, MD
Neurology Resident , University of Pennsylvania

Bianca Ho, MD, MSc
Diagnostic Radiology, University of Pennsylvania

Irene Tsai, MD
Internal Medicine, Temple University

Yazid K Ghanem, MD
General Surgery, Cooper University Healthcare
Hometown: Amman, Jordan
Internship: Hospital of the University of Pennsylvania, Perelman School of Medicine
Residency: Cooper University Healthcare (General Surgery)
Clinical Interests: Colorectal Surgery, Surgical Oncology, Minimally Invasive Surgery
Research Interests: Basic Science, New Technology, AI, Outcomes

Steven Pham, DO
Anesthesiology, West Virginia University

Shreya Makkapati MD
Cardiology, Temple University Hospital

Mariam Ansar
Internal Medicine, Cooper University Hospital
Dr. Mariam Ansar is an Internal Medicine PGY-2 Resident physician at Cooper University Hospital, Camden, New Jersey. She completed her medical school from Medical College & Hospital, in Kolkata, India and has worked there in critical care and emergency medicine for 2 years. She is passionate about community outreach internationally and seeks to impact global healthcare. Recently she was part of a global health elective to native communities in Bocas Del Toro, Panama is association with Floating Doctor’s (a nonprofit NGO). Previous year, she played a crucial part in organizing a ‘Winter coat drive’ organized by Cooper at Mount Cavalry Chruch, NJ. She is the co-president of GME Diversity, Equity and Inclusion Council for this session 2024-2025 at Cooper Hospital and is also the founder of Usmle_Helpline, an initiative to mentor students from across the world on a similar journey to residency. She has previously been the College representative for South Asian Medical Student’s Association (SAMSA), Elsevier Student Ambassador, and has organized several health camps in India in association with Child Rights and Youth (CRY) organization.

Eunice Choe, MD
Family Medicine, Thomas Jefferson University Hospital
Hi everyone, I’m Eunice! I’m a PGY-2 Family Medicine Resident at the Jefferson Center City campus. I studied Biology and Health: Science, Society and Policy at Brandeis University. After college, I served as an AmeriCorps VISTA to secure $700,000 in grant funding for a rural behavioral health organization. I then attended SUNY Upstate Medical University, where I contributed over 400 hours of advocacy and community service. Notable moments included representing 17 medical schools at the Medical Society State of New York House of Delegates; teaching medicine to high school students; providing respite to Hospice patients; fundraising for migrant workers; and working with Syracuse University law students to run a COVID-19-based writing competition and publication in the Syracuse Law Review. In 2021, I was awarded the National Health Service Corps scholarship, which paid for two years of medical school in exchange for working as a doctor in a medically underserved community. In residency, I’m working on my MPH at the Jefferson College of Population Health and enjoying going to Washington DC to advocate for our patients. Outside of medicine, I love getting late-night water ice with my church community group, attending free concerts at the Curtis, and going on Philly food adventures with my boyfriend. Would love to talk to you about health advocacy and medicine!

Jessica Yang, DO
Family Medicine, Bryn Mawr Hospital
Jessica is a second-year family medicine resident at Bryn Mawr Hospital. She attended Case Western Reserve University for college and received her medical degree from Rowan University School of Osteopathic Medicine in New Jersey. She also doubled as a writer who covered Asian American literature for various publications and explored her identity as a Chinese American immigrant. Her writing has been featured in Zora, Los Angeles Review of Books, and many other publications. In her free time, she enjoys traveling and visiting museums.

Zoha Shahabuddin, DO
Pediatrics, Saint Christopher’s Hospital for Children
Hi! I’m a PGY-2 in the Pediatrics Residency Program at Saint Christopher’s Hospital for Children in Philadelphia. I’m a proud New Jersian, went to Columbia University for undergrad where I majored in economics, and went to Rowan School of Osteopathic Medicine for medical school. I plan to apply for pediatric gastroenterology fellowship after residency. Some of my hobbies are traveling, hiking, painting (not well!), and exploring Philadelphia on foot (you never know what interesting things you’ll stumble across). I‘ve been passionate about creating spaces for dialogue about Asian American identity and the Asian American experience since undergrad, both inside and outside the context of medicine. I hope to use my career to support diverse voices and advocate for diverse needs.

TingAnn Hsiao, MD, MPH
Psychiatry, Cooper University Hospital
TingAnn Hsiao is a first year psychiatry resident at Cooper University Hospital. She was born in southern New Jersey. For college, she attended Cornell University and completed a major in Human Biology, Health, and Society and a minor in Health Policy. Afterwards, she pursued her MD/MPH at Thomas Jefferson University. During medical school, she conducted qualitative research and completed her master’s thesis on fentanyl test strips and other harm reduction strategies in the Emergency Department. Her current clinical interests include consult-liaison and addiction psychiatry. Outside of clinical work, she enjoys fostering cats and taking care of her houseplants.

Monica Nguyen, MD
Internal Medicine, Lankenau Medical Center

Robert "Robi" Francis Talaue Bucayu, MD, MPH
Pediatric Infectious Disease, Children's Hospital of Philadelphia
Pre-Health Panel

Sharon Kim
MSN Candidate, Johns Hopkins

Louise Paed
Pharmacy Student, Saint Joseph's University, Philadelphia College of Pharmacy

Julia Ossman
Pharmacy Student, Saint Joseph's University, Philadelphia College of Pharmacy

Christopher Xie
Medical Student, Sidney Kimmel Medical College
Christopher grew up in Chappaqua, New York, and attended Haverford College, where he majored in biology and competed in men’s foil as part of the fencing team. After graduation, he spent three years researching breast cancer therapeutics at Thomas Jefferson University, which deepened his passion for medicine and solidified his commitment to the field. Currently, Christopher is a second-year medical student at Sidney Kimmel Medical College. He serves as the president of APAMSA at Jefferson, which focuses on addressing healthcare disparities, promoting health equity, and advocating for AAPI health issues. He is also actively involved in JeffHOPE, a student-run organization that provides free healthcare services to underserved and homeless populations in Philadelphia as a Screening and Procedures CM at Our Brother’s Place.

Anuhea Leite-Ah Yo
Physician Assistant Student, Drexel University
Anuhea Leite-Ah Yo, a proud Native Hawaiian, is currently in her clinical year as a Physician Assistant student at Drexel University. Born and raised in Hilo, Hawaii, she graduated from Kamehameha Schools: Kea’au in 2014 and later earned her degree in Biology, with a minor in Psychology, from Wells College in New York. Along her journey, she gained valuable experience working as an EMT-B, Physical Therapy aide, Chiropractic aide, and Registered Behavioral Technician, each role deepening her love for caring for others.
In her free time, Anuhea enjoys being in the ocean surfing, playing volleyball, and cooking with her ‘ohana and friends. Her heart has always been with her Native Hawaiian community, who have helped her become who she is today. Anuhea’s path in medicine is driven by her desire to bring knowledge and care back home to Hawai’i, where she hopes to serve those who need it most and continue the spirit of aloha.

Christine Bae
Dental Student, University of Pennsylvania

Andrew He
Physical Therapist
Andrew attended University of the Sciences in Philadelphia for his undergraduate studies and earned his Bachelor’s of Health Sciences in 2020. He then continued to pursue a career in physical therapy and graduated with his Doctorate in Physical Therapy at Saint Joseph’s University in May 2023.
Andrew has a strong passion for helping others and loves to treat patients with a variety of orthopedic conditions. He enjoys treating athletes and would love to work with more as he begins his career. He would like to pursue continuing education courses to further specialize in athletic rehab as well as TMJ dysfunction, lumbar spine, and cervical spine rehabilitation.
He would describe himself as an “optimistic individual with a sense of humor”. Andrew was a former high school varsity tennis player and continues to play tennis recreationally as well as basketball and football at a recreational level. He loves fishing and is an avid Philly sports fan.
Address
Drexel University Health Sciences Building (60 N 36th St, Philadelphia, PA 19104)
Parking
The nearest parking lot is LOT G at 3330 Market Street. On weekends it is $14 per day starting at 5 AM.
Evenings 10 PM-5 AM: additional $8 fee applies.
Directions into the parking lot:
Enter the Garage on Ludlow Street.
Please pull at ticket to enter Garage. Payment is required before exiting the Garage. To leave facility, please pay at kiosk in lobby or at kiosk at exit ramp inside your vehicle. You must exit within 15 minutes of payment. If you encounter any issues, please use the help button located on the payment kiosk
To pay:
- Use your ticket and a credit card or cash at the first floor kiosk located in lobby, entrance off of Market Street
- Use your ticket and a credit card at the exit gate
- Text PAY to 321.341.2288 for one-time payment or to establish a secure profile
You can find more detailed information and FAQs regarding parking on Drexel’s website.
There is also street parking available within walking distance, although it may not always be available.
Accommodations
The Drexel University Health Sciences Building is located in University City. There are some locations nearby, listed below, but we encourage you to reach out to local students for more affordable accommodations. There may also be more affordable options in Center City and other areas in Philadelphia if you are willing to travel.
Sheraton Philadelphia University City Hotel
3549 Chestnut Street, Philadelphia, Pennsylvania 19104
Homewood Suites by Hilton University City Philadelphia, PA
4109 Walnut St, Philadelphia, Pennsylvania 19104
The Inn at Penn, a Hilton Hotel
3600 Sansom Street, Philadelphia, Pennsylvania 19104
We are excited to offer an opportunity for you to present any research that you have been involved in at our Region III conference this year.
We hope this can be a space where we can showcase and appreciate the amazing work everyone has been involved in. Abstracts presented at other conferences or published in journals can still be submitted for review. We welcome submission of all topics!
For more information and to submit an application, please click the link below.
National Board

Stephen Chien
Region III Director
Drexel University College of Medicine

Jeffrey Wang
Region III Director
Drexel University College of Medicine

Sandy Yang
Region III Director
Sidney Kimmel Medical College

Jessica Hseuh
Co-Membership VP
Georgetown University School of Medicine
Local Chapter Leadership: Drexel Univeresity College of Medicine and Temple University

Lillian Phung
DUCOM APAMSA Co-President

Lucy Zhou
DUCOM APAMSA Co-President

Kevin Lim
DUCOM APAMSA Advocacy and Education Chair

Winni Gao
DUCOM Advocacy and Education Chair

Bobby Van
DUCOM APAMSA Community Service Chair

Celter Odango
DUCOM Community Service Chair

Sharon Shania
DUCOM APAMSA Social Chair

Olivia Nguyen
Temple University Pre-Medical APAMSA President
Contact Us
Questions? Email us at region3@apamsa.org
2024 Region VII Conference

Proud to be AANHPI: Building Bridges, Empowering the Community
Date: Saturday, September 21, 2024
Location: University of Arizona, College of Medicine – Phoenix | 475 N 5th St, Phoenix, AZ 85004
Registration Details: Click below for more info
On behalf of the University of Arizona College of Medicine-Phoenix APAMSA, we are delighted to welcome you to sunny Phoenix for APAMSA’s Region VII Regional Conference!
Hosting this conference in Arizona for the first time is a unique and exciting opportunity. While Asians are the smallest minority group in our region, we are also the fastest-growing. This growth underscores the essential need to establish and strengthen our community. This year’s theme, “Proud to be AANHPI: Building Bridges, Empowering the Community,” reflects our commitment to fostering unity and presence within the Asian community in our region.
This conference is not just a celebration of our Asian identity; it is a platform for sharing experiences, building connections, sparking collaboration, and empowering each other to develop a strong identity both individually and as a community, despite demographic challenges.
We have worked diligently to create a conference filled with inspiring talks from community leaders, invaluable networking opportunities, and skill-building workshops. We have invited a diverse array of local speakers who will educate, inspire, and empower us to unite and advocate for our community.
We hope you enjoy your time here, build meaningful connections, learn from one another, and leave with a sense of belonging and cultural pride.
Proud to be AANPHI: Building Bridges, Empowering the Community
Hosting the Asian Pacific American Medical Student Association (APAMSA) Regional Conference in Arizona presents a unique and transformative opportunity. Unlike regions such as California, where connecting with Asian culture and identity is more accessible due to larger Asian populations, Arizona’s predominantly white and Hispanic demographic poses significant challenges for Asian individuals seeking a sense of community and belonging. By organizing this inaugural regional conference in Arizona, we aim to ignite a movement that strengthens the presence and unity of the Asian community here. This event is not merely about celebrating Asian identity; it is about fostering connections, sharing experiences, and empowering attendees to cultivate a robust identity despite demographic challenges. The conference will provide invaluable networking opportunities, skill-building workshops, and inspiring talks, all designed to help medical students and professionals forge a stronger sense of self and community. This initiative extends beyond Arizona, recognizing that many regions across the nation also lack substantial Asian populations. By addressing these shared challenges, we hope to inspire a nationwide effort to build resilient and supportive Asian communities, ensuring that all individuals, regardless of their location, can experience a profound sense of belonging and cultural pride.
Saturday, September 21, 2024
8 AM: Check-in / Registration
8:45 AM: Introductions and Greetings
9:15 AM: Keynote Speaker – Dr. Paul Tran, MD
10 AM: Speaker Session #1 – Dr. Vivian Huang, MD MPH
10:45 AM: BREAK
11 AM: Speaker Session #2 – Dr. Alice Lee, MD
11:45 AM: Speaker Session #3 – Dr. Rosanne Kho, MD FACOG
12:30 PM: LUNCH
1:20 PM: Research Poster Session
2 PM: Skill Building Session #1 / PREMED Abbreviated Doctoring
2:45 PM: BREAK / Transition Period
2:50 PM: Skill Building Session #2 / PREMED Abbreviated Doctoring
3:35 PM: BREAK
3:45 PM: All of Us Session w/ Dr. Yugay
4:05 PM: NMDP Session
4:15 PM: Closing Remarks + Raffle
6 PM – evening: Happy Hour Dinner Event
Stay tuned as we reveal more speakers!

Dr. Paul Tran, MDPediatric Gastroenterologist
Phoenix Children’s Hospital
Paul Tran is a pediatric gastroenterologist at Phoenix Childrens, where he has been practicing since summer of 2022 after finishing his fellowship training in Pediatric Gastroenterology at Children’s Hospital Colorado. He earned his medical degree from University of Colorado School of Medicine and completed pediatric residency at Children’s Health/University of Texas Southwestern in Dallas Texas.
He considers himself a dedicated medical educator, with formal roles as a Pediatric Clerkship Co-Director and doctoring faculty at UACOMP and Clinical Skills faculty at Creighton University. He is passionate about mentoring and coaching medical students, residents, and fellows and promoting a culture of kindness, encouragement, and empowerment in medical education. Outside his practice, Dr. Tran enjoys spending time with his wife and two sons – exploring the outdoors and trying out new restaurants. Paul also enjoys connecting with a broader audience through social media, where he shares his experiences and insights in the medical field.

Dr. Rosanne Kho, MD, FACOGProfessor & Chair
Department of Obstetrics and Gynecology
University of Arizona College of Medicine - Phoenix
Banner - University Medical Center Phoenix
Dr. Rosanne Kho serves as Chair of the Department of Obstetrics and Gynecology at the University of Arizona College of Medicine Phoenix. Prior to 2023, she was Head of the Section of Medical Gynecology and Minimally Invasive Gynecologic Surgery (MIGS) at Cleveland Clinic in Ohio. She is board certified in Obstetrics and Gynecology and sub-specialty board certified in Female Pelvic Medicine and Reconstructive Surgery (FPMRS). Dr. Kho focused her clinical and academic career in the field of pelvic surgery. She was involved in the early use of robotics in gynecology and had published on the techniques and appropriate application of the technology. She writes and teaches extensively on the adoption of surgical innovation and techniques to facilitate the performance and teaching of vaginal hysterectomy. She served for 10 years as one of four senior editors for the Journal of MIGS (2022 IF 4.3). In 2015, she founded the FMIGS subsection of the Fellows Pelvic Research Network, a fellows’ forum with senior mentorship for the conduct of multicenter trials to elevate the quality of fellows research work in MIGS. She has over 90 publications in peer-reviewed journals and book chapters and serves as research mentor for the residents and fellows.
Dr. Kho also served as the fellowship director for FPMRS and later in MIGS at Mayo Clinic in Arizona, Columbia University Medical Center in New York. In 2015-2017, as president of the fellowship in MIGS, she organized teams to revamp the fellowship program site requirements, learning goals and objectives, core curriculum and reading list. Additionally, the formal process to seek ABOG recognition of MIGS as a focused field in OB/GYN was instituted.
She currently serves as the President for the Society of Gynecologic Surgeons. She was recently appointed as the Director of AAGL Practice Guidelines Committee for the development of clinical practice guidelines in MIGS.

Dr. Peter Nakaji, MDProfessor & Chair
Neurosurgery
University of Arizona College of Medicine - Phoenix
Banner - University Medical Center Phoenix
Peter Nakaji, MD, is an internationally known neurosurgeon, who has published more than 200 peer-reviewed papers and holds more than two dozen patents. Dr. Nakaji has received a number of teaching awards and has served for nearly a decade as the program director for the Neurosurgery residency at Barrow Neurological Institute. In his current role as department chair and program director for the Neurosurgery residency at Banner Health, Dr. Nakaji extends neuroscience training for medical students, residents and fellows. In addition to treating complex diseases of the brain, Dr. Nakaji is a pioneer in the area of neuroendoscopy for “keyhole” treatment of conditions such as trigeminal neuralgia and colloid cysts. He has a passion for technically demanding brain surgery and is a respected authority in the treatment of aneurysms, arteriovenous malformations, cavernous malformations, moyamoya disease, extracranial-intracranial bypass, carotid artery disease, as well as brain and skull base tumors. Dr. Nakaji completed his residency at the University of California – San Diego. He received additional fellowship training in endoscopic neurosurgery at the Centre for Minimally Invasive Neurosurgery in Sydney, Australia, under the direction of Charles Teo, MD. He completed a second fellowship in cerebrovascular and skull base surgery at Barrow Neurological Institute at Dignity Health St. Joseph’s Hospital and Medical Center in Phoenix under Robert Spetzler, MD, before joining the staff as an attending neurosurgeon in 2004.

Dr. Alice Lee, MDEmergency Medicine Physician
University of Arizona College of Medicine - Phoenix
Dr. Alice Lee is an emergency physician in Mesa, AZ. She received her medical degree from SUNY Upstate Medical University, graduated from Creighton University EM Residency (formerly Maricopa Medical Center EM Residency) and has been in practice for 32 years. She is highly experienced in the care of geriatric emergencies, emergent airways, ED acute stroke care, and ED cardiopulmonary resuscitations. In 2017, she joined the University of Arizona College of Medicine-Phoenix faculty as an Assistant Clinical Professor where she assists in the Simulation Lab and the Anatomy Lab. In 2023, she added to her breadth of expertise by working as an aviation telemedicine physician consultant for MedAire/MedLink, Phoenix, AZ, providing medical direction in real-time for in-flight medical events. She is passionately bringing awareness of the little known health disparity of lung cancer in nonsmokers in the AANHPI population since surviving the disease in 2021. She has appeared on KevinMD podcasts and given lectures on this topic. She was born in Taiwan and immigrated to the US with her family at the age of 9. She is competent in conversational Chinese (Mandarin.)

Dr. Vivian Huang, MD, MPHInternal Medicine and Preventive Medicine
Vivian Huang, MD, MPH is dual boarded in internal medicine and preventive medicine with over 10 years experience in clinical medicine, international & domestic public health. She has a Masters of Public Health from Columbia University Mailman School of Public Health. Vivian’s domestic current and past experience includes working to support Native Americans in the US Southwest; in large urban hospital systems; academic centers; New York City Health Department and Federally Qualified Health Center. Vivian’s international experience includes working with Doctors Without Borders (Syria & Swaziland), Partners in Health (Sierra Leone), Columbia University Global Brigades (Honduras) and The Marshall Islands Government. Dr. Huang’s specialties/interests are Internal Medicine, Public Health, TB, Diabetes, Hepatitis B, Ebola, Immunizations, Vulnerable Populations/Health Inequities. She speaks 3 languages: English Mandarin Chinese and Spanish. She enjoys scuba/free diving, yoga, running & hiking.
Directions to the Venue
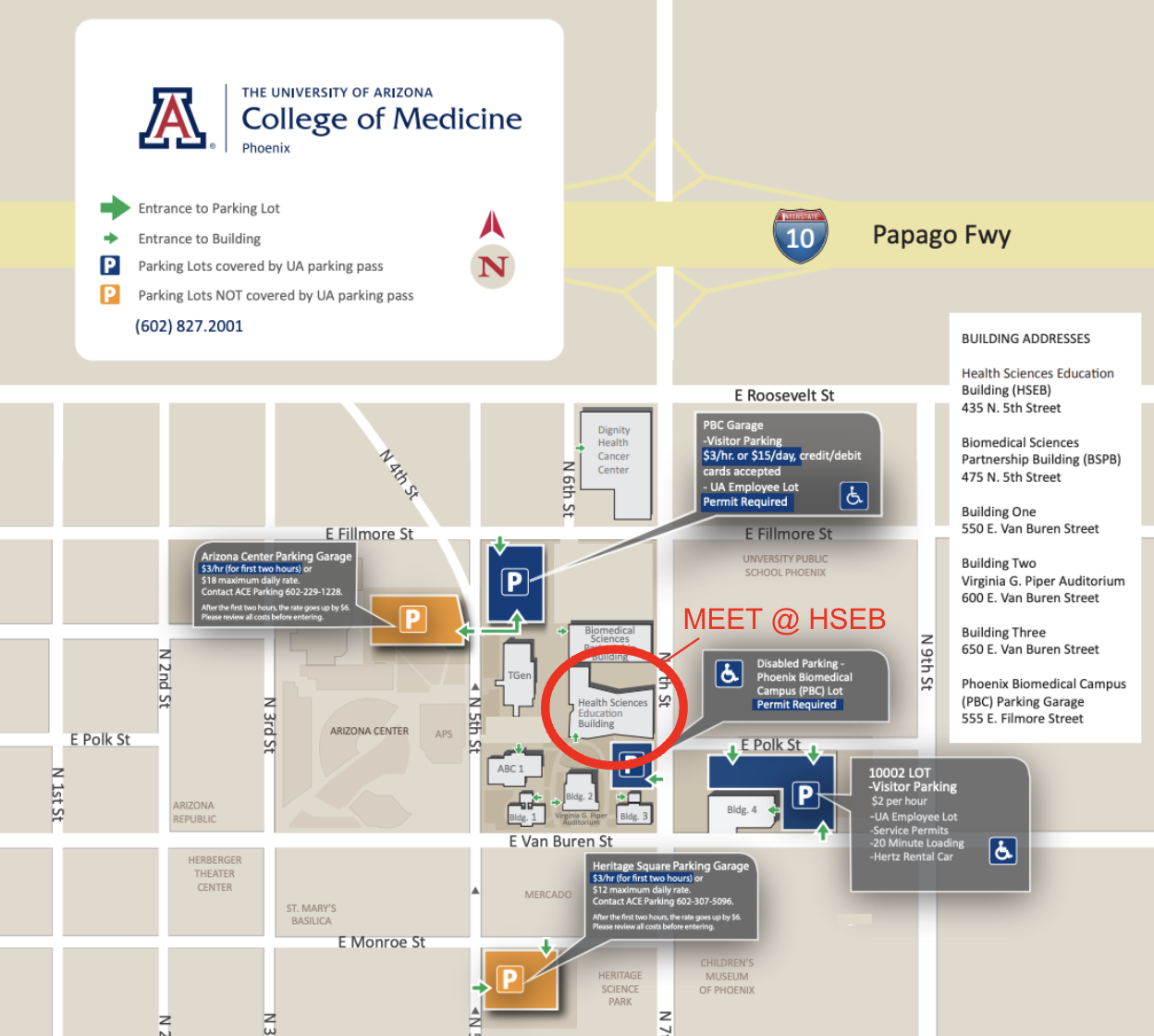
Campus Map
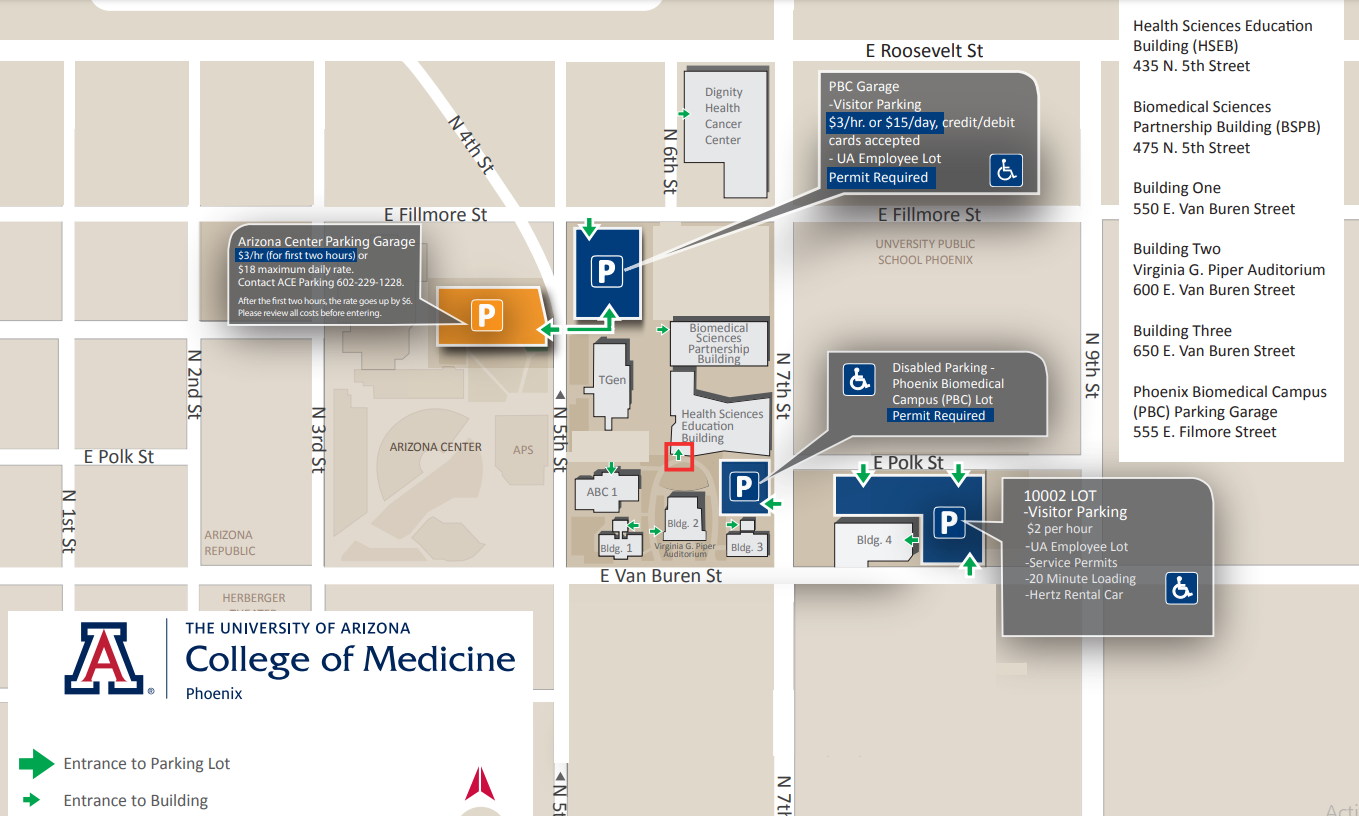
Featured Abstracts and Accepted Posters
Taylor Lee – “Digital Marketing Trends Amongst Members of the American Academy of Facial Plastic and Reconstructive Surgery (AAFPRS)”
Krishna Sinha – “Dedifferentiated Liposarcoma in the Head and Neck With Free Tissue Transfer Following Wide Surgical Excision: A Case Study”
Nhat Nguyen – “Feasibility study of artificial intelligence-based geriatric assessment study”
Cathleen Huang – “Automatic motion correction for myocardial blood flow estimation improves diagnostic performance for coronary artery disease in 18F-flurpiridaz PET-MPI”
Sophie Nguyen – “A magnetorobotic capsule for liquid cargo delivery to the gastrointestinal tract for treating microbial dysbiosis”
Adam Lin – “Clinically Significant Prostate Cancer Detection by Transperineal vs. Transrectal Magnetic Resonance Imaging Fusion Targeted Biopsy: Performance Among Possible Focal Therapy Candidates”
Justin Le – “Assessing and Improving Confidence of Medical Students Entering Residency with a Preparation for Residency Boot Camp Course”
Candice DeCuna – “Time Restricted Eating in Alzheimer’s Disease (TREAD): a Pilot Study”
Stacey Lin – “Cultural Competency and Inclusion at Creighton University SOM: Exploring Perspectives of Asian American and Pacific Islander (AAPI) Medical Students on Representation in Medical Education”
Shide Zhang – “Highlighting the AANHPI Medical Student Experience: A Scoping Review of the Literature Since The Start of the 21st century”
Hannah Lew – “Expression Pattern of Genes of Daphnia pulex Tissues at a Single-cell Resolution”
National Board

Thy Nguyen, OMS-I
Region VII Director, Registration Liaison
A.T. Still University – School of Osteopathic Medicine in Arizona

Phil Nguyen-Powanda, MS-III
Region VII Director
University of Arizona – College of Medicine (Phoenix)

Lyndon Bui, MS-IV
Region VII Director
University of Arizona – College of Medicine (Phoenix)

Amelia Huynh, OMS-IV
Membership Vice President
Pacific Northwest University – College of Osteopathic Medicine
Local Chapter Leadership

Stephen Yao, MS-III
Director of Conference and Planning
University of Arizona – College of Medicine (Phoenix)

Brittnay Hong, MS-III
Director of Conference and Logistics
University of Arizona – College of Medicine (Phoenix)

Euwie Park, MS-II
Director of Speaker Relations
University of Arizona – College of Medicine (Phoenix)

Khang Dao, MS-III
SIM Workshop Director
University of Arizona – College of Medicine (Phoenix)

Taylor Lee, MS-II
Doctoring Workshop Director, Director of Marketing and Design
University of Arizona – College of Medicine (Phoenix)

Chynna Nguyen, MS-II
Volunteer Liaison
University of Arizona – College of Medicine (Phoenix)

Van Dexter Calo, MS-II
Director of Communications
University of Arizona – College of Medicine (Phoenix)

Victoria Wang, MS-II
Director of Research
University of Arizona – College of Medicine (Phoenix)

Teresa Tran, MS-II
Director of Marketing and Design
University of Arizona – College of Medicine (Phoenix)

University of Arizona – College of Medicine (Phoenix)
Office of Equity, Diversity, and Inclusion
Contact Us
QUESTIONS? Email us at region7@apamsa.org!
2024 Region V Conference
Join us on Saturday Oct 19th, 2024 in Columbus, OH at Hamilton Hall (1645 Neil Ave, Columbus, OH 43210) for our Regional Conference as we discuss the role of doctors as advocates and storytellers in medicine and how we are able to create change within our communities. We hope to see you there!Registration is now CLOSED!
What stories are we choosing to tell? Whose stories are we not telling? And why are we telling them?
As doctors, we are the advocates and storytellers for our patients and communities; we should strive to give voices to those that are unheard and make space for difficult discussions about the physical and mental health of the people we serve. As members of a greater APIDA community, here too should our advocacy continue, and even still beyond the APIDA community.
In this way, what does APIDA advocacy mean when we do not center the oppressed in our stories? How far does our solidarity extend?
Whether it is the barriers to health millions of APIDA immigrants face trying to access care in the U.S. or the systematic bombing of hospitals in Gaza, we must be thoughtful in who we are choosing to talk about. There is no APIDA liberation without liberation of the oppressed, of those of the global majority. We must share these stories and many others as continue to understand who we are as an APIDA community and who we are as storytellers.
8:30 AM – Registration
9:00 AM – Opening Statements and Keynote Address by Dr. Anita Somani, MD
10:30 AM – First Break-Out Session
1: Culturally Competent Care for the Muslim Community — Ridha Anjum, MS-II
2: Advocacy 101 Workshop — Julianna Sim, MS-IV
3: Dr. Anh Thu Thai from Ohio Asian American Health Coalition
11:30 AM – Second Break-Out Session
1: Suture Clinic with Drs. Sayat
2: Hepatitis B in the Asian-American Community — Sophia Negash, MPH & Thanh Ma
12:30 PM – Lunch and Poster Presentations
2:00 PM – Third Break-Out Session
1: Physician Panel
2: Medical Student Panel
3: Cultural Framework with Liz Young
3:00 PM – Closing and Raffles!
Keynote Speaker

Dr. Anita Somani, MDOB/GYN at Ohio Health
State Representative for Ohio
Dr. Anita Somani is currently serving her first term as State Representative for Ohio’s 11th House District, which includes the cities of Dublin and Hilliard. She is running for re-election in District 8 which encompasses Worthington and parts of Dublin and Columbus.
For the last 32 years, Dr. Somani has worked in Columbus as a highly respected healthcare professional, currently as an OBGYN at OhioHealth. She earned her M.D. from the Medical College of Ohio and completed her residency in OB/GYN at Mt. Carmel Medical Center in Columbus. She has her certification in Minimally Invasive Gynecologic Surgery( MIGS). Dr. Somani is a past board member of the Columbus Medical Association and Planned Parenthood. She is currently a Board Member of LEAD Ohio.
Dr. Somani ran for office because she believes the state of Ohio has gone down the wrong path regarding prominent issues such as health care, increasing abortion restrictions and the loosening of gun laws, all of which disproportionately affect marginalized communities. As a physician and legislator, she has used her medical background to improve the public health of our state and to create evidence-based legislation that helps everyone in our community. She serves on the Health Policy, Health Providers, Families & Aging and Insurance Committees. She is the ranking member on Health Providers. She has sponsored many health related bills including the Reproductive Care Act (HB343), the Protect IVF technology(HB502) and the funding of Crisis Pregnancy Centers(HB565). She strongly believes in the separation of church and state. Public school funding should not go to school vouchers.
Dr. Somani lives in Columbus with her husband where they raised their son, an engineer and their daughter, an OB/GYN. She is a first-generation immigrant from India, and her father was the first Asian to serve in a Governor’s cabinet. On a personal level, she has completed 10 half marathons and still enjoys running. She is an avid reader and one of her biggest stress reducers is baking.
Workshop Speakers
Stay tuned as we reveal more speakers!

Dr. Linbee Sayat, MDAvina Women's Care
Assisting women through pregnancy and birth and optimizing a woman’s health status through the tumultuous changes that can occur during her life are both reasons Dr. Linbee Sayat loves being an OB/GYN. Dr. Sayat studied biochemistry at the University of Notre Dame and received her medical degree from The Ohio State University College of Medicine. During medical school she was inspired to pursue OB/GYN thanks to a rotation she spent at a rural Ohio hospital performing deliveries as well as a mission trip to the southern Philippine islands where she was able to participate in gynecological surgeries in a primitive setting. Dr. Sayat spent her first post-grad years as a physician at the Columbus Neighborhood Health Centers where she worked to meet the access to healthcare challenges of the underserved. She then served for a decade as teaching faculty at The Ohio State University Department of Obstetrics and Gynecology. She joined Avina Women’s Care in 2014 and has continued in private practice since that time. Dr. Sayat’s husband Jason is also an OBGYN physician at Avina Women’s care. They have 2 grown children, Jacob and Alana.

Dr. Jason Sayat, MDAvina Women's Care
For Dr. Jason Sayat, the decision to become a doctor was simple. From an early age, his mother, an obstetrician and gynecologist, and his father, a general surgeon, exposed him to medicine. Raised in Cambridge, Ohio, Dr. Sayat studied biology and neuroscience at Duke University. He then moved back to his home state to complete his medical training and later residency at The Ohio State University. Prior to joining Avina Women’s Care, he was in academic practice at The Ohio State University Wexner Medical Center. His specializations include minimally invasive gynecologic surgery, robotic surgery, in-office procedures and general women’s healthcare. Today, Dr. Sayat resides in Columbus with his wife, also a physician within our practice, and two children.

Dr. Anh Thu Thai, DHA, RRTOhio Asian American Health Coalition
Dr. Anh Thu Thai is from Columbus, Ohio. She has a background in respiratory therapy and her master’s and doctorate in healthcare administration. She currently works at The Ohio State University in research focused on adolescents and mental health. She serves as the Executive Director of the Ohio Asian American Health Coalition and is an active member of the American Public Health Association as the Caucus Director for Asian and Pacific Islanders. Her professional interests focus on addressing health disparities for Asian Americans, immigrants, and refugees. A few of her projects include: Discover Feminine Kits and Education for Mothers and Daughters, Franklin County Public Health Covid-19 Care Kits, Ohio Department of Mental Health & Addiction Services Mental Health Resource Guide and a Statewide Mental Health Providers Directory, and USAging Vaccine Initiative for Seniors.

Liz YoungInter-Change Consultants
Elizabeth Miu-Lan Young co-founded InterChange Consultants in 1987.
She is a specialist in cultural competencies training focusing on diversity issues at work. She has been active in the New York City Asian American Community for the past 40 years. One of the organizers of the initial Chinatown Health Fair which eventually led to the establishment of the Chinatown Health Clinic (now called the Charles B. Wang Community Health Center), she also taught the pilot Asian American Experience course at Hunter College and the University of Southern California. Liz served as the first Director of Project Reach – a Chinese-American Planning Council program working with Chinatown at-risk youth. She also worked in a garment sweatshop to better understand the immigrant experience. She was a senior research associate with an Affirmative Action consulting firm headed by Dr. Kenneth Clark.
Liz has presented “Political Savvy” and “Kick Butt!! Just Not Your Own” workshops for affinity groups of color at Lucent Technologies, AT&T and Verizon. She has co-facilitated similar courses in Hong Kong and Jakarta and provided cross-cultural teambuilding and civil-capacity building in East Timor.
She has also trained administrators, faculty and students in cultural competencies at Fashion Institute of Technology, Harvard, Yale, Columbia, New York University, Spelman, Princeton, the University of Connecticut, Brown University, Columbia University School of International and Public Affairs and new medical/dental students at Stony Brook University School of Medicine.
For the NCAA, Liz has co-facilitated the weeklong Leadership Intensive for the Leadership Institute for Ethnic Minorities and Division III’s groundbreaking Ethnic Minority and Women’s Internship Program joint orientation for interns, their supervisors and mentors. She currently serves as a staff developer with the Morningside Center for Teaching Social Responsibility, training public school educators, staff and students in restorative practices and Social and Emotional skills.
She is a graduate of the University of California at Berkeley and has received extensive training in Organizational Development.

Karen Jiobu, DLMHealth Care Advisor for Asian American Community Services
Karen Jiobu, DLM (ASCP), presently is a Health Care adviser, served as an Interim Executive Director (2018-2021) of Asian American Community Services ( founded in 1976) and continues to serve the Asian American community. www.aacsohio.org. Her community service started as a volunteer with the Asian Festival (29 years) serving as the Vice chair of the first board, treasurer and performance chair. She also started the Asian Festival Dragon Boat race event in 2010. She started screening for hepatitis B in 2006 at the Asian Festival and after 2008 at AACS, working with OSU medical students and the Asian and Somali ethnic communities has facilitated over 2000 screenings. She was awarded the Hepatitis B United Champion Award in 2013 in Washington, D.C. for her work in education, awareness, screening, and linkage to care for hepatitis B. and currently serves as an adviser at the National Hepatitis B Task Force. She was inducted into the Senior Citizens Hall of Fame in 2020 for her work with hepatitis B as well as her speaking about the Japanese American Internment in schools, libraries, and other organizations . On March 26, 2024, Karen was presented the Community Action Award by the Ohio Commission on Minority Health.
Prior to her retirement and community service she was Laboratory Director at Mount Carmel Health System starting out as a medical technologist then supervisor of Microbiology and then lab director of 100 staff associates and 10 managers. She was instrumental in the consolidation of the laboratories at Mount Carmel West, Mount Carmel East, and St Ann’s Hospitals and then becoming the Director of the Rapid Response Laboratories at all 3 hospitals before retirement. She worked as a technologist at the Los Angeles County General Hospital, Norfolk General Hospital (Virginia) and the Bellin Memorial Hospital (Green Bay, Wisconsin)

Julianna Sim, MS4DEI Officer for AMA MSS
and currently serves as the Diversity, Equity, and Inclusion (DEI) Officer for the American
Medical Association Medical Student Section (AMA MSS). In this role, she is leading initiatives
that promote inclusivity and address disparities within the medical field. Her work involves
developing and implementing programs aimed at increasing student representation and uplifting
voices of those underrepresented in medicine.
Julianna’s commitment to DEI stems from her multicultural background of Filipino and Chinese
descent. Through her role with the AMA MSS, she collaborates with physicians, residents, and
medical students to create a more equitable environment. She hopes that her efforts as DEI
officer will improve access to opportunities in medicine.

Ridha Anjum, MS2Volunteer Coordinator for the Noor Community Clinic

Sofia Negash, MPHProgram Coordinator of AACS Hepatitis B Mini Grant
Sofia Negash is the current Program coordinator of the AACS Hepatitis B minigrant. She is a recent OSU Master’s of Public Health Graduate. At this year’s Asian Festival, she contributed to enhancing data collection improvement and storage for the APIDA community for the Columbus Asian Festival.

Thanh MaAACS Program Coordinator and Manager for Asian Free Clinic
My name is Thanh Ma, the oldest son of the ten siblings. Growing up in the South Vietnam, I completed
the 7 th grade schooling. My father was an official of the South Vietnam government.
I set out a journey as one of “the Boat people” for the whole family to escape from Vietnam since the
Communist controlled. Came to the United States, in February 1985 my first job was at the Baker Pride
Oven Co. as a beginner welder > Machinist > Leadman of the Machine department. Working in the day
time, ESL class in the evening for about 2 hours a week, I obtained a GED certificate in May 1987 from
City of New York Board of Education. Enrolled in Rockland Community College in 1988 and College Of
Aeronautics in Flushing New York in 1989. School in the day time and work in the evening, at night and
weekends to support myself and my family. Graduated with a Bachelor’s degree in Aeronautical
Engineering in May 1993.
In September 1993, I entered in to the competitive and challenging world, got a job as an IT
Engineer. Work and continue education, gained a Master’s degree in Computer Networking in August
1998. In 2000, I worked at Cap Gemini, Earnest and Young as a Technical Support manager Data Center
NY-NJ that supported Beth Israel Medical Center, St. Luke and Roosevelt Medical Center, Long Island
College Medical Center, King Highway Hospital and many other hospitals within the network. In 2006, I
set out as a business investment until today. The Covid-19 really turned things upside down. Starting
from the COVID-19 outbreak, I have worked with different charities and volunteer agencies and now I
am with Asian American Community Services (AACS) as a coordinator and program manager for Asian
Free Clinic.
Life is very interesting, sometimes things go well “nice and smooth” other times things rough like an
“angry ocean!”

Dr. Andrew Keaster, MDPoster Evaluator

Dr. Steven Ing, MDPoster Evaluator
Panelists

Dr. Justin Jiang, MDInternal Medicine Resident at OSU
Justin is a graduate of OSU College of Medicine, where he served as a former chapter president of APAMSA. He plans on pursuing Hem/Onc fellowship after residency.

Dr. Cristiane Ueno, MDPlastic Surgeon at Ohio State University
I am a plastic surgeon who specializes in reconstructive procedures, including general reconstruction, top surgeries for transgender patients and breast reductions. When patients come to see me, they can trust that I will care for them as I would my own family members.
My enthusiasm for plastic surgery began in medical school when I learned how reconstruction could significantly improve quality of life for burn patients and I have felt called to this specialty ever since. It is a privilege to use my skills to help bring a sense of normalcy to patients impacted by trauma, cancer or a congenital anomaly.
I am also passionate about transgender care and helping people become their true selves. I serve as co-chair of the outreach program for The Ohio State University Wexner Medical Center’s LGBTQ+ employee resource group and volunteer at community events. My research is focused on reducing health care disparities and expanding medical education to underserved groups.
In addition to my clinical work, I am the associate program director for the Plastic Surgery Residency Program and an advisor for the Plastic Surgery Interest Group at Ohio State. I love working in academic medicine because helping to train and inspire future generations is one of the most fulfilling opportunities available.
When I am not working, I enjoy spending time with my family, traveling, volunteering and meeting new people. I stay active and healthy by running, which helps me regroup and focus on what truly matters. I also enjoy a good cup of coffee and trying diverse types of food.

Dr. Simran ChahalInternal Medicine/Pediatric PGY-2 at OSU
I’m originally from California, but I came to Ohio for medical school. I am planning to be a dual hospital for Medicine and Pediatrics after graduation. My academic interests include medical education and advocacy.
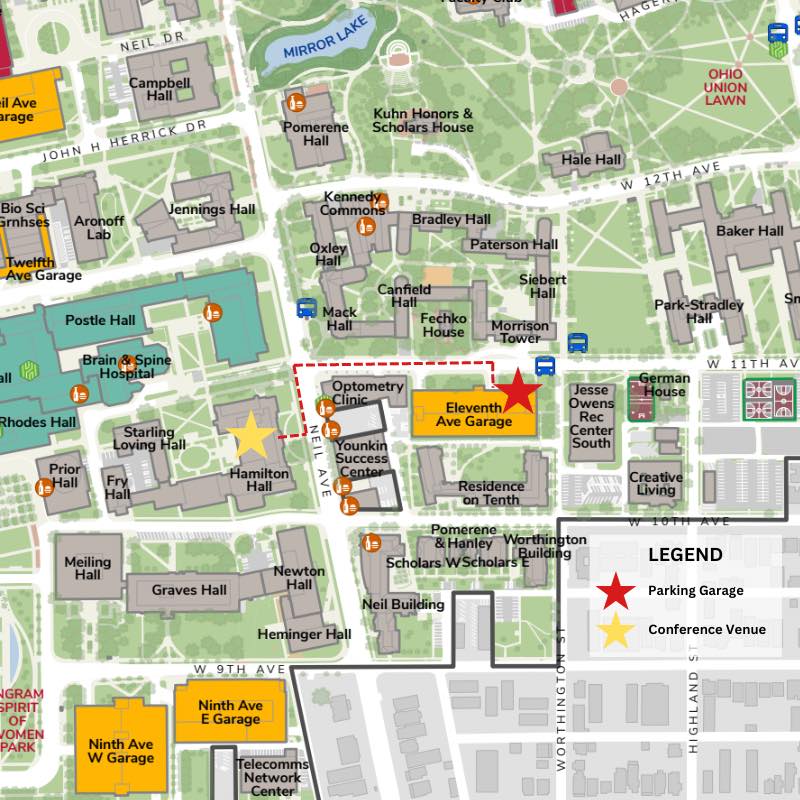
Parking is $14.50 per day. If interested in receiving a discount at $11 per day, please fill out the below form!
Must be completed by Oct 16th.
Accepted Posters
Impact of the Dobbs Decision on Abortion Rates, Preventive Measures, and Pregnancy Outcomes Across Racial Groups: A Large Public Health Database Analysis
Daniel B. Chen B.A., Arnav Mahajan MD, Fiona Cherry B.A., David Hackney MD, Helen Wong MD
Case Western Reserve University School of Medicine
Insufficient Sleep in Ohio and Its Complication in Risky Behaviors
James Dai, Jackson Mitchell, Jeannette Manger
Wright State University Boonshoft School of Medicine
Use of fluocinolone acetonide 0.59mg intravitreal implant for treatment of pediatric ADNIV: a case study
Tiffany Nguyen BS, BA, Christopher Riemann MD, Arjun Sood MD
University of Louisville School of Medicine, Cincinnati Eye Institute, Retina Associates of Western New York
Investigating the Health Needs of Asiatown Community Members in Cleveland, Ohio
Sophie Lu*, MPH, Hanna Suh*, BS, Carvell T. Nguyen MD, PhD
Case Western Reserve University School of Medicine
Improving Vaccination Rates in Patients on Biologic Therapy for Dermatologic Conditions Through Provider Education
Carly Perkowski, Bailey Stammen MS3, Steven Robbe MD
Wright State University Boonshoft School of Medicine
Impact of Social Determinants of Health on Stroke Severity in Northwest Indiana
Grace Armstrong, Jacobus Barnard, David Lin, Miranda Cash, Neon Calumpang, Amy Han
Indiana University School of Medicine
Best of both worlds? Otolaryngology applicant perceptions of hybrid residency interviews
Melody Y. Zhou, Nilam D. Patel, MD, Nina W. Zhao, MD, MAEd
Case Western Reserve University
Exploring the Relationship Between Sleep Disorders and Dementia Risk in Older Kidney Transplant Recipients
Brandon Chou, Yusi Chen, Jane Long, Yiting Li, Nidhi Ghildayal, Sunjae Bae, Dorry Segev, Mara McAdams-DeMarco
University of Louisville School of Medicine
Exploring the Socio-Demographic and Behavioral Drivers of Neurodegenerative Readmissions in Northwest Indiana
Neon Calumpang, Grace Zhou Armstrong, Jonathan Guerrero PharmD, Baraka Muvuka PhD, Kyle Gospodarek MD
Indiana University School of Medicine
Deterministic Barcoding of Neuron Identities through Multicolor Fluorescent Markers in C. elegans
Seung Hyeon Shim, Yangning Lu, Edward S. Boyden
Case Western Reserve University School of Medicine
The Diagnostic Performance of the Curtain Sign Using Lung Ultrasound Compared to Computerized Tomography Chest Diagnosis of Pleural Effusion.
John-Matthew Ang and Kahra Nix, MD
University of Louisville School of Medicine
Determinants of Self-Perceived Health in Teen LINK 2024 (Local Inventory of Needs and Knowledge)
Soowan Jeong, Sarah Ronis, MD, PhD
Case Western Reserve University School of Medicine
Racial and Ethnic Disparities in Ketamine and Esketamine Therapy for Major Depressive Disorder
Michael Liu BS, Rachel Branning DO, Austin Lee BS, Keming Gao MD, PhD
Case Western Reserve University School of Medicine
Barriers to Clinical Trial Participation in AAPI Communities in the Greater Cleveland Area
Alice Liu, Haitong Yu, Amy Zhou
Case Western Reserve University School of Medicine
LEPTIN AND CYTOKINE INTERACTIONS IN CHRONIC RHINOSINUSITIS: IMPLICATIONS FOR IMFLAMMATION MODULATION AND OBESITY
Kaelan Wong, BS 1,2; Jorge Arpi Palacios, MD 1,2; Mohamad R. Chaaban MD, MSCR, MBA 2
Case Western Reserve University School of Medicine
Deformity Parameters in Spinal Cord Stimulation
Crystal Xu, Eric Herring, Noah Yaffe, Jennifer Sweet, Michael Staudt
Case Western Reserve University School of Medicine
Gender disparities in bladder cancer diagnosis following hematuria or UTI symptom presentation
Edward Zhang, Jack C. Millot, Adithya Balasubramanian, Camilo Arenas-Gallo, Lauren Chew, Jacob McMann, Anyull D. Bohorquez Caballero, Stephen Rhodes, Jonathan E. Shoag
Case Western Reserve University School of Medicine
Late-Onset Steatocystoma Multiplex in an 87-Year-Old Male: A Rare Presentation Without Genetic Predisposition
Bailey Stammen, BS, Jaree Naqvi, MD, MS, MBA, & Julian Trevino, MD
Wright State University Boonshoft School of Medicine
Risk Factors for COVID-19 in Ohio: A Retrospective Study at the County Level
Young Jun Park MS3, Jeffrey B. Travers MD, PhD, Trevor J. Bihl PhD
Boonshoft School of Medicine
Feasibility of an At-Home Experimental Circadian Misalignment Induction for Adolescents
Nuha Syed, Dean W Beebe, Ph.D., Andrea L. Fidler, Ph.D., Stephanie J. Crowley, Ph.D., Nuha Syed
NEOMED
Early Mapping of Neurogenic Niche from Spatial and Single-Nucleus Sequencing on Adult Human Hippocampus
Tony Kim, Madeline Mariani, Cheick Sissoko, Andrew J. Dwork, Gorazd B. Rosoklija, Mark D. Underwood, Victoria Arango, J. John Mann, Maura Boldrini
Case Western Reserve University
Identifying Cardiac Dysfunction in Trauma Patients Using CT Imaging: A Pilot Study
Sin Lei (Lydia) Pui, A. Mahajan , T. Syphan , L. Walden , J. Goddard , G. Yerneni , I. Osman , S. Pui , Y. Hu , H. McKillen , G. Braybooks , A. Tran , A. Tkacenko , V. Shah , V. Ho , W. Baughman , A. Aneja , P. Ladha
Case Western Reserve University
Rate of myopia-related retinal detachments in the United States from 2018 to 2023
David Zhang, Jacqueline Shaia, Nadia Abbass, Rishi Singh MD, Katherine Talcott MD
Case Western Reserve University
Mutational Analysis of the Putative Lipid Transfer Protein YhdP in Escherichia coli
Michael Lee, Thomas J. Silhavy
Case Western Reserve University
Bone marrow aspirate and bone marrow aspirate concentrate: Does the literature support use in long-bone union and provide new insights into mechanism of action?
Austin Li, Andrew Moyal, MD; Austin Li, BSE; Jeremy Adelstein, MD; Tyler Moon, MD; Joshua Napora, MD
Case Western Reserve University
Fractal Features of the Left Atrium Associated with Atrial Fibrillation Recurrence After Catheter Ablation
Kevin Park BS, Golnoush Asaeikheybari MS, Abhishek Midya PhD, John Barnard PhD, Han Sun MSPH, Hyun Su Kim BA, Taylor Schilling MS, Rod S. Passman MD, MSCE, Ben B. Shoemaker MD, MSCI, Anant Madabhushi PhD, Mina K. Chung MD
Case Western Reserve University
A Retrospective Cohort Review of Genetic and Clinical Epidemiology of Inherited Retinal Degeneration (IRD)
Rolandson Le BA, Shelby Lands MS, Wei Wang MD, PhD
University of Louisville School of Medicine
Purple Urine Bag Syndrome: A Rare Hue in Medicine
Joyce Lee, Carly Perkowski, Roshin Papaly, MD, James Lamb, MD
Wright State University Boonshoft School of Medicine
Clinic Counts & Chlamydia Crisis: An Analysis of STI Services and Infection Rates Across Ohio and Its Neighbors (2016-2022)
Drewyer Meyers, Alexander Hull, Jeannette Manger
Wright State University Boonshoft School of Medicine
Risk of Bone Fracture and Dual-Energy X-Ray Absorptiometry Screening Rates in Lung Cancer Survivors
Ilene Trinh, Jaime Abraham Perez, PhD, Elleson Harper, BS, Lauren Chiec MD, Qian Wang, MD, MPH, Melinda Hsu, MD, MS
Case Western Reserve University School of Medicine
Assessing clinician confidence in Hepatitis B screening
Joyce Lee, Allison Chen, Erika Nguyen, Roma Amin, M.D.
Boonshoft School of Medicine
Outcomes Following Saucerization For Osteomyelitis in Obese Patients: A Comparison of 4,000 Patients
David Han BS, Andrew J. Moyal MD, Jeremy M. Adelstein MD, Robert J.
Burkhart MD, Tyler J. Moon MD, Raymond W. Liu MD, George Ochenjele MD, Joshua Napora MD
Case Western Reserve University School of Medicine
Investigating Predictive Value of Lesion Size, PSA Density, and MRI Volume for Detecting Clinically Significant Prostate Cancer
Tony Zhao MS, Anthony J. Pamatmat BS, Kaitlyn Malek MS, David Song BS, Gary Hollenberg MD, Eric Weinberg MD, Thomas Frye DO, Guan Wu MD, PhD, Hani Rashid MD, Tyler Seibert MD, PhD, Jean Joseph MD, MBA, Tom Osinski MD
Northeast Ohio Medical University
Differing Impacts of Facility Type on Long-Term Survival For Patients Receiving Hemicolectomy for Stage I-IIIC Early-Onset and Normal-Onset Colon Cancer
Jothsna Sabbasani, R,THUSAY and P. SILBERSTEIN
Wright State University Boonshoft School of Medicine
FUNCTIONAL IMPACT OF BCAA METABOLISM IN LIVER PATHOPHYSIOLOGY
Yea-Lyn Pak1, Sunha Park1, Shuxun Ren1, Chen Gao1,2, Yibin Wang3
1Department of Anesthesiology, University of California, Los Angeles, 2Department of Pharmacology and System Physiology, University of Cincinnati, 3Cardiovascular and Metabolic Diseases Program, Duke-NUS, Singapore
Case Western Reserve University School of Medicine
Demographic Disparities in the Epidemiology of Tenosynovial Giant Cell Tumor: A SEER Database Analysis
Felicia Tejawinata, BS; Ankit Mangla, MD
Case Western Reserve University School of Medicine
Bridging the Healthcare Gap: A Model for Culturally Competent Care through the Asian Women’s Health Specialty Clinic
Kelly Hao, Singyi Yen, Hannah Ong, Linbee Sayat, Jason Sayat
Ohio State University College of Medicine
National Board

Emily Chen
Region V Director
Wright State University Boonshoft School of Medicine
Logistics Coordinator

Sunshine Liu
Region V Director
Michigan State University College of Osteopathic Medicine
Communications Coordinator

Jordan Sontz
Region V Director
Michigan State University College of Osteopathic Medicine
Programming Coordinator

Jessica Hsueh
Membership Vice President
Georgetown University School of Medicine
Local Chapter Leadership

Amy Lin
Med Chapter President
Ohio State University College of Medicine
Communications Committee

Fumiya Abe-Nornes
Med Chapter Vice President
Ohio State University College of Medicine
Logistics Committee

Kelly Hao
Med Chapter Treasurer
Ohio State University College of Medicine
Communications Committee

John Huang
Med Chapter Community Outreach Coordinator
Ohio State University College of Medicine
Logistics Committee

Rita Suzawa
Med Chapter Mentorship and Development
Ohio State University College of Medicine
Programming Committee

David Kim
Med Chapter Community Outreach Coordinator
Ohio State University College of Medicine
Programming Committee

Sooho Myoung
Med Chapter First Year Liaison
Ohio State University College of Medicine

Jasmine Yang
Med Chapter First Year Liaison
Ohio State University College of Medicine

Jaden Zelidon
Ohio State University — Pre-Med
Programming Committee
Unpictured:
Joshua Jeyandran, Uyen Dao, Miguel Ramirez, Nathan Schiffler, Ethan Hsu, Eric Liu, Jessica Li
Contact Us
Questions? Email us at region5@apamsa.org
Thank you to our generous sponsors!











2024 Region VI Conference

Voices of Change: Stand Up, Speak Out
Saturday, October 26th, 2024
7:30AM-4:00PM CST
Medical College of Wisconsin
Registration Details
Register for General Admission tickets NOW! Last day is October 25th at 5:00PM CST! See the link below for more information and registration page.
APAMSA Region VI and the MCW APAMSA chapter are thrilled to invite you to the annual Region VI Conference hosted at the Medical College of Wisconsin (MCW) in Wauwatosa/Milwaukee. We are proud to host this event at our medical school, which serves as a gathering for all AANHPI people and communities in our region. Together we’ll celebrate our diverse backgrounds and challenge ourselves to be “Voices of Change: Stand Up and Speak Out” as a united AANHPI community.
Our theme emphasizes elevating and uplifting all perspectives, while enabling students to learn to become effective, thoughtful, and self-aware advocates. Throughout the conference, we’ll achieve this mission by engaging with influential speakers, participating in action-oriented workshops, resident panels, interactive breakout sessions, and showcasing the research contributions made by our APAMSA members.
This conference is also a valuable networking opportunity to connect with fellow medical students from our neighboring chapters. We strive to foster connections, uplift one another, and collectively share knowledge that bolsters our community. We look forward to welcoming you at MCW!
General overview of conference schedule!
7:30AM – Check-in and breakfast
8:30AM – Welcome Statement with Dr. Li
8:45AM – Keynote with Dr. Sayyad
9:15AM – APAMSA Health Affairs
9:45AM – First Breakout Session *
10:55AM – Second Breakout Session **
12:00PM – APAMSA Sponsors
12:00PM – LUNCH
1:00PM – Research Poster Presentations
2:40PM – Resident Panel
3:45PM – Closing Statement, Raffles, and Awards
* First Breakout Sessions
- “Mental health and re-writing stereotypes in the AANHPI community” with Dr. Agrawal
- “Discuss burden of CV disease in South Asian Communities” with South Asian Heart Association
- IUD workshop
- Suture workshop
** Second Breakout Sessions
- HAAPIE Curriculum – Culturally Competent Care and Integrating Health Curriculum
- “Mental Health and re-writing stereotypes in the AANHPI community” with Dr. Agrawal
- IUD workshop
- Suture workshop

Anjum Sayyad, MD, MBA, FAAPMR
Keynote Speaker
Associate Chief Medical Officer, Froedtert Hospital
Associate Professor, Department of Physical Medicine and Rehabilitation
Medical Director, Brain Injury Medicine, Froedtert Hospital and Medical College of Wisconsin

B U.K. Li, MD
Welcome Statement
Emeritus Professor of Pediatrics (GI)
Past-President North American Society for Pediatric Gastroenterology, Hepatology and Nutrition
Co-Founder national Asian Pacific American Medical Student Association

Himanshu Agrawal, MD
Mental Health and Re-Writing Stereotypes in the AANHPI Community Workshop & Research Poster Judge
Department of Psychiatry and Behavioral Medicine

Maya Safarova, MD
Research Poster Judge
Department of Medicine, Division of Cardiovascular Medicine
she/her/hers

Sophie Shay, MD
Research Poster Judge
Department of Otolaryngology
she/her/hers

Priyanka P. Shah-Basak, Ph.D.
Research Poster Judge
Assistant Professor
Director, Cognition and Brain Stimulation lab
Departments of Neurology & Biomedical Engineering
Co-Director, Basic to Translational Scholarly Concentration
she/her/hers
Directions to the Venue
The conference location is at the Health Research Center at MCW. This can be directly routed to via GPS.
Parking can be found on the east side of 87th Street. (Marked as “MCW Visitor and Staff Parking” on the map.)
Entrance to the Health Research Center is directly west of the parking structure across 87th Street. (Marked as “Building A” on the map.)
For Uber/Lyft, there is a road that takes you directly in front of the Health Research Center and you could be dropped off there.
Clearer images and instructions can be found on MCW’s website. Please click on the link for more information!
Campus Map
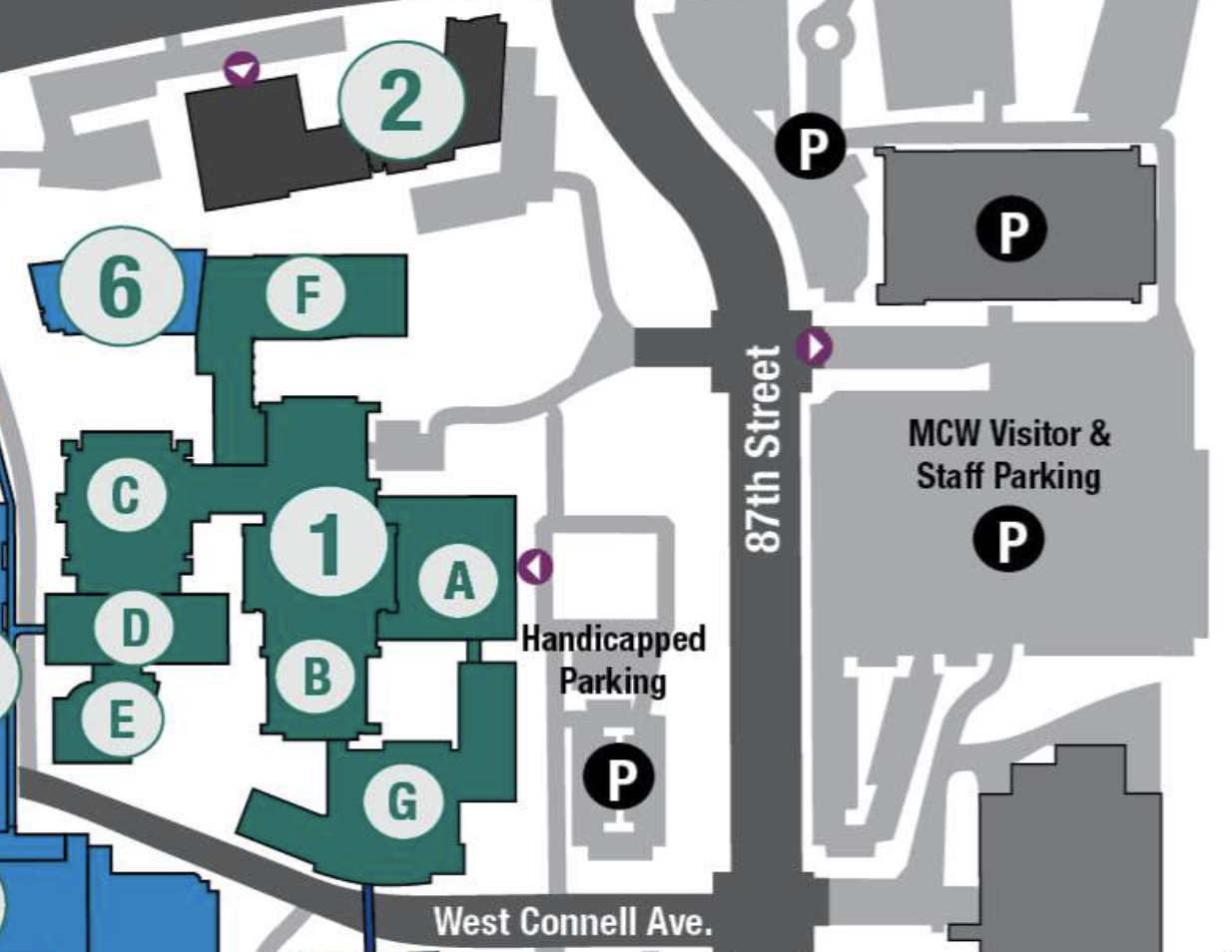
Accommodations and Recommendations
Staying for more than just a day for the conference?
Click on the link for budget friendly accommodations!! You can also find restaurants in the area or fun things to do in Milwaukee!
Featured Abstracts and Accepted Posters
Deniz Demircioglu, BS; Lou-Anne Acevedo Moreno, MD; William A. Hall, MD
Adileen Sii, MS-2; Maya Seshan, MS-2; Anjum Sayyad, MD; Lana M. Minshew, PhD; Kajua B. Lor, PharmD
Jany Sun, MS-3; Jim Boliboun, BS; Katherine Koo, MS-HSM; Valeria Vazquez-Trejo, MS-4; Michael Cui, MD, MS, MBA; Victoria Rizzo, PhD, LCSW-R; Jeannine Rowe, PhD, MSW
Luat Le, BS, Alexander J. Acuña, MD, Enrico M. Forlenza, MD, Joel C. Williams, MD
Rishi Kondapaneni, MS-2; Carson Gates, MS-3; Patrick Toerner Tassone, MD MS; Vipul Bhanderi, MD
Kaitlin Sung, MS-3; Dr. Marwah Farooqui, DO
Jieon Kim, M2; Prince Kumar, Postdoctoral Fellow; Pawan Singh, Principal Investigator
Sarah Kee, MS-2; Kevin Keuper, MD
Ian Rodriguez, M2; Sarah Melin, MPH; Jazzmyne A. Adams, MPH, David R. Friedland, MD, PhD; Sophie G. Shay, MD
O Aung, MS-2; Xiaolong Wang, MD, MS; Ruyu Yan, PhD; Peter J Rossi, MD, FACS; Mitchell R Dyer, MD, MSc; Yiliang Chen, PhD; Brandon Tefft, PhD; Kant Y Lin, MD, FACS; Bo Wang, PhD, MS, DDS
Shravani Khisti MS-2, Witty Kwok MS-2, Vikas Munjal MS-4, James Xiao, Joshua Weinberg PGY-4, Andrew Grossbach MD
Shravani Khisti1, Nikitha Damisetty, Yuefeng Lin, Dr. Ann Paula Monaghan-Nichols
Brian V. Li, Carson Gehl, Kaitlyn Nimmer, Tahseen Shaik, Kali Quade, Yun Xing, Xin Yang, Sarah Kerns, Anai N. Kothari
Snigdha Kosuri, MPH, MS-1; John Meurer, MD, MBA; Constance Gundacker, MD, MPH
Laurel X Chen MBE; Jian Zhang PhD; Jennifer S Yauck MS MA; Gail Stendahl APNP; Steven Kindel MD; Ke Yan PhD; Margaret M Samyn MD MBA
Tejas C. Sekhar, BA; Jessica S. Park, BA; Jessica Kulawiak, PharmD; Colleen B. Nash, MD, MPH
Alicia Wang, MS-2; Tarin Tanji, MS-2; Elaine Chen, MD
Nancy Jacobson MD, Elizabeth Papautsky PhD, MS, Matthew Scanlon MD, Brett Bordini MD, Katie McDermott PhD, Sarah Yale MD, Takahiro Ishikuri, Madelyn Anderson, Meagan Ladell MD
Tarin T. Tanji MS-2; Jae Young Heo, MD; Terrence Murphy, MD, MPH; Vivek Chaturvedi, MD
Hunjung Choi, MS-1; Jordan Parker, MD, FAAD
Lyiba Malik, MS; Amy Y. Phan, PhD; Andrew D. Spearman, MD
Tarin T. Tanji, MS-2; Michael Anukwu, MS-2; Jianing Tang, MS; Maria Gamez, BS; Lirong Yan, PhD
Kailynn Yang, MS-3, Canaan Kehr, MS-3, Mia Rumps, Mary Mulcahey MD
Kevin To, MS-2; Monika Pantha, MS-2; Scott Mead, MD
Allen Ku, MS-1; Branchford, MD;Deborah DeRyckere, Ph.D; Xiaodong Wang, Ph.D
Angelique Sumilang, MS-2; Maria Replogle, PhD; Kailey Frank, BS; Linda M Reis, MS, CGC; Elena V Semina, PhD
Kevin Truong-Balderas, MS-3, Hao Chen, MS-3, Sierra Thomas, MS-4, Erin X Wei, MD
Daniel Ma, M1; Sneha Anand, M3; Haile He; Alan Landay, PhD; James Moy, MD
Tejas C. Sekhar, BA; Qianyi Pu, MS; Ryan Guidi, MS; Nicholas P. Cozzi, MD, MBA; Kyle Bernard, MD; Eric P. Moyer, MD; Michael A. Gottlieb, MD; Galeta C. Clayton, MD
Qianyi Pu, MS-2; Bowen Li, OMS-I; Wenyuan Chen, BS
Aditya Somisetty BA; Hanna Shevalye, BS; Timothy Eggleston, BSE; Apurva C. Dusane M.Pharm; Jessica M. Skeie, Ph.D.; Gregory A. Schmidt, MBA, CEBT; Aliasger K. Salem, Ph.D; Mark A. Greiner, MD
Gabriella Tran, MS-2; Oscar Chen, MD, MS
Matthew Gao, M1; Andrea Benavides, BS; Josalyn L Cho, MD; Anna Stanhewicz, PhD
Spencer Pham, MS-1, Aravinthasamy Sivamurugan, MS-4, Satoshi Hanada, MD
Ashley Hong, MS-2, Don O. Kikkawa, MD, Marissa K. Shoji, MD
Christopher Jun, M2, Chad Grueter, PhD, Kayla Henry
Nicole Nowak, MS-2; Maria Mihailescu, MD; Kyle Amber, MD
Austin Stellpflug, PhD; Sameer Shakir, MD; Kaleb Keener, MS-2; Christopher Nguyen, MS-2; Milan Patel, MS-4; Kant Lin, MD; Bo Wang, PhD
Sherry Zhou, MD-PhD 5 (G3), Jim Maher, PhD
Kousalya Velagapudi, MS2; Patrick Hackett, MS; Stephanie Bustros, MD; Bornali Kundu, MD PhD.
Kauyen Chen, MS-2; Joel Jihwan Huang, MS-1; YeLeung Leini Huang, Undergraduate; Tsz King Donald Chow, MS-2
Sara Amini, BS; Fabrice Jotterand, PhD
Gabriella Tran, MS-2; Oscar Chen, MD, MS
Sonu Bhandari, MS-2; Margaret Kvale, MS-2; Alina Burek, MD
Joel Jihwan Hwang, MS-1; Echu Liu, PhD; Cornelius B. Groenewald, MB, ChB
Donald Chow, MS-2; Ethan Wang, MS-2; Amber Stefanski, MS-2; Sheyna Gifford, MD, MPH, MBA; Keniesha Thompson, MD, MS, FACP, FHM
Calista Bulacan, MS-2; Thomas Matoska, MD; Shravya Jasti; Anjishnu Banerjee, PhD; Lindsay Puckett, MD
National Board

Gautami Galpalli
Region VI Director
Southern Illinois University School of Medicine
She/Her/Hers

Vivian Hoang
Region VI Director
Kansas City University – Joplin
She/Her/Hers

Stephanie Ngo
Region VI Director
University of Kansas School of Medicine
She/Her/Hers

Nicholas Wu
Region VI Director
Saint Louis University School of Medicine
He/Him/His

Jessica Hsueh
Membership Vice President
Georgetown University School of Medicine
She/Her/Hers
Medical College of Wisconsin (MCW) Chapter Leadership

Adileen Sii
Co-President
she/her/hers

O Aung
Co-President
he/him/his

Maya Seshan
Hmong Community Health Chair
she/her/hers

Andrew Doan
Hmong Community Outreach Chair
he/him/his

Calista Bulacan
Secretary
she/her/hers

Chen Yu (Allen) Ku
he/him/his
Contact Us
Questions? Email us at region6@apamsa.org
2024 Region I & II Conference

Threads of Wellness: Weaving Community, Connectedness, and Cultural Humility within the AANHPI Experience
Date: Saturday, October 12, 2024
Location: Yale School of Medicine | Sterling Hall of Medicine
Registration Details: Click below for more info
000 days 00 hours 00 minutes 00 seconds
Conference Information:
Theme: “Threads of Wellness: Weaving Community, Connectedness, and Cultural Humility within the AANHPI Experience”
Date & Time: Saturday, October 12, 2024 | 9 AM – 5 PM
Location: Yale School of Medicine Sterling Hall of Medicine | New Haven, CT (333 Cedar St, New Haven, CT 06510)
Saturday, October 12th, 2024
| Event | Time |
| Check-in / Breakfast / Booths (Mary S. Harkness Memorial Auditorium / Rose Garden) | 9:00 AM |
|
Opening Statements / Introductions (Mary S. Harkness Memorial Auditorium)
Dean Marietta Vázquez / All of Us (AoU) / National Marrow Donor Program (NMDP) |
10:00 AM |
|
Keynote Address (Mary S. Harkness Memorial Auditorium):
Keynote Speaker: Victor Sta. Ana, MD, MSED, FAAFP |
10:45 AM |
| Breakout Session A | 11:30 AM |
|
Session 1: Out of Hospital Cardiac Arrest in Asian Americans: Current Issues & Local Solutions
Dr. David Yang, MD / Jasmine Jiang, MS3 |
Mary S. Harkness Memorial Auditorium |
|
Session 2: Never Enough: ADHD Experiences in Asian Americans
Dr. Zilin Cui, MD, EdM |
Sterling Hall of Medicine (SHM) 115 |
|
Session 3: Advancing Girl Empowerment and Women’s Health Equity in India
Dr. Ishita Sunita Arora, Ph.D., M.A.L.S. |
The Anlyan Center (TAC) Auditorium |
|
Session 4: Working with Limited English Proficient Patients and their Interpreters
Esther Lim |
Brady Auditorium |
|
Lunch / Research
Lunch: The Analyan Center Upper Lobby Courtyard | Rain Location: Cafe Med |
12:30 PM |
| Breakout Session B | 1:30 PM |
|
Session 1: WE Medicine: Convergence of Western and Eastern Medicine to Develop Future Medicines
Dr. Yung-Chi Cheng, Ph.D. |
The Analyan Center Auditorium |
|
Session 2: Spot the Signs, Stop the Cycle: Treating Eating Disorders in the AAPI Community
Registered Dietitian and Certified Diabetes Care and Education Specialist: Eling Tsai, MPH RD CDCES |
Brady Auditorium |
|
Session 3: Palpating Breath – An Osteopathic Approach to the Respiratory Patient
Dr. Jake Gallagher, DO |
Sterling Hall of Medicine (SHM) 115 |
|
Session 4: Mentorship: Stories of Asian Americans journeys in medicine
Dr. Joyce M. Oen-Hsiao, MD / Dr. Yingfei Wu / Dr. Barry Wu, MD, MACP |
Mary S. Harkness Memorial Auditorium |
| Breakout Session C | 2:30 PM |
|
Session 1: Inside the Mind of a Program Director: Navigating Residency with the Experts!
Dr, Ethan Daniel Fried, MD / Dr. Shwetha Iyer, MD / Dr. Timothy B. Sullivan, MD / Dr. Ingrid Walker-Descartes MD, MPH, MBA, FAAP |
Mary S. Harkness Memorial Auditorium + ZOOM |
|
Session 2: Liver “Transplantation and Medical Education”
Dr. Hiroshi Sogowa, MD, FACS |
The Analyan Center Auditorium |
|
Session 3: Balancing Points of View
Dr. Mina L. Xu, MD |
Brady Auditorium |
|
Session 4: Enhancing Cultural Competence: Addressing Mental Health Disparities in AANHPI Communities
Karen Chen, MS2 / Kanoe Evile, MS2 / Ted Shi, MS2 / Maya Xia, MS2 |
Sterling Hall of Medicine (SHM) 115 |
| Boba Break (Interactive BINGO) (Rose Garden) | 3:15 PM |
| Breakout Session D | 3:30 PM |
|
Session 1: Sew It Together: A Suturing Adventure
Dr. Hiroshi Sogowa, MD, FACS |
Sterling Hall of Medicine (SHM) 115 |
|
Session 2 (PRE-HEALTH): Creating Your Personal Roadmap into Medicine
Steve Paik, MD, EdM (Associate Dean for Student Affairs and Admissions at the Frank H. Netter MD School of Medicine at Quinnipiac University) |
The Anlyan Center (TAC) Auditorium |
|
Session 3: Medicine is a Noble Pursuit and Necessary to Sustain Life, But Art Is What We Stay Alive For
Dr. Andy Nguyen, MD |
Brady Auditorium |
|
Session 4: Residency Unlocked: Expert Guidance for Your Medical Journey & Insider Tips from Top Competitive Specialties!
Dr. Karen Bach, MD (Plastic Surgery) / Dr. James Hwang, MD (Radiology) / Dr. Arvin Saleh, MD (Anesthesiology) / Dr. Amanda Zhou (Dermatology) |
Mary S. Harkness Memorial Auditorium |
| Closing Remarks / Raffle (Mary S. Harkness Memorial Auditorium) | 4:30 PM |
| Conference Ending / Clean Up (Mary S. Harkness Memorial Auditorium) | 5:00 PM |
| Post-Conference Social (BAR New Haven) | 6:00 PM |
Keynote Speaker

Victor Sta. Ana, MD, MSED, FAAFP
Dr. Victor Sta. Ana (pronounced “Santa Ana”) is a family physician, Medical Director of Homeless Services at the Institute for Family Health, and Director of Icahn School of Medicine at Mount Sinai’s Primary Care Scholars Program. Dr. Sta. Ana graduated from Brown University with a concentration in Ethnic Studies and focus on Asian and African American literature. He subsequently earned a Master’s Degree in Education and taught Science and Special Education in the NYC public school system. In 2005 he changed careers to medicine, ultimately graduating from Albany Medical College and completing residency at the Institute for Family Health’s Beth Israel Residency in Urban Family Medicine. After residency he joined the faculty of the new Harlem Residency in Family Medicine where he continues to teach and provide patient care.
Since 2010, Dr. Sta. Ana has partnered with Damayan Migrants Workers Association, a grassroots organization dedicated to organizing low-wage Filipino workers, combating labor trafficking, promoting human and workers’ rights, and developing social justice leaders. Through his work with Damayan, he conducts worker health assessments in support of their applications for legal immigration status as survivors of labor exploitation. He has worked in community-based settings such as federally-qualified health centers, homeless shelters, food pantries, public schools and jails.
In 2015 he was chosen to direct Mount Sinai’s Primary Care Scholars Program for medical students interested in careers in primary care for underserved communities, and in 2021 he was promoted to Medical Director of Homeless Services at the Institute for Family Health. In this role he oversees five health centers for people with lived experience of homelessness. Dr. Sta. Ana also provides direct care at the Ali Forney Center for homeless LGBTQIA+ youth, and the Broadway Presbyterian Church for chronically homeless adults.
Dr. Sta. Ana has appeared in local and international news media advocating for domestic worker rights, advocated successfully at the state-level for homeless and runaway minors to consent to their own medical care, published, and has been invited to present locally, regionally and internationally on his clinical and advocacy work. Dr. Sta. Ana lives in Queens, NY with his partner and 3-year old.
Breakout Session A: Health Disparities

David Yang, MD
Dr. David Yang is a Clinical Instructor in the Department of Emergency Medicine. He earned his BS in Biomedical Engineering and BSAS in Electrical Engineering from Washington University in St. Louis, MD from LSU Health Sciences Center in New Orleans, and his MHS from Yale University. He recently completed his emergency medicine residency through the Yale Emergency Scholars Program and his Yale Emergency Scholar and Emergency Medical Services (EMS) fellowship.
Nationally, Dr. Yang has served as Mental Health Co-Chair for the Asian American Pacific Medical Students Association (APAMSA) and on the Equity and Inclusion Committee with the Society of Academic Emergency Medicine (SAEM). At the local level, he works closely with the sexual assault forensics committee and providing language concordant education to improve bystander interventions in cardiac arrest.
Dr. Yang’s current research focuses on addressing disparities of care in three domains. First, he examines the discrimination that healthcare workers face in the clinical setting with a particular focus on Asian Americans. Second, he focuses on improving the quality of care that survivors experience after a sexual assault. Third, he examines disparities in health outcomes and prehospital service utilization.

Jasmine Jiang, MS3
Jasmine is a third-year medical student at Yale School of Medicine. She earned her Bachelor’s degree in Biomedical Engineering from Vanderbilt University in 2021, with a second major in Medicine, Health, and Society. During her time at Vanderbilt, she founded the university’s Doctors Without Borders student chapter, focusing on serving both global and local communities. In Nashville, she established and developed public health workshops for local refugees with the goal of increasing health literacy on critical topics such as navigating the U.S. healthcare system and first aid.
Now in New Haven, Jasmine continues her commitment to community health by organizing Mandarin CPR workshops for local immigrants, training over 100 Mandarin-speaking individuals in the past year. She is passionate about improving community health and looks forward to integrating these efforts into her future career as a physician.

Zilin Cui, MD, EdM
Dr. Zilin Cui is a PGY-2 psychiatry resident at St. Elizabeth’s Medical Center in Boston, MA. She is interested in going into child and adolescent psychiatry. She graduated from UMass Medical School in 2023, and before that she completed my undergraduate studies at UChicago.
Contact information: Zilin.cui@bmc.org

Ishita Sunita Arora, Ph.D., M.A.L.S.
Dr. Ishita Sunita Arora (she/her/hers) is a Faculty member at the Department of Internal Medicine at Yale University School of Medicine and a Research Fellow in Community Evaluation and Youth Programming at the Research Institute for Structural Change, Michigan State University. Dr. Arora is a clinical, community, and applied social psychologist who works with underserved and marginalized populations in the resource-limited settings of South Asia and the United States. As a psychotherapist and research scientist, her healthcare services focus on four core areas – (a) advancing health equity and evidence-based policy for women’s, reproductive and maternal health, (b) promotion of girl empowerment and prevention of gender-based violence, (c) advancing anti-racism, diversity, equity, inclusion, and social justice, and (d) equitable access and utilization of mental healthcare among historically minoritized communities. Dr. Arora has expertise in community-engaged participatory research, mixed-methods research, program development and evaluation, implementation science, and violence prevention and intervention in academic medicine, community and not-for-profit organizations. Dr. Arora earned her Ph.D. in Human Services Psychology from the University of Maryland and a Master’s in Liberal Studies and Leadership from Ashoka University, India. Dr. Arora’s work is guided by anti-racist, anti-casteist, anti-oppressive, decolonial, and liberatory praxis.

Volunteer Health Interpreters Organization (Represented by Esther Lim, MS1)
Volunteer Health Interpreters Organization (VHIO) is a student-run organization at UC Berkeley that strives to eliminate language barriers in healthcare by providing free language interpretation and translation services in the San Francisco Bay Area. Over the past 17 years, we have worked with various healthcare organizations and medical schools to facilitate effective communication between providers and patients.
Many limited English proficient (LEP) patients do not have access to medical interpreters when they need the service, leading to lapses in understanding during the clinical encounter. A healthcare interpreter ensures that the patient and provider can communicate effectively, and in addition, acts as a cultural buffer and patient advocate.
Our presentation will explore what it means to have cultural competence vs. cultural humility when interacting with LEP patients of different cultural backgrounds, and how healthcare professionals can maintain a collaborative relationship with patients’ interpreters.
Contact information: cal.vhio@gmail.com
Breakout Session B: Alternative Medicine

Yung-Chi Cheng, Ph.D.
Henry Bronson Professor of Pharmacology and Professor of Medicine at Yale University School of Medicine, Academician of Academia Sinica and Connecticut of Academia of Science, Chairman and founder of Consortium for Globalization of Chinese Medicine (CGCM)
Professor Yung-Chi Cheng has been a leader in cancer and viral pharmacology. There are four approved drugs in Cytomegalovirus (CMV) and Hepatitis B (HBV), including the first anti-CMV drug, Gancylovillin and first anti-HBV drug, Lamivudine™ (3TC), discovered from his lab. Currently he has four additional drug candidates, including Chinese medicine PHY906 under clinical trials for the treatment of cancer, Hepatitis B Virus, and Human Immunodeficiency Virus (HIV). His leadership in antiviral and anticancer research has been recognized by his service as a member and Chairman of the Therapeutic Study Section of NIH, a member of the Board of Scientific Counselors of the Division of Cancer Treatment of the National Cancer Institute, and a member of the AIDS Research Advisory Committee of NIH, a member of the Board of Directors of the American Association for Cancer Research.
He is also chief consultant for many government and research institutions in Taiwan, mainland China and Hong Kong. He also holds honorary professors in more than 20 institutions in greater China. He is the founder of Society of Chinese Bioscientist in America which just celebrated 30 year birthday. He is also a consultant for many pharmaceutical firms and is the scientific founder of three biotechnology companies sponsored by Yale University, including Achillion who went public, PhytoCeutica who licensed its lead candidate drug PHY906, and Yiviva who is developing evidence-based botanical products to address aging-associated diseases. Throughout his career he has received numerous honors, including the Leukemia Society of America Scholar Award, the Rhodes Memorial Award from the American Association for Cancer Research, ASPET Award (Am Soc Pharm and Exp Therap), an Outstanding Investigator Award from the National Cancer Institute and Cheung on Tak Intl Award for Outstanding Contribution to Chinese Med among many others, Fellow of the National Foundation of Cancer research. He was the strategy consultant in biotech area for the Division of Science and Technology of Yunnan Province and has as academician working station in Quanming. He has received more than 10 honorary professor or doctor degrees from different institutes around the world.
Professor Cheng’s interests are in the development of new drugs and the improvement of the use of clinically proven drugs for the treatment and prevention of cancer, and cancer associated viruses such as herpes virus, human immunodeficiency virus or hepatitis B virus associated diseases. The types of agents are deoxyribonucleoside analogs, folate analogs and compounds that interfere with DNA and RNA metabolism. Currently he is interested in exploring the potential uses of Chinese medicines for unmet clinical needs.

Eling Tsai, MPH RD CDCES
Eling Tsai is a Registered Dietitian and Certified Diabetes Care and Education Specialist. She specializes in eating disorder treatment and prevention, weight-inclusive diabetes management, and family feeding. Eling received her Master of Public Health degree at the Yale School of Public Health and has experience in counseling and programming in a variety of settings, including private practice, hospitals, and community centers.
Eling uses a Health at Every Size® and Intuitive Eating approach to support her clients in improving their health, well-being and outlook around food. In addition to individual counseling, Eling enjoys educating groups about weight stigma, cultural competence in healthcare, and the joys of building a positive relationship with food and nutrition.

Jake Gallagher, DO
Dr. Jake Gallagher completed his residency at St. Barnabas Hospital in the Bronx, a level 1 trauma center and had the privilege of performing OMT on a variety of patients from newborns to acutely ill patients in the ICU. He was also in residency during the covid pandemic, and experienced treating patients with OMT in that setting. Currently, outside of teaching at Touro, he works at his private practice in Stamford, CT, where he see many patients with forms of chronic pain, often incorporating OMT with home exercise planning and mindfulness practices (thinking about somato-emotional types of pain) when appropriate.

Joyce M. Oen-Hsiao, MD
Dr. Oen-Hsiao is the Associate Professor of Medicine (Cardiovascular Medicine), Medical Director of Cardiac Rehabilitation at the Yale New Haven Health Heart and Vascular Center. She is a non-invasive cardiologist, focusing on women’s heart health, prevention, and general cardiology. She also sees patients in the office and also reads echocardiograms, nuclear stress tests, and cardiac CTs. She did her undergrad at Brown University and medical school at the Yale University School of Medicine.
Email: joyce.oen-hsiao@yale.edu

Barry Wu, MD, MACP
Barry J. Wu, MD, MACP received his BS degree in chemical engineering from Rensselaer Polytechnic Institute and MD from the University of Rochester. He completed his internal medicine residency at Yale New Haven Hospital. He is a Professor of Medicine and co-directs the first and last courses at Yale School of Medicine and recruits and trains 200 faculty involved in the clinical skills training and interprofessional education for medical, nurse practitioner and physician associate students. He co-directs the Connecticut Older Adult Collaboration for Health (COACH) 4M to enhance the geriatric workforce in primary care and is Chair of the Health Committee for the Yale China Association and collaborated on a model of residency training at Xiangya Hospitals adopted by the government of China. He is married with one son and faculty advisor for the Yale APAMSA Group, Yale ACP Internal Medicine Interest Group and Yale Health Professional Christian Fellowship. His email is barry.wu@yale.edu.

Yingfei Wu, MD, MPH
Yingfei Wu, MD, MPH completed her BS from the University of California, Los Angeles, MD from the Medical College of Wisconsin, and MPH from the Johns Hopkins Bloomberg School of Public Health. She trained in Internal Medicine at NYU Grossman School of Medicine and is currently a General Internal Medicine fellow at Harvard Medical School and Massachusetts General Hospital. Dr. Wu served on her local APAMSA chapter board at the Medical College of Wisconsin as well as on the APAMSA National Board, including as National President from 2018-2021. Her research experience ranges from basic neuroscience research and qualitative community surveys to systematic reviews and analyses of large clinical trials. Dr. Wu is passionate about primary care and clinical research in chronic cardiometabolic diseases, especially in addressing health inequities for minority/underrepresented populations.
Breakout Session C: Transplanting Dreams

Hiroshi Sogawa, MD, FACS
Dr. Hiroshi Sogawa is a multi-organ transplant surgeon, performing adult and pediatric liver, kidney, pancreas, and intestinal (multi-visceral) transplant, and hepatobiliary surgery (including robotic- assisted and laparoscopic liver resection and pancreas surgery). Dr. Sogawa has served as the associate director of adult and pediatric liver transplant. Prior to joining the medical staff at Westchester Medical Center, Dr. Sogawa served as Director of Abdominal Transplant Surgery Fellowship/Assistant Professor of Surgery at the University of Pittsburgh Medical Center, preceded by an appointment as Assistant Professor of Surgery at Icahn School of Medicine, Mount Sinai Medical Center.
A graduate of the Shiga University of Medical Science in Shiga, Japan, Dr. Sogawa completed residency in general surgery and gastrointestinal surgery at the Tokyo Women’s Medical University Hospital in Tokyo, Japan. Then he came to the US and completed a residency in general surgery at the State University of New York (SUNY), Stony Brook. Following residency training, Dr. Sogawa completed a multi-organ transplant and hepatobiliary surgery fellowship at Mount Sinai Medical Center. Dr. Sogawa also completed a research fellowship at Massachusetts General Hospital/Harvard Medical School for tolerance induction using mixed chimerism.
Dr. Sogawa is Professor of Surgery, Vice Chair of Education, and Surgical Clerkship Director at the Department of Surgery, New York Medical College. Dr. Sogawa’s research interests focus on improving post-transplant outcomes, induction of clinical immunologic tolerance in transplant recipients, safety and efficacy of living donor liver transplantation, intestinal transplantation, and minimally invasive (robotic and laparoscopic) hepatobiliary surgery. He is a member of numerous committees at national and international organizations as well as an editorial board member of major surgical journals.

Mina L. Xu, MD
Dr. Mina L Xu, MD, is the Director of Hematopathology and Professor of Pathology and Laboratory Medicine at Yale School of Medicine, specializing in diagnosing blood diseases and cancers. She is an internationally recognized academic pathologist and is also Director of Yale Pathology’s Expert Consultation Practice. Dr. Xu’s research focuses on the pathogenesis of hematopoietic malignancies, aiming to translate findings into diagnostic and therapeutic advancements in the field. Specifically, she is working on spatial multi-omics of lymphomas in transformation and in the development of novel cancer biomarkers.

Karen M. Chen, MS2
Karen Chen is a second-year medical student from Dallas, TX at the Columbia Vagelos College of Physicians and Surgeons (VP&S). She serves as the Columbia APAMSA chapter’s co-president. She is also the co-director of the Human Rights Clinic at Columbia. Karen graduated from Stanford University in 2022 with a B.S. in Computer Science and minor in Human Rights. Prior to medical school, Karen spent a year as Fulbright Research Scholar at Yonsei University in Seoul, South Korea, conducting global health research to develop novel corneal transplant hydrogel alternatives for use in low-resource areas. Karen is passionate about AANHPI issues, driven by her desire to address the healthcare disparities at home and abroad, and hopes to serve as a voice for the AANHPI community in future career in medicine.

Kanoe Evile, MS2
Kanoe Evile is a second year medical student at the Columbia University Vagelos College of Physicians & Surgeons. She grew up in the town of Haleiwa, HI on O’ahu in a Filipino-Samoan family that inspired her love for her community and Pacific Health. She completed her B.S. in Biological Engineering with a minor in Linguistics at MIT before entering the MD/PhD Program at Columbia. She is passionate about addressing Asian American, Native Hawaiian, and Pacific Islander (AANHPI) issues and looks forward to best serving these communities at the intersection of medicine and public health. Currently, she serves as the NHPI Director on the APAMSA National Board.

Ted Shi, MS2
Ted Shi is a second-year medical student at Columbia University Vagelos College of Physicians in Surgeons. He is originally from Overland Park, Kansas and attended The University of Texas at Dallas, where he received a bachelor’s degree in mathematics. In medical school, he serves as the social chair for the school’s APAMSA chapter, where he plans social events for the organization.

Maya Xia, MS2
Maya Xia is a second-year MD-PhD student at Columbia University Vagelos College of Physicians in Surgeons. She is originally from Houston, TX and graduated from Vanderbilt University with a bachelor’s in Neuroscience. Prior to starting medical school, she worked at the National Institutes of Health, where she studied mechanisms underlying PTSD in mouse models. At Columbia, she serves as the culture and education chair for the school’s APAMSA chapter.

Ethan Daniel Fried, MD
Dr. Ethan Daniel Fried is a graduate of the City College of New York, Sophie Davis School for Biomedical Education (a 7 year BS-MD program) and the SUNY Stony Brook School of Medicine. He completed his residency in Internal Medicine at SUNY Downstate-Kings County Hospital in Brooklyn and a fellowship in Pulmonary and Critical Care Medicine at the Cornell University Medical School – New York Hospital. He has a Master’s Degree in Clinical Epidemiology from the Harvard School of Public Health. He also has a Master’s Degree in Health Professions Pedagogy and Leadership from Hofstra University. Dr. Fried is currently Associate Chair for Education and Internal Medicine Residency Program Director at Lenox Hill Hospital, part of Northwell Health and Professor of Medicine at the Zucker School of Medicine at Northwell/Hofstra. He is also Associate Designated Institutional Official for Lenox Hill and Vice President of Academic Affairs at Northwell Health. In 2012, Dr. Fried was inducted as a Master of the American College of Physicians.

Shwetha Iyer, MD
Dr. Shwetha Iyer is Program Director of the Primary Care/Social Internal Medicine Program at Montefiore Medical Center/Albert Einstein College of Medicine. She received her medical degree from Temple University and completed her residency in the Primary Care/Social Internal Medicine Program Track at Montefiore. She developed and completed training as a global health faculty fellow in the Global Health and Clinical Skills Fellowship at Montefiore. Her area of interest includes medical education, specifically in curriculum development and coaching. She has adapted and teaches a weight management curriculum for residents, developed and co-directs the clinical reasoning curriculum, and has refined the advocacy and women’s health curriculum for the residency program. Her current curricular focus is the development of the Master Adaptive Learner model and structural competency in residency education. Prior to her current position, she served as Associate Program Director for the Primary Care/Social Internal Medicine Program.

Timothy B. Sullivan, MD
Dr Timothy B. Sullivan is Chair of the Department of Psychiatry and Behavioral Sciences and the founding Program Director of the Psychiatric Residency Training Program, from 2013-2023, at Northwell Health/Staten Island University Hospital (SIUH); and Associate Professor of Psychiatry at the Donald and Barbara Zucker SOM at Hofstra/Northwell. After graduating from Dartmouth Medical College, he trained in Internal Medicine and Hematology-Oncology at Saint Vincents Hospital in Greenwich Village, New York; and subsequently pursued further training in Psychiatry at the New York Hospital Westchester Division, Cornell University Medical Center, where he then served as a member of the faculty for several years.
Dr Sullivan is a Distinguished Life Fellow of the American Psychiatric Association; Fellow of the International Society for Affective Disorders; Co-Chair of the Psychotherapy Section of the World Psychiatric Association; Vice President of the World Association for Dynamic Psychiatry, a member of the Executive Council for the World Federation of Psychotherapy, and Associate Editor of Psychodynamic Psychiatry. He is also Chair of the Education Committee for the American Academy of Psychodynamic Psychiatry and Psychoanalysis (AAPDPP).
Dr Sullivan, throughout his career, has been active in the communities where he has worked, maintaining relationships with and frequently lecturing to NAMI, as well as serving for several years as First Vice President of the Board of Westchester Arc, and as a member of the Board of Governors of NYSARC. He currently serves on the Board of Partners Health Plan, a first-in-the-nation managed care organization focused on providing quality care for individuals with developmental disabilities.
In addition to founding the psychiatry residency training program at SIUH when he arrived there in 2011, he has subsequently, in his role as Chair, focused on modernizing systems of care and recruiting teaching faculty from distinguished institutions; collaborated with other hospital departments on a variety of projects, including Integrated/Collaborative Care models; developed programs that improve the recognition and treatment of persons with substance use disorders in primary care settings; promoted efforts to enhance behavioral care for individuals with Intellectual and Developmental Disabilities and their families; participated in community public health initiatives targeting underserved communities and populations at risk, especially adolescents; and helped begin hospital programs addressing resident and physician wellness. His current area of academic interest is the structure of future psychiatric practice and the training/educational needs of future psychiatrists, with an emphasis on proposed models of psychotherapy training.

Ingrid Walker-Descartes MD, MPH, MBA, FAAP
Dr. Walker-Descartes attended the University of Rochester School of Medicine & Dentistry where she obtained her Doctorate in Medicine. Upon graduating from medical school, she did a residency in Pediatrics at New York Methodist Hospital in Brooklyn, NY and subsequently pursued further training in a combined General Academic Pediatrics and Child Abuse Fellowship at Mount Sinai Hospital.
Dr. Walker-Descartes is currently on faculty at Maimonides Children’s Hospital of Brooklyn. In the Department of Pediatrics, she serves in two roles – one as a clinician and the other as an administrator. In her clinical roles, she practices General Pediatrics and a Child Abuse Pediatrics. As an administrator, she serves in the following roles: Program Director of the Pediatrics Residency training program, Fellowship Director for the Child Abuse Fellowship Program, the Vice Chair of Education for the Department of Pediatrics, and the Director of Child Maltreatment Services for the Children’s Hospital.
Dr. Walker-Descartes has published several articles as well as book chapters focused on the various forms of child maltreatment. Her involvement in child protection and advocacy also includes her involvement in several local and national professional organizations such as the AAP Chapter 2 Committee on the Prevention of Family Violence, the AAP Special Interest Group on Child Abuse and Neglect, the American Professional Society on the Abuse of Children (APSAC), the New York State Child Abuse Medical Provider Program (CHAMP) and the Ray Helfer Society for Child Maltreatment Pediatricians. She has also served as a consultant for the New York City Administration for Children’s Services Accountability Review Panel that reviews the child fatalities across the five borough and continues to lend her skillsets wherever possible to advance the healthcare agenda for all vulnerable children.
Contact: (718) 283-7503
Breakout Session D: Stitching Success

Steve Paik, MD, EdM
Steve Paik MD, EdM is the Associate Dean for Student Affairs and Admissions at the Frank H. Netter MD School of Medicine at Quinnipiac University.
He earned his MD at the Boston University School of Medicine. He completed his Pediatric residency training and Chief Residency at the Babies and Children’s Hospital at Columbia University. He then went on to complete a Pediatric Academic Fellowship in Urban Community Health at Columbia. During his fellowship, he earned an EdM at Teachers College Columbia University in Adult Learning and Leadership. Dr. Paik is Board Certified in Pediatrics and Pediatric Hospital Medicine, and he has served on faculty at NYU and Columbia as a Pediatric Hospitalist. He has served in pediatric residency leadership for 15 years (as Associate Program Director at NYU and Program Director at Columbia) prior to joining the Netter School of Medicine.
Dr. Paik has been an active member of the medical education community. He was in the first cohort of the Pediatric Academic Societies’ Educational Scholar Program. He has served as a faculty member for the Academic Pediatric Educator Excellence (APEX) Teaching Program. He currently serves as a member of the AAMC Advancing Holistic Principles Advisory Committee. His educational scholarly interests have included curriculum development and evaluation, faculty development, mentoring/coaching, professional identity formation, inclusive and equitable learning environments, skills development (teaching, feedback, conflict resolution, communication, and leadership).

Dr. Andy Nguyen, MD
Dr. Andy Nguyen, MD is a first year anesthesiology resident at Yale. As a first generation physician, he completed his undergraduate and medical school education through one of the inaugural cohorts of a combined BS/MD 7 year accelerated medical program at Augusta University and the Medical College of Georgia in Augusta, GA where he grew up. During his time in medical school, he used his more than decade long professional experience in photography and videography to merge digital media and medicine to build a social media platform culminating in over 300k in following and 50 million views across YouTube, Instagram, TikTok, and podcast streaming platforms. Most notably on YouTube (@ND M.D.) his 73Q interview series has created a library of resources that include testimonies from notable physicans of specialties ranging from psychiatry to plastic surgery such as Dr. America Revere, Dr. Jake Goodman, Doc Schmidt, Dr. Glaucomfleken, and much more. His experience traveling all around the country to share physician stories, directing and hosting multiple podcasts, using media experience to enrich medical school curriculum, and even being a TEDx speaker has been an example of the importance of maintaining creative passions in medical school and how important it is to share your story…because someone out there needs to hear it.

Dr. Karen Bach, MD
Dr. Karen Bach, MD, is a second-year plastic surgery resident at Yale. As a first-generation college graduate, she earned her Bachelor of Science in Physiological Sciences from UCLA. She then graduated from the University of Toledo College of Medicine in Ohio, where she was inducted into Alpha Omega Alpha and the Gold Humanism Honor Society. Karen’s involvement with APAMSA began during her premed years, where she served as the national bone marrow director. Later, during her medical training, she founded the local regional chapter at her medical school as served as President. Her professional interests include addressing healthcare disparities across different ethnic groups, microsurgery, and hand surgery. During her leisure time, she enjoys traveling with her fiancé, exploring the newest food scene, and hanging out with her cat.

James Hwang, MD
James Hwang is radiology resident at Yale University. He went to Duke University, where he studied biology with minors in Chemistry and Psychology. For medical school, he went to the Mayo Clinic Alix School of Medicine, which has multiple campuses. He was part of a program where I completed my first two years of medical school at the Rochester, Minnesota campus, and my clinical training years at the Jacksonville, Florida campus. Radiology requires a preliminary year, which he completed at Kaiser Permanente Hospital in Santa Clara, California. He is now in my first year at Yale, and he intends to complete a radiology fellowship in the future. In his free time, he enjoys spending time with my fiancé, friends, and family, along with traveling, both nearby and internationally. He is passionate about lifelong learning and mentorship and would love to connect with those with questions for him.
Contact information: james.hwang@yale.edu, Twitter @jameshwang214

Arvin Saleh, MD
Arvin Saleh is currently a CA1/PGY2 anesthesiology resident at Yale in New Haven. Arvin grew up in the US Pacific Northwest, Indonesia, and Singapore, before earning his undergraduate degree at Johns Hopkins in Baltimore. During his undergraduate studies, Arvin spent 4 months researching agriculture and nutrition policy in Nepal. Arvin then moved north to Boston to pursue his MD/MPH at Tufts. During this period, he spent a year living in Tanzania researching child growth and development outcomes. Arvin’s professional interests include global health, critical care, and pediatric anesthesiology. During his spare time, Arvin enjoys cooking, trying to cultivate a green thumb, and saving up to get more travel experiences. He can be reached at arvin.saleh@yale.edu.

Amanda Zhou, MD
Dr. Amanda Zhou is a PGY3 dermatology resident. She went to college at the University of Southern California and medical school at Yale. In medical school, she was involved in medical education, medical student wellness, the humanities in medicine, and basic science research in a dermatology lab studying skin cancer prevention. In residency, she is on the Clinician Educator track and continues to focus on medical education and wellness, including serving as a member of the Graduate Medical Education Committee and being a “Friend” in Yale’s “Call a Friend” one-on-one peer support initiative.
Directions to the Venue
- Tweed New Haven Airport (Served by Avelo Airlines)
- Local taxi service, M7 taxi (203-777-7777), is available at the airport, as are car rentals.
- Bradley International Airport
- Connecticut Limousine Service (https://ctlimo.com) and Go Airport Shuttle Connecticut (www.2theairport.com) service to New Haven is available from Bradley, Kennedy, LaGuardia, Newark, and White Plains airports.
- Union Station
- Amtrak – service is scheduled daily from Boston, Washington, D.C., or New York (Penn Station)
- Metro-North – Hourly service to New Haven from Grand Central Station in New York every day of the week
By car:
- From I-95 North or South Take Exit 47 (Route 34) to Exit 1. Visitor parking is available in the Air Rights Garage, which can be entered from MLK Jr. Boulevard, South Frontage Road, or York Street.
- From I-91 South Take Exit 1 (Route 34) to Exit 1. Continue to the Air Rights Garage, as above.
- From Merritt Parkway (Rte. 15) North Take Exit 57 to Route 34 East into New Haven. Turn right onto Ella T. Grasso Boulevard (Rte. 10) and then left onto South Frontage Road (Legion Avenue). Follow Yale New Haven Hospital and Rte. 34 signs. Continue to the Air Rights Garage, as above.
- From Wilbur Cross Parkway (Rte. 15) South Take Exit 59 immediately after the tunnel. Go right at end of ramp. Merge left onto Whalley Avenue at light. Stay on Whalley until you see signs for Yale New Haven Hospital at Park Street. Follow hospital signs, then make a left turn onto South Frontage Road. Continue to the Air Rights Garage, as above.
In need of funds? Apply for the APAMSA Diversity Travel Grant! Deadline: 9/20/2024
Campus Map (Click on Maps for Better Resolution)
Hotels and Accommodations
Apartments:
Hotels:
APAMSA Regions 1 and 2 invite you to submit an abstract for the Northeastern Regional Conference on October 12, 2024. There is no cost for submitting an abstract.
Deadline for abstract submission: September 28, 2024 @ 11:59 pm EST.
Submissions are now closed. Thank you all who submitted their abstracts. If you have not bought your ticket, please do so as soon as possible.
Research Prize Winners:
First Place: Su Htwe – Real World Application of Gene Therapy for Spinal Muscular Atrophy
Second Place: Justin Kong – Preschool mother-child emotional preparation program leads to significant improvement in autonomic regulation: a randomized controlled trial
Third Place: Ryan Yu – Prostate Cancer Characteristics and Outcomes for Medicare Recipients With and Without HIV
Featured Abstracts and Accepted Posters
Alexander Yu
Icahn School of Medicine at Mount Sinai
Poster #1:
Biportal Endoscopic Spine Surgery Shows Greater Reduction in Disability, While Uniportal Offers Faster Recovery in Lumbar Degenerative Disease: A Meta-Analysis
Alyssa Carlson
SUNY Downstate College of Medicine
Poster #2:
Acquired Hemophilia A Following SARS-CoV-2 Infection and Vaccination: Mechanistic and Clinical Insight
Eric Wang
Dartmouth Geisel School of Medicine
Poster #3:
A Culturally Relevant Approach to Nutrition Education: Chinese Heritage and Identity through Food And Nutrition (CHIFAN)
Ethan Wang
Yale School of Medicine
Poster #4:
Effectiveness of Mandarin-Language Workshop on CPR Skills in Chinese Americans Who Speak Mandarin As a First Language
Jefferson Poserio
University of New England College of Osteopathic Medicine
Poster #5:
Deletion of 11β-HSD1 Prevents Craniofacial Bone Loss Caused by Caloric Restriction
Jennifer Hong & Alyanna Tam
SUNY Downstate College of Medicine and Robert Wood Johnson Medical School
Poster #6:
Dismantling Structural Racism in Pediatric and Obstetric Clinics: Observing Health Disparities and Medical Mistrust
Jessalyn Li
Dartmouth Geisel School of Medicine
Poster #7:
Bridging the Digital Divide: Enhancing Digital Health Literacy through One-on-One Technology Coaching in Rural Living Communities
Ji Hyun Kim
New York Medical College
Poster #8:
Single-Surgeon Prospective Cohort Study: Comparing the Usage of Transanal Hemorrhoidal Dearterialization (THD) with Anolift, THD with Mucopexy, and Traditional Excisional Treatment for Grade IV Hemorrhoids
Joy Miao
Dartmouth Geisel School of Medicine
Poster #9:
Interventional Education in Cancer Prevention to Promote Sun Safe Habits and Lower Risk of Cancer in Rural Youth Populations
Joyce Quon
Yale School of Medicine
Poster #10:
Evaluation of CHATogether as a Creative Community-Based Intervention for Asian American Mental Health Needs: A Mixed-Methods Study
Justin Kong
SUNY Downstate College of Medicine
Poster #11:
Preschool mother-child emotional preparation program leads to significant improvement in autonomic regulation: a randomized controlled trial
Mehreen Pasha
University of Connecticut School of Medicine
Poster #12:
CFAP45, a heterotaxy and congenital heart disease gene, affects cilia stability
Paul Teng
New York Medical College
Poster #13:
Outcomes of Pediatric Patients Before and After RNS Thalamic Neurostimulation
Rebecca Chang
Yale School of Medicine
Poster #14:
Developmental Deconvolution of Pediatric Hepatoblastoma
Rithikaa Rajendran
Rutgers University
Poster #15:
Differential Roles of LPO Glutamatergic and GABAergic Neurons in Modulating Cocaine Reward and Aversion: Implications for Cocaine Use Disorder
Ryan Yu
Icahn School of Medicine at Mount Sinai
Poster #16:
Prostate Cancer Characteristics and Outcomes for Medicare Recipients With and Without HIV
Ryan Chan
New York Medical College
Poster #17:
Asian Representation in Kidney Transplant Clinical Trials
Sarah Ho
Yale School of Medicine
Poster #18:
Asian American women leadership in academic medicine: a qualitative study of medical residents’ perceptions of facilitators and barriers to leadership
Su Htwe
New York Medical College
Poster #19:
Real World Application of Gene Therapy for Spinal Muscular Atrophy
Sharon Yu
SUNY Downstate College of Medicine
Poster #20:
Utilizing Myeloperoxidase Staining and Clinicopathologic Correlation for Diagnosing Prurigo Pigmentosa Linked to Diabetic Ketoacidosis in New-Onset Type 1 Diabetes Post COVID-19
National Board

Melissa Calica
Region 1 Director
Tufts University School of Medicine

Stephen Lin
Region 1 Director
University of New England College of Osteopathic Medicine

Ruby Chung
Region 2 Director
SUNY Downstate
College of Medicine

Ker-Cheng (KC) Chen
Region 2 Director
SUNY Downstate College of Medicine

Yue Jiao Jiang
Region 2 Director
Touro College of Osteopathic Medicine Harlem

Sarah Lee
Region 2 Director
New York University Grossman Long Island School of Medicine

Paul Tominez
Membership Vice President
University of California, San Francisco School of Medicine
Local Chapter Leadership

Isabel Wang
Co-President
Yale School of Medicine

Emily Xu
Co-President
Yale School of Medicine

Ashley Wang
Event Planning Co-Chair
Yale School of Medicine

Tiffany Jiang
Event Planning Co-Chair
Yale School of Medicine

Rebecca Chang
Service and Conference Co-Chair
Yale School of Medicine

Joyce Quon
Service and Conference Co Chair
Yale School of Medicine

Javieer Singh
Treasurer
Yale School of Medicine

NEW APAMSA Skin Cancer Screening Toolkit
Rachel, our Cancer Initiatives Director of National APAMSA is promoting our brand new Skin Cancer Screening Toolkit launched earlier this year. It is packed with everything a local chapter needs to host their own skin cancer screening event. Here is the link if you’re interested: https://www.apamsa.org/skin-cancer-screening-protocol/
Chinese American Medical Society Events
FCMS & CAMS Scientific Conference on Health Care of the Chinese in North America on Saturday, November 2, 2024
Location: Pier 60 Chelsea Piers | NY
Save the date for the CAMS & CAIPA Red Lantern Gala on Saturday, November 2, 2024
Location: Pier 60 Chelsea Piers | NY
ASPIRE is starting its first Asian American cohort study for cancer research.
CLICK HERE to learn more.
Talk: The Alcohol Flushing Response
Dr. Eric Gross is an anesthesiologist at the Stanford School of Medicine, where his research laboratory focuses on the impact of genetic variants on perioperative organ injury. Taking a translational approach, the lab primarily investigates cardiovascular injury, with a current emphasis on aldehydes and the genetic variant responsible for inefficient aldehyde metabolism.
One common phenomenon related to this research is alcohol-induced facial flushing, where individuals experience redness and an increased heart rate after drinking. This flushing is linked to a genetic variant that leads to the accumulation of acetaldehyde, a harmful intermediate from alcohol metabolism. Traced back to the Han Chinese in Central China, this variant heightens health risks, including certain cancers, especially among those who smoke or drink. Additionally, it diminishes the effectiveness of nitroglycerin, a medication used during heart attacks.
Dr. Gross will discuss the genetic basis of alcohol flushing, its associated health risks, and the urgent need for greater education among medical professionals and the public. His research centers on aldehydes and their metabolism by the enzyme aldehyde dehydrogenase 2 (ALDH2), affecting nearly 540 million people worldwide. The significance of this work is evident in publications in prestigious journals such as Science Translational Medicine, Pain, BJA, Journal of Clinical Investigation, Redox Biology, and Physiological Reviews.
The NIH Medical Research Scholars Program (MRSP)
The National Institutes of Health Clinical Center, the world’s largest research hospital, continues the proud tradition of training the next generation of clinician-scientists. The NIH Medical Research Scholarship Program (MRSP) is a year-long residential professional development program for research-oriented medical, dental, and veterinary students at the NIH intramural campus in Bethesda, MD, as well as its satellite campuses.
The MRSP offers a robust investigational experience through a basic, clinical, or translational research project with an experienced mentor that matches their professional interests. Focused on helping develop a career in biomedical research, the MRSP year provides students with a dedicated advisor/mentor and a vast curriculum of academic activities featuring world-renowned clinician-scientists, networking opportunities, and professional development workshops. The NIH MRSP has a proven history of launching the next generation of clinician-scientists into highly successful, impactful careers.
Medical, Dental, and Veterinary students currently enrolled in their 2nd, 3rd, or 4th years with a strong interest in biomedical research are eligible to apply. Diversity strengthens our community and improves the quality of our training mission. We welcome and encourage applicants from all communities and backgrounds to apply. Applications must be fully completed and submitted by DECEMBER 2, 2024 at 5:00PM EST. **Please note the earlier application cycle and deadline this year. **
Students will be notified of their selection by mid-January. Interviews will take place February 18 & 19, 2025 during a 2-day virtual program that also includes informational sessions. Notifications of selection for the MRSP Class of 2025-2026 will be sent on February 28. The deadline to accept the offer will be March 7, 2025.
The NIH MRSP Team will conduct a live, virtual informational webinar on Thursday, October 10th at 1:00PM (EST).
Click Here to Register or go to Zoomgov.com Meeting ID: 161 702 4095 Passcode: MRSP2526 More information about our program can be found at: NIH Medical Research Scholars Program. If you have any questions or would like additional information about the MRSP, please do not hesitate to contact us at mrsp@mail.nih.gov.
Contact Us
Questions? Email us at region1@apamsa.org or region2@apamsa.org.
2024 National Conference

Blooming in the Desert
Date: March 1-3, 2024
Location: Kirk Kerkorian School of Medicine, 625 Shadow Ln, Las Vegas, NV 89106

Registration Details:
House of Delegates Registration – CLOSED
Banquet Tickets – CLOSED
Ticket Waitlist – CLOSED
Ticket Refund Request – CLOSED
Conference Tickets – SOLD OUT
Research Abstract Submission – CLOSED
Discounted Housing Form & Roommate Match – CLOSED
Hello everyone! On behalf of Kirk Kerkorian School of Medicine, we’re so happy to welcome you to Las Vegas for APAMSA’s 30th Annual National Conference!
In recent years, APAMSA National Conference themes have centered around boldly imagining the future and thoughtfully examining the past in order to bring our community together around the common goal of addressing healthcare disparities. Now we ask: How do we sustainably solve these challenges by employing the strengths that already exist within our communities and unify these efforts? This year, our theme is “Blooming in the Desert: Resilience, Adaptation, and Growth.” We want to emphasize mobilizing existing activism and local stakeholders to collaboratively and creatively meet these goals amid both seasons of monsoons and droughts. This theme is rooted in our chapter’s unique experience as a group of medical students at a young but eager university that was established to serve a rapidly growing city with ever changing needs. As we continue to learn how to “bloom” in these early stages to serve our own community, we recognize that countless communities across the country are doing the same. 2024 APAMSA National Conference is an opportunity for us to learn from each others’ experiences to shape AANHPI health across the country.
We’ve worked hard to bring in a variety of speakers who will graciously educate, inspire, and empower us to effect change and become better future community leaders.
We hope you will enjoy your time here building life-long connections, learning from each other, and exploring the City that Never Sleeps.
~ Nataliyah Tahir, Tiffany Chen, Eric Chio, Avery Zhou, Michelle Zhu, Kenny Do
2024 APAMSA National Conference Directors
Friday, March 1
Kirk Kerkorian Medical Education Building, 625 Shadow Lane, Las Vegas, NV 89106
5:30-6:30pm – Check in
6:00-8:00pm – Anti-Racism Caucus
Saturday, March 2
Kirk Kerkorian Medical Education Building, 625 Shadow Lane, Las Vegas, NV 89106
7:30-8:30am – Check in
8:30-9:05am – Welcome Address
9:05-9:50am – Keynote Address
10:00-10:45am – Breakout Session 1
11:00-11:45am – Breakout Session 2
11:45-12:50pm – Lunch, Diversity Mixer
12:00-1:45pm – House of Delegates (HOD) Meeting
1:45-2:45pm – Poster Session
3:00-3:45pm – Breakout Session 3
4:00-4:45pm – Breakout Session 4
5:00-5:30pm – Closing Ceremony, Election Results
7:30-10:00pm – Banquet (Ping Pang Pong)
Sunday, March 3
Kirk Kerkorian Medical Education Building, 625 Shadow Lane, Las Vegas, NV 89106
9:00-12:00pm – Transition Meeting for elected leadership
The 2024 APAMSA National Conference has secured discounted accommodations at The Linq Hotel & Experience on The Strip from Friday, March 1, 2024 through Sunday, March 3, 2024. The Linq is a 10 minute drive to the conference venue, the Kirk Kerkorian Medical Education Building! Shuttle services to the Kirk Kerkorian Medical Education Building will be provided for those reserving rooms with The Linq the morning of the conference.
The Linq Hotel & Experience: 3535 Las Vegas Blvd S, Las Vegas, NV 89109
Discounted housing is available on a first come, first served basis. Please sign up for this discounted housing here. This form also allows the option to request a roommate. Here are the important dates to lookout for:
January 1, 2024: Last date to sign up for Linq housing and/or roommates via the housing form
January 14, 2024: Group confirmations, details, and codes sent
January 31, 2024: Deadline to reserve your room
Cost: average $140/night (for 2 people, +$30 per additional person)
Fees: ~$30
Check out our transportation guide for tips on parking as well as how to commute from the airport to the conference venue, and around The Strip/Downtown!
Want more housing options? Check out our Las Vegas hotel guide for alternatives.

The 2024 APAMSA National Conference has secured discounted flights with United Airlines. Check out the infographic below for instructions on how to make your flight reservation.
2024 APAMSA NC United Airlines Booking Instructions
Abstract submission for the Research Poster Session is open until December 31st, 2023. Sign up here!
– Poster presentations are in-person and after lunch time during the conference (Saturday, March 2nd, 2024).
– Abstracts can be submitted into one of four categories: Basic Science; Translation & Clinical Health; Community Health, Epidemiology, Education, and Policy; and Healthcare Professional and Trainee Wellbeing.
– At least one author will need to be available at all times to give a quick oral presentation and answer questions during this session.
– There will be judges who will be selecting for the most outstanding abstracts in each category during the abstract presentation session.
Please note:
– Abstract approval decisions will be emailed to the corresponding author.
– Upon approval of submission, presenters will need to provide a demonstration of conference ticket purchase to confirm their attendance at this poster session.
– APAMSA unfortunately does not offer any poster printing services.
Feel free to contact research@apamsa.org with any questions!

Nataliyah Tahir
National Conference Logistics Director
Kirk Kerkorian School of Medicine

Eric Chio
National Conference Logistics Director
Kirk Kerkorian School of Medicine

Avery Zhou
National Conference Speaker Relations Director
Kirk Kerkorian School of Medicine

Michelle Zhu
National Conference Speaker Relations Director
Kirk Kerkorian School of Medicine

Kenny Do
National Conference Finance Director
Kirk Kerkorian School of Medicine

Tiffany Chen
National Conference Communications Director
Kirk Kerkorian School of Medicine

Logistics
National Conference Committee Members
Kirk Kerkorian School of Medicine
From left to right: Nataliyah Tahir, Michelle Zheng, Charissa Alo, Eric Chio

Speaker Relations
National Conference Committee Members
Kirk Kerkorian School of Medicine
From left to right: Kim Inciong, Avery Zhou, Michelle Zhu, Leah Yim

Communications
National Conference Committee Member
Kirk Kerkorian School of Medicine
From left to right: Allen Zhang, Tiffany Chen, Claire Ong
Not pictured: Celica Cosme

Finance
National Conference Committee Member
Kirk Kerkorian School of Medicine
From left to right: Gemma Lagasca, Kenny Do, Mira Dani
Thank you to our Sponsors!
For those who are interested in having an exhibitor booth at the National Conference, please contact conference@apamsa.org and CC externalvp@apamsa.org and sponsorship@apamsa.org in your email by January 26th, 2024 so that we can draft a sponsorship contract and create an invoice for you. Thank you for your interest!
2024 APAMSA NC Sponsorship Packet
Check out the National APAMSA Instagram to follow our speaker reveals! We will be introducing new speakers up until the conference!

Vivienne Hau, MD, PhD
Vivienne S. Hau, MD, PhD is a Clinical Assistant Professor with the Kaiser Permanente (KP) Bernard J. Tyson School of Medicine and a retina surgeon with the Southern California Permanente Medical Group. She is the Area Vice-Chair of Clinical Research and Director of the largest KP ophthalmology clinical research program focusing on age-related macular degeneration and diabetic retinopathy.
Dr. Hau is an openly transgender woman and first-generation Vietnamese boat immigrant. As a medical student she established the University of Arizona APAMSA chapter and later elected Regional Director and 2001 National President. Her chapter was one of the first to involve pre-med students. She is the first LGBTQIA+ elected board member of the American Society of Retina Specialists and currently co-chairs the DEI Committee and started the first LGBTQIA+ ophthalmology mentorship program. She’s an invited national speaker on supporting transgender and non-binary (TGNB) patients and colleagues and spoken to Fortune 500 companies on better supporting their TGNB communities. She was one of the first physicians to have transitioned at KP.
Dr. Hau is a mother to a beautiful 9-year-old daughter and her perfect day is taking her to Disneyland. She also volunteers guiding blind athletes in marathons and does triathlons.

Nolan Kagetsu, MD, FACR
Nolan studied chemical engineering at the Massachusetts Institute of Technology. After graduating from Albany Medical College (before the creation of APAMSA !), he completed a residency in diagnostic radiology at Mount Sinai West and a fellowship in Diagnostic and Interventional Neuroradiology at NYU. He currently is a diagnostic neuroradiologist at Mount Sinai in New York City. He advises the Mount Sinai APAMSA chapter. Nolan serves on the APAMSA alumni advisory board, the American College of Radiology (ACR) Commission for Women and Diversity, the board of the Association of University Radiologists, the Advisory Committee to the ACGME office of Diversity, and serves on the ACR Council Steering Committee. He has written about unconscious bias, microaggression, and being an upstander. He is a Professor of Radiology and Medical Education at the Icahn School of Medicine at Mount Sinai. He has 2 adult children and lives with his wife in New York City.
Kristine Jan C. Espinoza, PH.D. Candidate
Kristine Jan Cruz Espinoza is a Pinay Ph.D. Candidate studying Higher Education and completing a graduate certificate in Program Evaluation and Assessment at the University of Nevada, Las Vegas (UNLV). Her research interests revolve around race-based higher education policies, currently focusing on Minority-Serving Institutions (MSIs; i.e., Asian American and Native American Pacific Islander-Serving Institutions (AANAPISIs) and Hispanic-Serving Institutions (HSIs)) and racial data classifications. As part of her UNLV MSI Student Council initiative, she advocated for the systematic collection of disaggregated race data in the UNLV undergraduate and graduate admissions applications, which went into effect for Fall 2023 admits. She spoke on the importance of disaggregation of race data for Asian Americans, Native Hawaiians, and Pacific Islanders on Nevada Public Radio’s (KNPR) Exit Spring Mountain podcast. Before graduate study, Kristine worked full-time as the Student Affairs Officer in the UCLA Asian American Studies Department. She was a community college transfer student from Long Beach City College to the University of Hawaii at Mānoa, where she earned her B.A. in Biology, B.A. in Anthropology, and M.Ed. in Educational Administration.
Dr. David Kuykendall, MD
David Kuykendall is the current program director for the Kirk Krekorian School of Medicine Family and Community Medicine Residency. He leads the residency that trained him as a resident. Immediately after graduation he signed on as faculty and is now an associate professor with the school of medicine. He enjoys primary care and acute issues and loves medical education and community outreach.
Dr. Bernice Ponce de Leon, DO
Dr. Bernice Ponce de Leon, DO is a board-certified adult psychiatrist who recently completed a Child and Adolescent Psychiatry Fellowship at University of Southern California (2021-2023). She earned her BS in Psychology at Duke University, attended medical school at Touro University Nevada, and completed her adult psychiatry residency at University of Nevada Las Vegas. Her journey has been driven by her passion for Asian American mental health, from hosting outreach events to decrease mental health stigma in medical school, to serving as a Diversity Leadership Fellow with the American Psychiatric Association (2020-2022) as a resident/fellow. In her spare time, she enjoys watching Korean variety shows and crocheting.
Dr. Yingfei Wu, MD, MPH
Yingfei Wu, MD, MPH completed her BS in Neuroscience from the University of California, Los Angeles, MD from the Medical College of Wisconsin, and MPH in epidemiology and biostatistics from the Johns Hopkins Bloomberg School of Public Health. She completed her Internal Medicine residency at NYU Grossman School of Medicine and is currently a General Internal Medicine fellow at Harvard Medical School/Massachusetts General Hospital. She has served on her local MCW APAMSA chapter board as well as on the APAMSA National Board, including as National President from 2018-2021. Her research experience ranges from basic neuroscience research and qualitative community surveys to systematic reviews and secondary analyses of large randomized clinical trials. Dr. Wu is passionate about primary care and clinical research in chronic cardiometabolic diseases, especially in addressing health inequities for minority/underrepresented populations.
Dr. Ruey Hu, MD, MPH
Ruey Hu, MD, MPH is a cardiovascular outcomes researcher and third-year fellow in cardiovascular medicine at Yale School of Medicine. He was voted by Yale medical students as outstanding fellow teacher of the year in 2021, voted by Yale medical residents as the Department of Medicine’s 2022 Fellow of the Year, voted by APAMSA medical students as 2023 Alumnus of the Year, and voted by Yale emergency medicine residents as the 2023 Consultant of the Year. Originally from Canada, Dr Hu served as national president of APAMSA 2016-2018. He completed his AB at Princeton University, MD and residency at Vanderbilt University, and MPH in epidemiology and biostatistics at the Johns Hopkins School of Public Health, where he was inducted into the Delta Omega Public Health Honor Society. A metabolomics researcher, he is a two-time winner of the NKF National Young Investigators’ Forum. His research has been published in the Journal of the American Medical Association (JAMA) and Annals of Internal Medicine. His tool for guideline directed medical therapy, GDMT.org, has been recognized by the American Heart Association and is used by clinicians in 70 countries. He is an active peer reviewer for cardiology and nephrology journals and serves on the intern selection committee of the Yale internal medicine residency program.
Dr. Francisco S. Sy, MD, MS, DrPH
Dr. Francisco Sy is Professor & Chair, Department of Environmental and Occupational Health at UNLV School of Public Health. He is the Principal Investigator of Mountain West Clinical & Translational Research Infrastructure Network, funded by NIH/NIGMS. He is the Editor of AIDS Education and Prevention- An Interdisciplinary Journal since 1988. His research expertise include infectious disease epidemiology and health disparities research. Dr. Sy worked as a Senior Health Scientist Administrator at NIH National Institutes on Minority Health and Health Disparities Health for 12 years. At Centers for Disease Control and Prevention, he was a Senior Health Scientist in the Division of HIV/AIDS Prevention for 4 years. He was a member of the CDC SARS Outbreak Investigation Team in 2003. Dr. Sy was an Associate Professor of Epidemiology at University of South Carolina School of Public Health for 15 years. Dr. Sy earned his Doctor of Public Health degree in Immunology & Infectious Diseases in 1984 from Johns Hopkins School of Public Health; and Master of Science in Tropical Public Health in 1981 from Harvard School of Public Health. He obtained his MD in 1975 & BS Pre-Med in 1970 from University of the Philippines.
Dr. B U.K. Li, MD
Dr. B U.K. Li is an Emeritus Professor of Pediatrics at the Medical College of Wisconsin (MCW). He completed his A.B. (religion) at Princeton University, M.D. and internal medicine internship at Kansas University, and pediatric residency, chief residency, and gastroenterology fellowship at the University of Wisconsin-Madison. Over his career, he investigated the intestinal transport of carnitine, developed a 27-hour medical student diversity curriculum and a 3-year curriculum for 78 pediatric subspecialty fellows, studied the mechanisms of cyclic vomiting syndrome, and established the first interdisciplinary Cyclic Vomiting Syndrome (CVS) Program that treated national and international referrals. He was elected the first minority President (2008-2010) of the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition (NASPGHAN.org). He published over 160 articles and chapters and gave 80 Grand Rounds and international presentations. He chaired or co-chaired the Clinical Guidelines task force on the Diagnosis and Treatment of CVS in Children (2008), on the Diagnosis and Treatment of CVS in Adults (2019) and the ongoing pediatric update (2023). He co-edited the Fellows’ Concise Review of Pediatric Gastroenterology, Hepatology and Nutrition and serves as a Section Editor of Pediatric Gastroenterology for UpToDate. He received the Outstanding Clinical Teacher Award at the University of Wisconsin, three Diversity Awards from The Ohio State University, the MCW President’s Diversity and Inclusion Award (2018) and two career achievement awards in pediatric gastroenterology – the Murray Davidson Award (2012) and the inaugural Master Educator Award (2018). Dr. Li co-founded the Asian American Student Association at Princeton (1970) and the national Asian Pacific American Medical Student Association (APAMSA.org) in 1995 and continues on the advisory board. He has spoken to regional APAMSA Chapters and National Conferences and received APAMSA’s 10 th Anniversary Service and 25 th Anniversary Mentor Awards.
Dr. Kevin Riutzel, DO
Born in South Korea and raised in the greater Los Angeles area, Kevin Riutzel is a family physician currently working in the heart of LA’s Koreatown. The clinic he works at is a federally-qualified health center primarily serving local AAPI communities, many of whom are the 1st generation in their families to immigrate to the U.S. He has served in several roles for APAMSA including National President for three terms as well as National Pre-med Director, Region XII Director, and local chapter president. He finished his undergraduate studies at UC San Diego and graduate studies at Columbia University. After graduating from Touro University Nevada, he completed his training in family medicine at UC Irvine with a focus on integrative medicine. He served as one of the chief residents while at UC Irvine. Kevin takes a particular interest in mental health and culturally-sensitive nutritional counseling in AAPI communities along with providing an integrative and holistic approach to the care he offers to the communities he serves. He is not burned out, and he enjoys his job.
Dr. Hieu Pham, MD, MSPH, AAHIVS, FAAFP
Hieu Pham, MD, MSPH, AAHIVS, FAAFP (he/him) works at International Community Health Services (ICHS) in Seattle, WA as a Family Medicine Physician. ICHS is the biggest healthcare provider to AANHPI in Washington state. He provides full spectrum primary and obstetrical care to all patients, and serves as the in-house HIV specialist and gender affirming care subject expert. Additionally, Dr. Pham directs the ICHS Family Medicine Residency, a site of the larger Swedish Cherry Hill Family Medicine Residency (SCHFMR). As an immigrant, queer physician of color, Dr. Pham is particularly interested in immigrant and refugee health, LGBTQIA+ health, and mentoring the next generation of physicians of color. His other clinical interests include health equity, anti-racist framework in medicine, chronic hepatitis B, obstetrical and gynecological health, and diabetes. Dr. Pham was born in Saigon, Vietnam and was raised in Queens, New York. He did his undergrad at Columbia, Master’s at Johns Hopkins, and medical degree at Rush Medical College, where he was involved with APAMSA national board. He completed his residency in Family Medicine at SCHFMR, where he was also chief resident. Outside of work, Dr. Pham enjoys bouldering, reading, traveling, camping, board games, mixology, and cooking the food of his motherland. He is always in search for the best bún bò huế.
Dr. Winston Wong, MD, MS, FAAFP
A graduate of the UCSF School of Medicine, Dr. Winston Wong, MD, MS, FAAFP, is the Chair and acting CEO of the National Council of Asian Pacific Islander Physicians (NCAPIP). Dr. Wong was a founding member of NCAPIP when it was established in 2007 to provide a national voice for API physicians to advocate for health equity on behalf of their communities. Dr. Wong has served in national leadership roles in the U.S. Public Health Service and Kaiser Permanente, where he led population management efforts to address health disparities and to support Kaiser’s commitment to safety net providers. Dr. Wong has ongoing roles at the National Academy of Medicine, and in health philanthropy including the CDC Foundation and Grantmakers in Health. He is also a Scholar-in-Residence at the Kaiser Permanente UCLA Center for Health Equity. He was featured as a “Face of Public Health” in the American Journal of Public Health, and received the Community Hero Award from Asian Health Services based in Oakland, California.
Dr. Aakash Shah, MD
Dr. Aakash Shah is a practicing emergency room doctor who helped treat the earliest confirmed cases of COVID-19 in New Jersey. In addition to his clinical work, Dr. Shah has founded several programs to promote community health. Most recently, Dr. Shah founded Healing the Vote which helped recruit, train, and mobilize over 250 pre-health students to assist over 3,500 New Jerseyans to vote over the course of six weeks. He has also served as an advisor to the US Secretary of Health and Human Services and multiple federal, state, and local policymakers. Dr. Shah obtained his MD from Harvard Medical School, his MBA and MSc in Comparative Social Policy from Oxford University as a Rhodes Scholar, and his BA and BS from Ursinus College. He was awarded an honorary doctorate from Centenary University.
Dr. John T. Pham, DO
Dr. John T. Pham is the Dean and Chief Academic Officer of the University of the Incarnate Word School of Osteopathic Medicine. He formerly served as Vice Dean of Western University of Health Sciences College of Osteopathic Medicine of the Pacific Northwest in Lebanon, Oregon. He is an Associate Professor of Family Medicine and has a passion for teaching and inspiring the next generation of osteopathic physicians. Dr. Pham settled in Portland, Oregon with his parent and younger brother after emigrating from Vietnam in 1975. He is the eldest of three sons and the first in his family to attend medical school. Dr. Pham attended Oregon State University, where he majored in Biology and minored in Chemistry. After graduating from Oregon State University, he left the state for the first time since arriving in Oregon to attend medical school at Des Moines University in Iowa. Dr. Pham completed his residency in family medicine at the Eastmoreland Hospital. After graduating from residency, Dr. Pham was an ambitious and eager physician. His ambition and motivation to give back to his community was embedded in his fiber. He became an entrepreneur and opened a solo practice clinic in Portland, where he practiced for more than 9 years prior to joining WesternU in 2011. Being fluent in Vietnamese, Dr. Pham’s practice served a large number of first- and second-generation Vietnamese. Throughout his time in private practice, Dr. Pham mentored countless numbers of medical students and pre-med students at his clinic. Dr. Pham has been recognized for mentoring both locally and nationally. These acknowledgements have earned him D.O. of the Year from the State Association in 2010 and Mentor of the Year from the AOA in 2007. His love of teaching led him to Western University COMP-Northwest, where he began educating as an Assistant Professor of Family Medicine for the inaugural class in 2011. When the opportunity arose for him to give back to the community and train future compassionate and competent physicians, he did not hesitate. He now brings his passion for education and mentoring to the University of the Incarnate Word School of Osteopathic Medicine as Dean.
Dr. Jhemon Lee, MD
Dr. Lee is a private practice radiologist in Los Alamitos, CA. He was one of the original student organizers that helped lead to the formation of APAMSA in 1995, and has helped lead APAMSA’s Advisory Board ever since. He is a board member of the National Council of Asian Pacific Islander Physicians (NCAPIP). He is president of the Orange County chapter of OCA – Asian Pacific American Advocates, and has previously held many roles in the National Association of Asian American Professionals (NAAAP), including National President, President of its Chicago chapter, and co-chair of its 2008 National Convention. He is also the Medical Advisor for the Diagnostic Medical Sonography programs at Platt College. Dr. Lee received his bachelor’s degree in Engineering Sciences at Harvard University and obtained his medical degree from the University of Maryland. He completed his residency in diagnostic radiology at the University of Chicago, where he was chief resident, and a fellowship in abdominal imaging at Brigham and Women’s Hospital/Harvard Medical School in Boston. On the side, Jhemon writes and performs sketch comedy with the Asian American comedy group “No MSG Added,” and he and his wife previously performed improv comedy for years with groups such as Cold Tofu, Los Angeles’ longest running API improv troupe.
Dr. Sandhya Wahi-Gururaj, MD, MPH
Dr. Sandhya Wahi-Gururaj is a board-certified general internist and professor of internal medicine. Dr. Wahi has been in medical education for over 20 years across the continuum. She held multiple roles including program director for 12 years at the University of Nevada, Reno (UNR), now known as the Kirk Kerkorian SOM of at UNLV internal medicine residency program. Dr. Wahi has a keen interest in physician professional development and well-being, and among other activities she regularly presents faculty development sessions at the national level. . She is the Governor of the Nevada Chapter American College of Physician (ACP), a Well-being Champion Emeritus, and was the program planning chair for 11 years. In addition, she is an active board member of the Nevada Physician Wellness Coalition. Dr. Wahi is a recipient of multiple awards including the NV ACP’s Chapter Laureate Award, Woman Physician of the Year, and is a member of the Alpha Omega Alpha Honor Medical Society. She is a graduate of the Northwestern University Feinberg School of Medicine and the Boston University School of Public Health. She completed her internal medicine residency, chief residency, and general internal medicine fellowship at the Boston University Medical Center.
Dr. Marcus Kawika Iwane, MD
Dr. Marcus Kawika Iwane was born and raised in Hawaii on the island of Oahu. He earned his medical degree from the University of Hawaii, John A. Burns School of Medicine (JABSOM) in 2010. He continued his training at the University of Hawaii Internal Medicine Residency Program and is board certified in internal medicine. He belongs to the American College of Physicians, Hawaii Chapter and serves as president of ‘Ahahui ‘o nā Kauka, the Association of Native Hawaiian Physicians. In 2014, Dr. Iwane joined Hawaii Permanente Medical Group, where he practices internal medicine. He is the chief of the Kaiser Permanente West Oahu Medical Office at Kapolei, known as Kīpukaoha, where he leads a collective effort with community organizations to create innovative programs and partnerships that promote Native Hawaiian health and healing. He serves as clinical faculty for JABSOM, the Kaiser Permanente Bernard Tyson School of Medicine and the Kaiser Permanente Hawaii Internal Medicine Residency Program. In 2018, Dr. Iwane was named to Pacific Business News’ 40 Under 40 list of exceptional leaders. Most recently, he was recognized on the peer-nominated list Best Doctors in America® and received the 2021 Kaiser Permanente David Lawrence Community Service Award. In 2023, Dr. Iwane completed the Climate and Health Equity Fellowship through the Medical Society Consortium on Climate and Health.
Jennifer Young, MPA
Jennifer serves as the Director of Community Engagement at the Kirk Kerkorian School of Medicine where she also lectures on health policy, social determinants of health, health systems science and population health. She attended the University of Nevada-Las Vegas and graduated with a Bachelor in Political Science. After 20 years in healthcare she obtained a Masters in Public Affairs with a concentration in health policy from Indiana University. Currently she is pursuing a doctorate in public policy and her research focuses on identifying and addressing social needs in primary care settings.
Susan Choi
Susan has been associated with Be The Match since 2014, as the Director of Asians for Miracle Marrow Matches (A3M), a network partner organization based in Los Angeles and dedicated to engage and enroll potential donors from communities of color. Susan joined Be the Match in 2022 and currently serves as the Manager of Asian American, Native Hawaiian and Pacific Islander Partnerships and Patient Engagement. In this role, Susan manages community and collegiate partnerships with the goal of increasing aware of Be the Match’s mission and diversifying the registry. Susan also leads the Patient Engagement Program and organizes collaborative efforts with patients and the Be the Match recruitment team to explore and support recruitment opportunities.
Susan Choi is originally from Hong Kong and raised in Southern California. She holds a Master of Science degree in Environmental Health Science and Policy from the University of California, Irvine. She is a busy mom of three and could be found in a gym on weekends watching her boys’ basketball games.
Never been to Las Vegas, Nevada before? Come explore our city! Known as the city that never sleeps, there’s plenty of activities to do here and plenty of yummy food!
Check out our Exploring Vegas Guide (with clickable links) for ideas on how to make the most of your time here.
We’re excited to announce that applications for the 2024-2025 National Board are now open.
We’re calling for candidates to apply by Sunday, February 18th, 2024 @ 8:59pm PST/11:59pm EST. If you are looking for opportunities to join the national leadership at our organization, this is your chance! You can find more information about how to run for the 2024-2025 National Board by visiting https://www.apamsa.org/elections/.
The annual APAMSA National Board Election is held every year during the week of the National Conference, and is an opportunity for APAMSA student members across the nation to get involved in the organization’s leadership.
Election Day: Saturday, March 2nd, 2024
Applications Deadline: Sunday, February 18th, 2024 @ 8:59pm PST/11:59pm EST

Contact Us
Questions? Email us at conference@apamsa.org.
.